Minimally invasive surgery is effective for uveitic and steroid-induced glaucoma too
The tube shunts used in conventional uveitic glaucoma surgeries can cause cornea damage, exposure, diplopia and, in uveitic eyes, late recalcitrant hypotony, says Jonathan Eisengart, MD, a glaucoma specialist at Cleveland Clinic Cole Eye Institute. However, minimally invasive glaucoma surgery (MIGS) may eliminate these risks.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“In our experience, the newer MIGS procedures have been safer, quicker and more effective for uveitic and steroid-response glaucoma than conventional glaucoma surgeries,” he says.
That anecdotal insight inspired a recent study of 24-month outcomes in patients with steroid-induced or uveitic glaucoma undergoing MIGS. Researchers retrospectively reviewed the charts of patients who had either gonioscopy-assisted transluminal trabeculotomy (GATT) or excisional goniotomy (with Kahook Dual Blade) at the Cole Eye Institute between 2016 and 2020. The study, published in Journal of Glaucoma, included 40 eyes of 33 patients who underwent GATT and 24 eyes of 22 patients who had goniotomy. Of these, 88% of GATT patients and 75% of goniotomy patients received 24 months of follow-up.
In the study, 38% of the GATT eyes and 17% of the goniotomy eyes had concomitant phacoemulsification cataract surgery. Though concurrent MIGS and cataract procedures are common in eyes with noninflammatory glaucoma, Dr. Eisengart says the patients with uveitic eyes in his study were different: They had complicated disease, and the focus was on addressing multiple issues.
“The choice between goniotomy and GATT was not dependent on whether cataract surgery was being performed but was based on other considerations, such as how high the pressure was, what prior surgeries had been done on that eye, the status of the iridocorneal angle and the vision in the other eye,” says Dr. Eisengart.
Outcomes of the MIGS procedures didn’t seem to be affected by concurrent cataract surgery. The procedures were similarly successful. Among the study’s results, 24 months after surgery:
Advertisement
“These surgeries are so much safer and in many cases as effective or more effective than tube shunts,” says Dr. Eisengart. “Many ophthalmologists still consider goniotomy and other MIGS procedures only for patients with mild to moderate primary open-angle glaucoma. This study demonstrates that these procedures can benefit a wider range of patients and disease conditions, particularly patients with secondary open-angle glaucoma in which trabecular dysfunction is thought to be the primary cause of elevated IOP.”
Another important — and unanticipated — finding was that 24 months after these procedures, the eyes receiving ongoing steroid treatments had similar IOP to eyes without continued steroid exposure.
“In other words, you can continue treating patients with uveitis with the steroids they need to save their vision without the risk of raising their eye pressure,” says Dr. Eisengart.
The primary postoperative complication in the study was transient hyphema, which affected patients who received GATT more than those who had goniotomy.
“Hyphema can cause transient high IOP and can significantly blur the vision,” says Dr. Eisengart. “IOP spikes can occur unexpectedly as well, typically two to four weeks postoperatively. Usually these spikes are transient and respond to medication.”
Within the first month after surgery, 21 of the 40 GATT eyes (53%) had hyphema present at some point, while only 1 out of the 24 goniotomy eyes (4%) did. One month after surgery, persistent hyphema was reported in 3 of the 40 GATT eyes and in none of the 24 goniotomy eyes.
Advertisement
Within the first month after surgery, 8 of the 40 GATT eyes (20%) experienced transient IOP elevation higher than 30 mm Hg, while 4 of the 24 goniotomy eyes (17%) did. However, sustained IOP elevation — defined as higher than 21 mm Hg at two consecutive visits before the first month after surgery — was found in only 1 of the 40 GATT eyes and 2 of the 24 goniotomy eyes.
Surgical failure was 8% for GATT and 14% for goniotomy at 24 months.
“Many times there isn’t any visible anatomic reason for failure of the surgery,” says Dr. Eisengart. “In those cases, it typically makes sense to move on to a tube shunt, although other traditional glaucoma surgeries may be indicated depending on the patient’s exam and history.”
Dr. Eisengart believes that this study’s findings could change clinical care.
“Ophthalmologists should consider these MIGS procedures for their patients with steroid-induced or uveitic glaucoma,” he says. “I strongly believe that these procedures will become first-line therapy and the standard of care in the surgical management of uveitic glaucoma.”
Advertisement
Advertisement

Prescribing eye drops is complicated by unknown risk of fetotoxicity and lack of clinical evidence

A primer on MIGS methods and devices

7 keys to success for comprehensive ophthalmologists

From medication to laser treatment to surgery

Tissue remnants seem unrelated to clinical outcome

Prematurity is linked with poorer outcomes of retinal surgery in adulthood
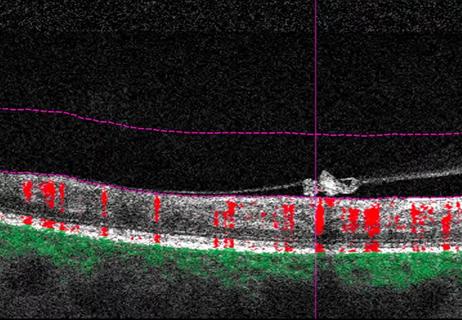
Why retina specialists should get comfortable with this imaging tool
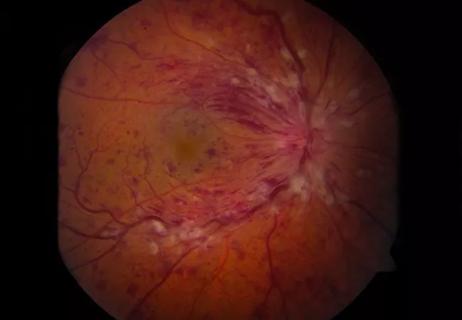
Intraretinal fluid volumes and other features detectable with OCT may help predict treatment response