Sustained efficacy and safety
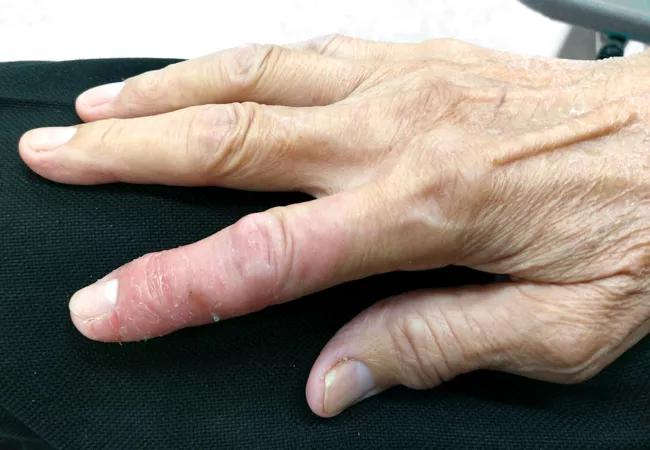
Intravenous golimumab is both safe and effective over a one-year treatment period for patients with psoriatic arthritis (PsA), according to the results of a randomized controlled trial known as GO-VIBRANT and recently published in Arthritis Care and Research. Results demonstrate a sustained response from the previously reported 24-week study.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Given the changing landscape of psoriatic disease treatment, a more tailored approach that takes into account disease characteristics, prior treatments and patient preferences, is now possible,” says M. Elaine Husni, MD, MPH, first author of the publication and Director of the Arthritis and Musculoskeletal Treatment Center and Endowed Chair of Translational Functional Medicine Research at Cleveland Clinic. “Our results show that IV golimumab is another safe and effective treatment option for patients with PsA.”
GO-VIBRANT was a phase 3, randomized, double-blinded, placebo-controlled study evaluating the efficacy of golimumab, a fully human monoclonal antibody against tumor necrosis factor alpha (TNF-ɑ). The study investigated the drug’s effect on patients who had active disease despite conventional therapy with disease-modifying anti-rheumatic drugs (DMARDs) or non-steroidal anti-inflammatories (NSAIDs).
The golimumab group (N = 241) received 2 mg/kg at weeks 0 and 4 and then every 8 weeks, while the placebo group (N = 239) began crossover to golimumab at weeks 24 and 28 and then every 8 weeks if there was limited response. The primary outcome of the study was the proportion of patients achieving American College of Rheumatology 20% (ACR20), 50% (ACR50) or 70% (ACR70) improvement criteria, as well as the Psoriasis Area and Severity Index > 75% improvement criteria (PASI75) when receiving golimumab compared with placebo. Researchers used the PsA-modified Sharp/van der Heijde score (SHS) to measure radiographic progression.
Advertisement
At one year, 76.8% of patients in the golimumab group achieved an ACR20 response, compared with 77.0% in the placebo group. An ACR50 response was achieved in 58.1% of the golimumab group and 53.6% of the placebo group; 38.6% and 33.9%, respectively, met criteria for an ACR70 response. At one year, 71.9% of patients with 3% or more body surface area affected in the golimumab group achieved a PASI75 response compared with 60.6% in the placebo group. A little over 5% of patients treated with golimumab had one or more serious adverse events. Significant improvements in SHS and patient-reported health-related quality of life were seen in the golimumab group versus the placebo group.
Intravenous golimumab may offer an option for monotherapy to patients with PsA. “We saw some nice clinical efficacy here, especially in the intravenous form, but we also saw similar response rates in patients who were on combination methotrexate to those who were on golimumab monotherapy,” she says. “While the combination is better in rheumatoid arthritis, in psoriatic arthritis we need to think about the role of methotrexate and whether monotherapy might be a better option.”
The GO-REVEAL trial demonstrated the efficacy of subcutaneous golimumab, but GO-VIBRANT results showed slightly better efficacy in the intravenous form, offering a strong option for patients who prefer to avoid injectables.
“Patient preferences should help drive treatment algorithms, and the GO-VIBRANT study gives rheumatologists an intravenous biologic option for treating psoriatic arthritis,” says Dr. Husni. “We now can offer an even more personalized approach for patients with this disease.”
Advertisement
Advertisement

The case for continued vigilance, counseling and antivirals

High fevers, diffuse rashes pointed to an unexpected diagnosis

No-cost learning and CME credit are part of this webcast series

Summit broadens understanding of new therapies and disease management

Program empowers users with PsA to take charge of their mental well being

Nitric oxide plays a key role in vascular physiology

CAR T-cell therapy may offer reason for optimism that those with SLE can experience improvement in quality of life.

Unraveling the TNFA receptor 2/dendritic cell axis