
Cardiac transplantation is a treatment option for heart failure that is subject to strict eligibility criteria resulting in limited access for older patients with common medical co-morbidities such as obesity and diabetes. Just over 3,800 cardiac transplants were performed in the United States in 2021, leaving thousands on the national waitlist and tens of thousands ineligible for a coveted spot.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“While extraordinary advances in left ventricular assist device care during the last 25 years make it possible to provide a life-saving treatment to many heart failure patients who are not eligible for cardiac transplantation, too few are being offered this destination therapy,” says Mauricio Velez, MD, a specialist in advanced heart failure and transplant cardiology with Cleveland Clinic Florida.
Clinical outcomes for LVAD therapy have improved dramatically over time. Based on the most recent report of the Interagency Registry of Mechanically Assisted Circulatory Support (INTERMACS), mean one-year post-LVAD survival is 83%. Recent reports of long-term LVAD support have suggested that survival greater than 50% at seven years with a low incidence of disabling complications is possible.
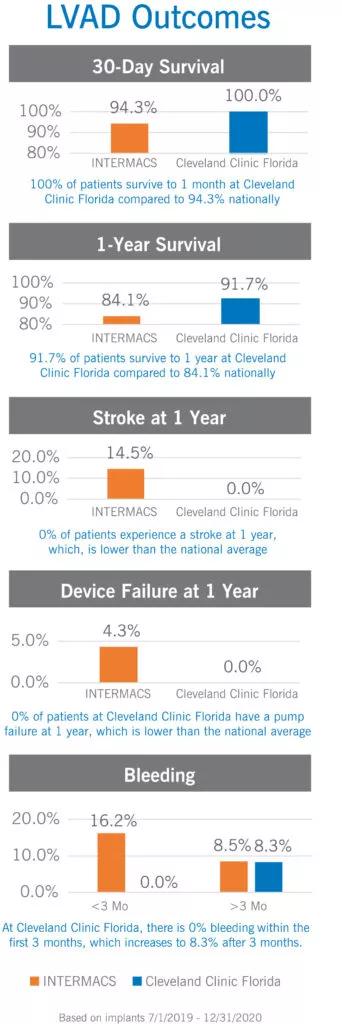
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/16f466af-5a88-4555-84bb-0f50a27682e6/Weston-LVAD-outcomes-12-2020_FOR-PUB-342x1024_jpg)
Clinical outcomes for patient supported with long-term left ventricular assist devices at Cleveland Clinic Florida, 2019-2020 implants.
The data for this research were provided by The Society of Thoracic Surgeons’ Interagency Registry for Mechanically Assisted Circulatory Support (Intermacs) Database – INTERMACS Data Quality Report (2021-07)
“Personally, I’ve cared for a patient who was supported by the same LVAD for more than 10 years,” notes Dr. Velez.
At Cleveland Clinic Florida, outcomes currently exceed national statistics with one-year survival after LVAD surgery of more than 91%, rivaling one-year survival after cardiac transplantation estimated at 92%. The survival benefit with LVAD support is accompanied by improvements in quality of life and functional status that are noticeable as early as three to six months after implantation.
Advertisement
A significant majority of patients experience symptom improvement from New York Heart Association (NYHA) class IIIb-IV (severe symptoms) to NYHA class I-II (mild to no symptoms) after LVAD surgery. Rehospitalization after LVAD remains a significant challenge, with a majority of patients requiring a hospital admission within one year of surgery.
“Nationally, short and long-term survival are likely to inch closer to that of cardiac transplantation as clinical care and LVAD technology continue to improve,” adds Dr. Velez.
Florida is home to 20 million people, based on recent U.S. Census figures. It is estimated that 2.6% of the U.S. population suffers from heart failure, translating to approximately 520,000 people in Florida. Of these, about 50% suffer from heart failure with reduced ejection fraction and about 20% of those individuals – an estimated 52,000 people – are living with severe heart failure symptoms.
About half of these patients, or some 26,000 people in Florida, are younger than 80 years, and many of them could benefit from advanced heart failure therapies, including cardiac transplant and mechanical circulatory support. Yet only 263 heart transplants were performed in Florida in 2021, based on data from the Scientific Registry of Transplant Recipients and the United Network for Organ Sharing, and only 63 (24%) were performed in patients older than 65 years.
“These contrasting figures highlight the fact that cardiac transplantation alone cannot meet the care needs of the large population of advanced heart failure patients in our region,” says Dr. Velez. “However, LVAD surgery volume in Florida as a whole has been chronically low, revealing a great need for access to this treatment option for patients with severe heart failure symptoms.” Cleveland Clinic Florida’s Advanced Heart Failure section includes a heart transplant program and a mechanical circulatory support program, distinguished with exceptional outcomes. Long-term LVAD therapy is based on a multidisciplinary team approach and in collaboration with referring physicians. Early referral improves individual patient outcomes and is strongly encouraged.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/95441d4f-430a-40d1-99a4-1cccf0b78da0/LAVD-chart-540x1024_png)
Advertisement
Advertisement

Nonthermal technique reduces bleeding and perforation risk

Standardizing a minimally invasive approach for Barrett’s Esophagus and Esophageal Cancer

PSMA-targeted therapy for metastatic prostate cancer now offered at Cleveland Clinic Weston Hospital

Nationally recognized urologic oncologist offers vision for growth, innovation, and excellence

Noninvasive modality gains ground in United States for patients with early-to-moderate disease

Cleveland Clinic Weston Hospital’s collaborative model elevates care for complex lung diseases

Interventional pulmonologists at Cleveland Clinic Indian River Hospital use robotic technology to reach small peripheral lung nodules

Trained in the use of multiple focal therapies for prostate cancer, Dr. Jamil Syed recommends HIFU for certain patients with intermediate-risk prostate cancer, especially individuals with small, well-defined tumors localized to the lateral and posterior regions of the gland.