Two studies reveal new insights about upper airway stimulation therapy
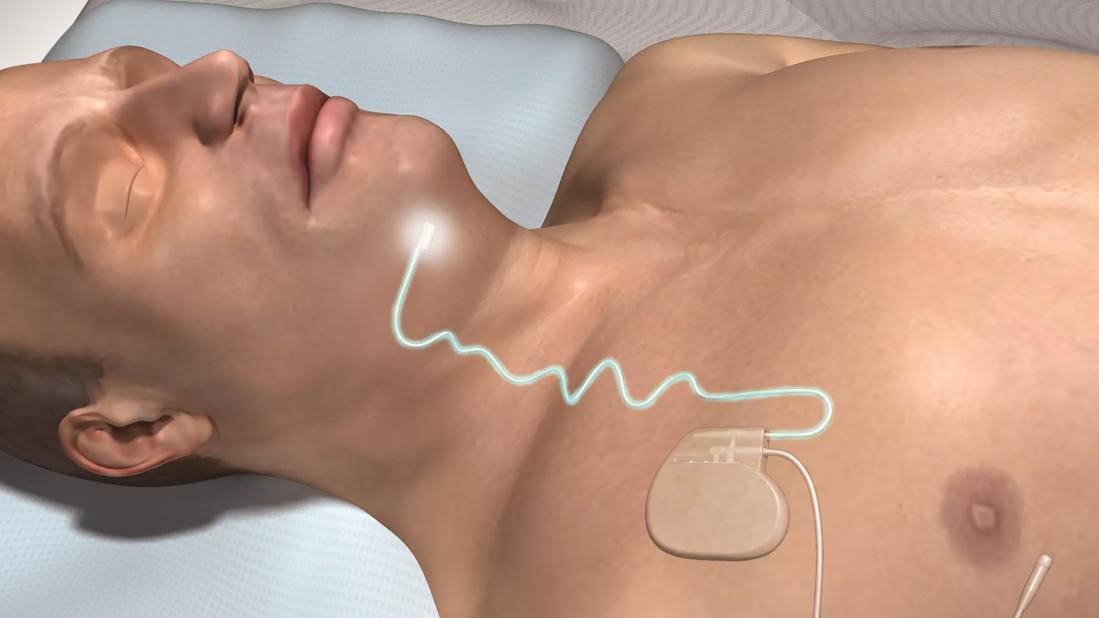
The Inspire® Upper Airway Stimulation (UAS) system has become a common therapeutic option for patients with obstructive sleep apnea (OSA) but intolerant of continuous positive airway pressure. Still, questions remain about how to improve post-operative outcomes and determine comparative utility with more traditional airway reconstruction approaches.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A new study led by otolaryngologist, Alan Kominsky, MD, staff in Cleveland Clinic’s Head & Neck Institute and Sleep Disorders Center, demonstrated in-office adjustments that improve post-operative outcomes related to UAS. Dr. Kominsky and Joseph Meleca, MD, first author on the study and fourth-year resident in the Head & Neck Institute, presented these findings at the American Academy of Otolaryngology-Head and Neck Surgery Annual Meeting in New Orleans on September 15.
The retrospective review examined 60 patients who underwent UAS, and later received awake endoscopy (AE) to correct discomfort or inefficacy related to their implanted UAS device. A total of 24 AEs were performed in 19 (32%) patients with an average of 235 (85-553) days from surgery. The study found that reprogramming the implanted pulse generator settings offered improved therapeutic benefit.
“There are few guidelines on post-operative AE adjustments for patients who have received an implant,” says Dr. Kominsky. “Our hope was that these recommendations, along with Inspire’s recent recommendations, will standardize clinical management and improve device compliance and results.”
This follows another recent study, also led by Dr. Kominsky, published by the American Journal of Otolaryngology. The study examined outcomes in patients with moderate-to-severe OSA who underwent hypoglossal nerve stimulation (HNS), the flagship UAS therapy, versus those who underwent traditional airway reconstructive surgery, specifically uvulopalatopharyngoplasty (UPPP).
Advertisement
The study, a retrospective case series, examined a group of patients who received HNS implantation (n=20) and a UPPP group (n=20). Data collection included age, sex, BMI, history of OSA treatment, pre- and post-operative Apnea–Hypopnea Index and self-reported Epworth Sleepiness Scale. Findings showed a greater relative difference in post-operative outcomes in the HNS cohort (-34.4, p=<0.001) compared to the UPPP cohort (-11.5, p=0.02).
“Soft-tissue airway surgery has been a standard-of-care for decades, but increasingly we find that HNS leads to better patient outcomes, which this study demonstrated,” says Dr. Kominsky.
UAS is a relatively new intervention and further studies are needed to improve outcomes and demonstrate its comparative success. Surgeons, like Dr. Kominsky, believe it illustrates a new era in OSA intervention. “It’s changing the landscape of sleep surgery, and that warrants continued investigation.”
Advertisement
Advertisement

Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor

Case study illustrates the potential of a dual-subspecialist approach

Evidence-based recommendations for balancing cancer control with quality of life

Study shows no negative impact for individuals with better contralateral ear performance

HNS device offers new solution for those struggling with CPAP

Patient with cerebral palsy undergoes life-saving tumor resection

Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition

Detailed surgical process uncovers extensive middle ear damage causing severe pain and pressure.