The disorder can greatly impact patients’ quality of life, but sclerotherapy and a multidisciplinary approach to care can be life-changing
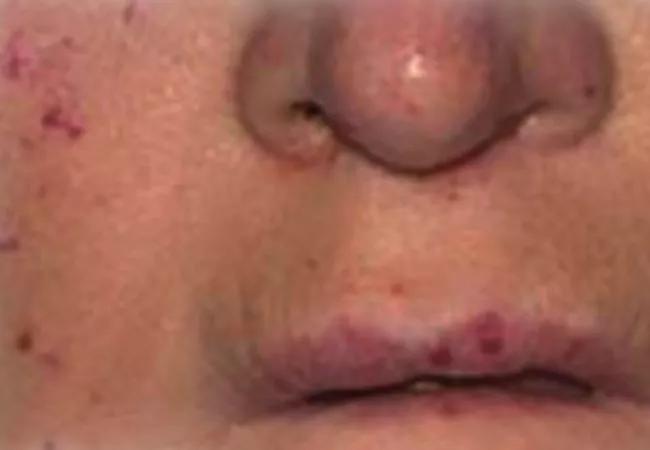
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7c6b0bdf-e6c0-4102-aaf4-3a3a6862c6b1/23-HNI-3732983-ContemporaryManagement-HHT-CQD_650x450_jpg)
HHT
Hereditary hemorrhagic telangiectasia (HHT) is a genetic bleeding disorder that can seriously impact patients’ quality of life. Patients typically have frequent, severe nosebleeds as well as bleeding and lesions in other body systems. However, advances in treatment and a multidisciplinary approach can successfully manage this condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Before they get treatment, many patients are confined to the house because they’re afraid they’ll develop a nosebleed,” says Troy Woodard, MD, a Rhinology, Sinus, and Skull Base Surgeon at Cleveland Clinic’s Head & Neck Institute. “I had a chef who couldn’t work anymore because he would bleed when he prepared food. I’ve had attorneys talk about getting blood on their legal papers. It’s bad.”
Cleveland Clinic is an HHT Center for Excellence, and Dr. Woodard, the president-elect of the American Academy of Otolaryngology-Head and Neck Surgery, is a leader in the management of HHT. He has helped to develop novel medical and surgical therapies that have improved outcomes. Dr. Woodard has presented widely on his work, including recently at the 2022 American Academy of Otolaryngology—Head and Neck Surgery annual meeting.
A characteristic sign of HHT is small red spots on the face caused by ruptured capillaries. While nosebleeds are one of the most common symptoms, HHT can also cause gastrointestinal bleeding, and in some cases, it can cause life-threatening bleeds in the lungs, liver and brain. Along with causing disruption to patients’ lives, these frequent bleeds can lead to fatigue and anemia, and some patients require regular iron or blood infusions.
Traditionally, HHT nosebleeds have been treated with laser therapy and cautery, which does work to stop bleeding, but produces only short-term results. Instead, Dr. Woodard prefers to treat patients with sclerotherapy, a vein-hardening injection commonly used to treat varicose veins.
Advertisement
Dr. Woodard conducted a study comparing laser and cautery with sclerotherapy and found that both treatments reduced nosebleeds. However, patients who received sclerotherapy needed only around two procedures in a two-year period, while patients who received the traditional therapies needed up to eight.
“It’s really changed our patients’ quality of life,” he says.
Typically, Dr. Woodard first tries to manage HHT patients with medications, including topical therapies like timolol or topical Avastin to reduce bleeding, or Tranexamic acid to stop severe bleeds. Some patients may also be treated with systemic medicines like Avastin or Votrient.
“We usually try it for a good couple of months,” he says. “However, if the bleeds persist and worsen, we want to move on to other treatments as soon as possible. We don’t want the patient passing out or fainting from blood loss.”
Dr. Woodard also collaborates with other specialists to treat bleeding in other areas, including gastroenterologists who use endoscopy or colonoscopy to treat GI lesions. He says a multidisciplinary approach is key to managing HHT.
“Because this disease can affect multiple organ systems, we have doctors who specialize in those particular areas,” he says. “We all work together so the patient can get comprehensive treatment.”
While more invasive surgical options have been tried, Woodard noticed they have significant negative side effects. One approach involves removing the lining from the inside of the nose and replacing it with a skin graft.
Advertisement
“The problem with that is that people will still develop lesions underneath the new graft, so it kind of makes it even harder to manage,” he says.
In some severe cases, surgeons will close off the entire nasal cavity to prevent air from drying the nasal lining and causing blood vessels to rupture.
“Yes, it tends to decrease the nosebleeds, but you won’t be able to smell anymore,” he says. “You have to change the way you breathe and deal with consequences like dry mouth. So there’s a downside.”
Physicians who don’t normally treat HHT should know that these patients should be screened for arterial venous malformations in the brain, lungs and liver. These abnormalities can rupture undetected and cause death. “If they’re not comfortable with that screening, they can send the patient to an HHT center,” says Dr. Woodard.
While HHT can cause severe quality of life issues, Woodard says treatment and management can make a real difference. He recalls one patient who had been confined to his home due to nosebleeds and was getting blood transfusions and iron infusions multiple times a month. With treatment, he’s been able to travel again, including visiting locations with limited medical access. “He went to Antarctica. He’s gone on Safari,” Woodard said. “It really has changed his life because he couldn’t even go across town before.”
Podcast content: This podcast is available to listen to online.
Listen to podcast online (https://www.buzzsprout.com/2241209/13504200)
Advertisement
Advertisement
Exploring the true prevalence of AATD among Americans and why so many remain undetected
Recommendations on identifying and managing neurodevelopmental and related challenges
Phenotypic clustering study reveals four distinct disease trajectories
Rare genetic disorder prevents bone mineralization
Oral medication reduces epistaxis and improves quality of life for patients with rare vascular disorder
A recently published case series highlights the broad range of laryngeal findings that can present among individuals with EDS
Cleveland Clinic report shares details and outcomes of novel technique for open repair
National database study reveals insights into survival outcomes