Pilot study supports feasibility when paired with a cloud-based platform
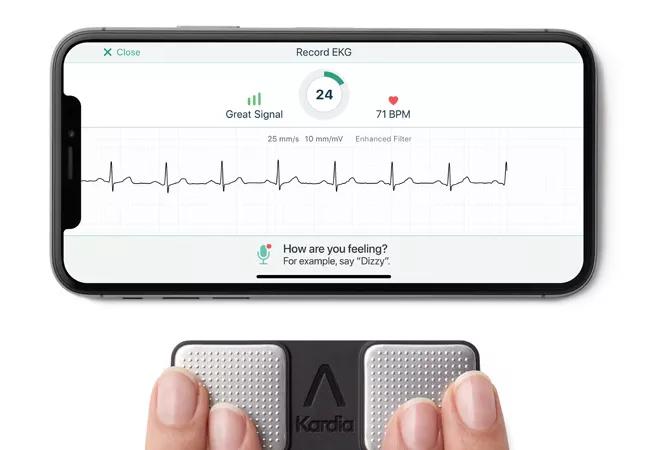
Coupling a smartphone-based ECG device with a novel cloud-based platform provides effective detection of long-term post-ablation atrial fibrillation (AF), finds a pilot study published in Cardiovascular Digital Health Journal (2021;2:92-100).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The system enabled us to provide better care with no increase in phone calls, emergency department visits, hospitalizations or patient anxiety — and with less need for additional traditional monitoring,” says the study’s principal investigator, Khaldoun Tarakji, MD, MPH, Associate Section Head of Cardiac Electrophysiology at Cleveland Clinic.
Previous studies of consumer ECG devices have focused on validating the technology or screening the general public. This was the first study to assess a platform designed to alert physicians only to abnormal ECGs for verification and follow-up.
“We were able to show that a consumer digital device can be integrated into patient care successfully, with no additional burden on patients or physicians,” says Dr. Tarakji.
Digital health devices for consumers promise to deliver better, more effective care at a lower cost. However, adoption by clinicians has been slow.
A primary reason, says Dr. Tarakji, is lack of a clear workflow to triage and handle the data, which has spawned concerns about data overload for busy clinicians.
“How does a practitioner manage, triage and store these data?” Dr. Tarakji asks. “Until these issues are addressed, the technology can be used on a handful of patients, but scalability is limited.”
An enthusiastic proponent of digital technology, Dr. Tarakji has investigated multiple smartphone-based health applications. One of them is the KardiaMobile device (AliveCor®), which he has used for arrhythmia detection for his patients for several years.
Advertisement
He worked with the device’s manufacturer to develop its KardiaPro software platform, which bypasses the need for emails and allows ECG strips to be securely uploaded to the cloud rather than shared as email attachments.
Artificial intelligence was used to interpret the recordings and provide initial diagnosis of normal rhythm or possible AF. The platform was then programmed to flag abnormal recordings and suspected AF and then send these recordings to an inbox, where they can be retrieved and read by the physician in a timely fashion. Normal ECGs remain on the platform; they are not directed to the physician’s attention but can be easily accessed on demand.
The pilot study — a single-center investigation at Cleveland Clinic — was designed to evaluate how the KardiaMobile/KardiaPro (KM/KP) platform compares with routine care following successful AF ablation and to assess its suitability for long-term follow-up. “We hoped to ease fears in the medical community about adopting these technologies,” Dr. Tarakji says.
The study also aimed to determine:
A total of 100 patients (mean age, 64) presenting four months after initial successful AF ablation were randomized — 51 to the KM/KP arm and 48 to traditional care (1 withdrew) — and followed for six months. Patients in both arms were able to contact their electrophysiologist about any questions or symptoms. Additionally, patients in the KM/KP group were told to record their heart rhythm once a week, or whenever they had symptoms.
Advertisement
AF was detected in 11 patients in the KM/KP group (21.6%) at a median of 68 days compared with 7 patients in the control group (14.6%) at a median of 91 days. These differences were not statistically significant but showed a trend favoring the KM/KP smartphone approach.
Upon physician review, the four recordings in the KM/KP group labeled as possible AF were found to be sinus rhythm with premature atrial contractions. None of the 40 patients in the KM/KP group who had no recording interpreted as possible AF were found to have AF upon review.
Healthcare utilization was similar between the groups, although more patients in the control group (27.1%) than in the KM/KP group (5.9%) required additional ECGs or cardiac monitors (P = 0.004).
“This indicates that these smart device ECG tracings, when coupled with physician review of suspected AF episodes, are reliable and reduce the need for additional traditional monitoring,” Dr. Tarakji notes.
Concerns that providers would be deluged with data proved to be unfounded, as patients in the KM/KP arm collected and transmitted two recordings per week, on average.
Fears that older patients would not use the technology also proved unjustified. Enthusiasm for the technology spanned age brackets and education levels. None of the patients enrolled had prior experience using smartphone ECG technology, Dr. Tarakji says.
Speculation that access to information on their heart rhythm would increase patients’ anxiety also was unfounded. Responses to a generalized anxiety disorder questionnaire given before and after the study saw no change in anxiety scores in either group.
Advertisement
“The ability to visualize the recordings with instant automated interpretation provided reassurance, which is an advantage not available with traditional cardiac rhythm monitors,” Dr. Tarakji observes.
The authors hope this study will encourage more electrophysiologists to embrace digital technology for post-ablation monitoring. “These devices empower patients by providing the tools to record their rhythm when they need to,” Dr. Tarakji says.
He adds that the ability to access multiple ECG recordings over time promises to foster better-informed care that can be achieved remotely. “A virtual visit supported by ECG data obtained over time is better than an in-person visit with one single ECG,” he explains. “These are the types of solutions that prompt us to challenge ourselves. The future is here. We just need to understand it better.”
“Our clinical care and follow-up of patients with atrial fibrillation continues to improve,” adds study co-author Oussama Wazni, MD, Section Head of Cardiac Electrophysiology. “Leveraging these tools will help patients and physicians collaborate and be true partners in atrial fibrillation management. It’s an exciting time.”
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more