Study followed patients an average of eight years
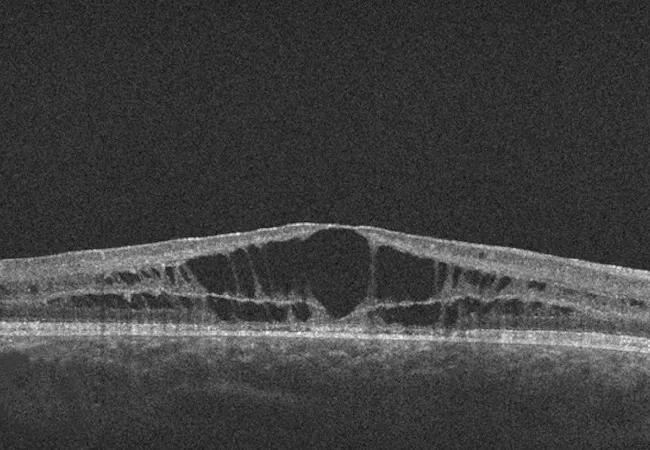
Patients with retinoschisis (splitting of retinal layers) typically present in childhood with cystic macular lesions and decreased visual acuity. Most people with the disease record low visual acuity (20/70 to 20/200) by early adulthood (median age 25).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Though it’s one of the more common inherited retinal diseases, juvenile X-linked retinoschisis (XLRS) currently has limited treatment options. However, there has been a surge of interest in finding treatments for XLRS due to the identification of the nearly 300 genes that cause the majority of inherited retinal diseases, as well as the discovery of gene therapy for patients with pathogenic sequence variations in the RPE65 gene, says Elias Traboulsi, MD, MEd, Director of the Center for Genetic Eye Diseases at Cleveland Clinic Cole Eye Institute.
“There are ongoing gene therapy trials for the RS1 gene, which causes XLRS,” he says. “We do not yet have official results. While we’re making good progress, we’re not there yet.”
Given the indeterminate advent of XLRS-targeted gene therapy, Dr. Traboulsi and his research team recently studied the long-term effects of topical dorzolamide, a carbonic anhydrase inhibitor often used to treat XLRS.
“Dorzolamide was initially developed as an intraocular pressure-lowering drug, and its favorable effects on cystoid macular edema have been well described,” he says.
The retrospective interventional study, recently published in Retina, involved 18 eyes in 10 male patients with genetically confirmed XLRS and the presence of cystic macular lesions on optical coherence tomography (OCT). (Two eyes were excluded from the study due to retinal detachment.)
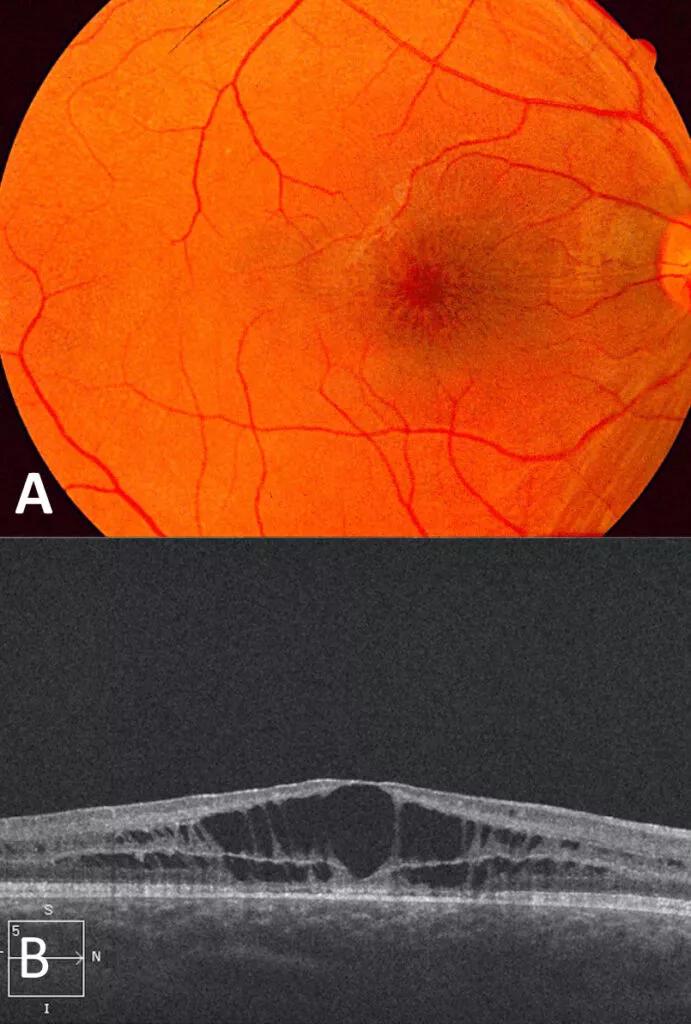
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2902ed65-dba8-4f3b-83d7-f311046ff28d/22-EYE-3391159-CQD-Treating-Retinoschisis-inset-691x1024_jpg)
A. Right fundus photograph of a patient with X-linked juvenile retinoschisis. Note the spokelike pattern of cystic schisis cavities in the foveal region. B. OCT demonstrating schisis cavities in the macula of a patient with X-linked juvenile retinoschisis.
Advertisement
The patients, examined and followed at the Cole Eye Institute between 2005 and 2021, were treated with topical 2% dorzolamide eyedrops two to three times per day in both eyes. Dr. Traboulsi has been prescribing the drops three times per day (if possible) since 2015 because he has observed it to work in some patients when twice daily application has not. (There are no comparative studies, however.) None of the patients experienced any significant side effects of topical dorzolamide.
The study showed a statistically significant improvement in visual acuity over a follow-up period averaging eight years — the longest follow-up to date in an XLRS case series. As measured by logarithm of minimum angle of resolution (based on best-corrected visual acuity using a Snellen chart), mean visual acuity was 0.45 (20/56) at baseline (standard deviation [SD] 0.17) and 0.34 (20/43) at last follow-up visit (SD 0.22, P < .01).
The study also found that while patients’ central subfield thickness (CST) decreased by an average of 57.60 microns (429.88 at baseline, 372.28 at last follow-up visit) in the same average follow-up period, that decrease was not statistically significant (P = .10).
Notably, one patient had no cystic macular lesions remaining around 10 years after starting dorzolamide treatment.
“It looks like this treatment is not only preventing the schisis in the macular area from increasing, but it may be helping stabilize, if not improve, visual acuity over time,” says Dr. Traboulsi.
These results confirm findings from earlier studies, all of which had fewer patients and/or a shorter follow-up period.
Advertisement
“There’s still a lot of variability between patients and even at different times when we examine these patients; the retina may get thicker or thinner again,” says Dr. Traboulsi.
He explains that CST is not a reflection of the actual retinal layers. Though the retina itself may be thinner, the cystoid spaces may be bigger, causing a larger measurement.
While he wasn’t surprised by the overall results, Dr. Traboulsi says it was a “pleasant surprise” to find that visual acuity was indeed improved over such a long period of time.
“In a diseased retina, you would expect that over time some of the photoreceptors or other retinal neurons would get damaged and vision would get worse, even if the schisis cavities were reduced,” he says. “Longer follow-up will shed more light on the ultimate outcome of vision and retinal degeneration in this disease while patients are on dorzolamide.”
Because patients with X-linked retinoschisis are not encountered often in general ophthalmic practices, or even in retina specialty practices, Dr. Traboulsi believes studies like this one have a powerful impact on clinical care.
“Care is not only to give or not give a medication, but it’s also how confident we are in delivering a certain modality of treatment and what we can tell patients to expect from it,” he says. “I think this paper will change clinical care because it will make clinicians more confident that dorzolamide is indeed the way to treat these patients while we await more definitive types of treatments.”
Advertisement
Advertisement

Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma

Registry data highlight visual gains in patients with legal blindness

Prescribing eye drops is complicated by unknown risk of fetotoxicity and lack of clinical evidence

A look at emerging technology shaping retina surgery

A primer on MIGS methods and devices

7 keys to success for comprehensive ophthalmologists

Study is first to show reduction in autoimmune disease with the common diabetes and obesity drugs

Treatment options range from tetracycline injections to fat repositioning and cheek lift