Intracardiac echo mapping of para-septal fat pads provides fast, accurate and radiation-free targeting
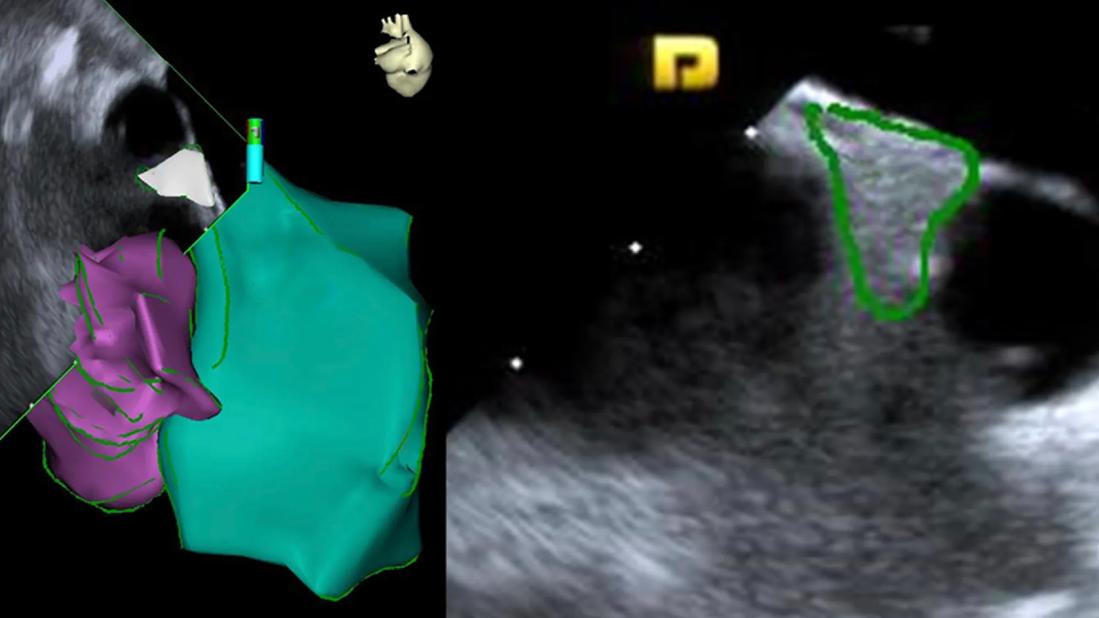
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7959a6f4-cb34-4f3f-916b-049006c20fcf/cardioneuroblation-cqd-feature)
side-by-side heart scans with color markings
A novel approach to cardioneuroablation using intracardiac echocardiography (ICE) to guide targeting is feasible for treatment of cardioinhibitory vasovagal syncope and results in good outcomes at midterm follow-up. That’s the conclusion of a team of electrophysiologists at Cleveland Clinic who used ICE to localize ganglionated plexi within visible epicardial fat pads in Waterston’s interatrial groove for radiofrequency ablation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The series of 17 patients who underwent the procedure was reported in a study in Europace (2025;27[12]:euaf295).
“Our ICE-based localization strategy is highly accurate and has important advantages over other methods that use CT mapping,” says the study’s lead and corresponding author, Pasquale Santangeli, MD, PhD, Director of the Ventricular Tachycardia Program at Cleveland Clinic. “By relying on live non-fluoroscopic guidance, this approach avoids patient exposure to radiation doses and also provides an unequivocal and reproducible way to visualize the ablation targets.”
Radiofrequency ablation of epicardial ganglionated plexi — specifically, clusters of parasympathetic inputs to the sinus node and atrioventricular node (AVN) — has been reported to be effective for treating cardioinhibitory vasovagal syncope. However, identification of the optimal target sites and techniques for accessing them has been a subject of continuous investigation.
Anatomical evidence from cardiac surgery cases indicates that fat pads located in Waterston’s groove have the highest density of such ganglionated plexi, making these areas excellent ablation targets. The operators in this series employed direct imaging of these targets using ICE to guide cardioneuroablation.
The cohort consisted of 17 patients (ages 18-56 years; 53% men) with recurrent cardioinhibitory vasovagal syncope refractory to first-line therapy. Patients had been referred for pacemaker implantation and were offered cardioneuroablation as an alternative.
Advertisement
All patients had a history of at least two episodes of syncope within the previous year, with 24% having had at least five episodes. All had ECG documentation of bradyarrhythmia correlating with syncope, including sinus pauses (n = 13) and/or AVN block (n = 4).
The procedures were conducted between October 2022 and July 2024.
Cardioneuroablation targets were identified with ICE and reconstructed on a 3D electroanatomic map.
Ablation covered right atrial and left atrial sites adjacent to fat pads and focused on the following, based on patient needs:
Identification of the target fat pads was accomplished in all patients; the mean time for complete mapping was 7 ± 5 minutes.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/eaf1c894-72ec-4d69-9226-a68f8eaa7913/cardioneuroblation-cqd-inset)
Representative ICE visualization and reconstruction of the right superior fat pad. Note the topographic anatomical relationships visualized on ICE: the target right superior fat pad is contained in between the superior vena cava (SVC), the septal aspect of the right superior pulmonary vein (RSPV) and the lower border of the right pulmonary artery (PA). Reprinted from Farwati et al., (Europace. 2025;27[12]:euaf295), under terms of the Creative Commons Attribution License. © The authors.
“We demonstrated the importance of these targets by observing an immediate and significant increase in heart rate after radiofrequency ablation,” Dr. Santangeli explains. “After completion of the procedure, there was total abolition of sinus pauses and AVN block with extracardiac high-frequency vagal stimulation, confirming these targets’ value.”
Procedures were conducted under general anesthesia. Total procedure time was 157 ± 43 minutes, including total radiofrequency time of 27 ± 10 minutes. No periprocedural complications occurred. Patients were kept overnight on continuous ECG monitoring.
Advertisement
After median follow-up of 12 months (interquartile range, 4-25 months), results were as follows:
“I believe that using ICE guidance optimizes the ablation and also, we anticipate, the durability of the positive treatment effects,” says study co-author Oussama Wazni, MD, MBA, Section Head of Cardiac Electrophysiology and Pacing at Cleveland Clinic. “We will continue to monitor these patients and others undergoing the procedure to gather long-term data on a larger cohort for a future published series.”
Because of the excellent results in these early patients, Dr. Wazni reports that Cleveland Clinic electrophysiologists now routinely use this strategy for qualified candidates. He adds that many electrophysiologists at other centers that offer cardioneuroablation for vasovagal syncope also target the same ganglionated plexi used in this study, but identification is less specific and relies on preprocedural CT acquisitions.
“We believe that changing to ICE can improve outcomes even more,” he says. “Experienced electrophysiologists should be able to adopt this approach based on details provided in our published article.”
Advertisement
Advertisement
Large series confirms early and long-term survival advantages over partial pericardial resection
Join us in Cleveland July 17 for a practical, first-of-kind course
AHA statement provides the latest comprehensive, evidence-based information
Why definitive surgical closure is the gold standard, and new ways to make it possible
Multimodal evaluations reveal more anatomic details to inform treatment
A closer look at the impact on procedures and patient outcomes
Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve
Join us in Florida this winter for a long-standing CME favorite