Is it ready for prime time?
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/547157b8-c76c-49db-8839-3b952252acc1/650x450-SHOSKES-Shockwave_jpg)
650×450-SHOSKES-Shockwave
By Daniel Shoskes, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As urologists, we have decades of experience with extracorporeal shockwave lithotripsy for breaking apart stones within the body. Today, a related and emerging technology, low-intensity shockwave therapy (LiSWT), is being explored for several other urological applications.
Already used in orthopedics, physical therapy and wound treatment, the small, portable LiSWT device uses energy levels about 10 percent of that used for lithotripsy, producing painless procedures without the need for general or local anesthetic. The device is not yet commercially available in the United States.
LiSWT’s biologic effects include neo-angiogenesis, improved blood flow, tissue remodeling, influx of stem cells and reduction of pain and inflammation.1, 2 Presumed mechanisms of action include neovascularity with improved arterial flow3 and influx of stem cells (assessed in animal models).4
In urology, the most common and thoroughly studied application of LiSWT is for erectile dysfunction (ED). The original protocol involved treating the penis twice a week for three weeks, repeated after a no-treatment interval of three weeks.5 Improvements were seen in International Index of Erectile Function (IIEF-5) Questionnaire scores and in penile arterial blood flow. Effects were confirmed in a double-blind sham-controlled trial4 using modified once-per-week protocols, which are much more practical for patients.6
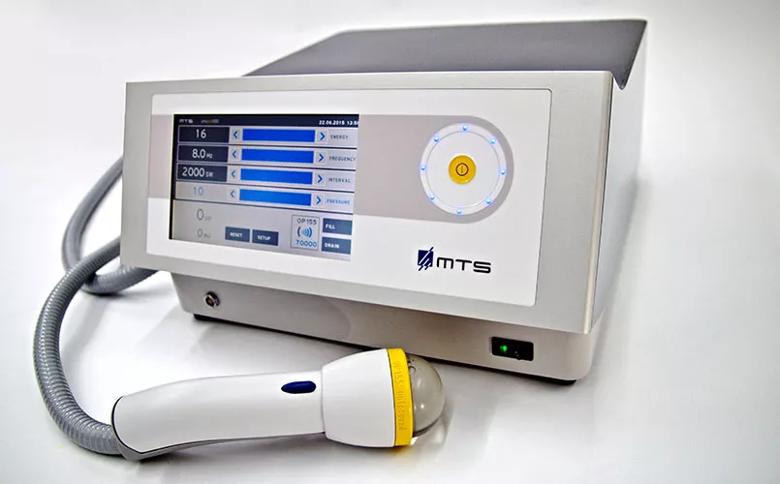
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/16f84da2-89ed-48a6-8072-d86b8876b326/805x-Inset-Shoskes-Shockwave_jpg)
UroGold 100™ device. Image courtesy of Tissue Regeneration Technologies, LLC (TRT); Woodstock, Georgia.
Advertisement
In our initial experience administering 3,000 shocks per week for six weeks using the UroGold 100™ device (Tissue Regeneration Technologies, LLC ; Woodstock, Georgia), Sexual Health Inventory for Men (SHIM) scores improved from 11.0 +/- 3.6 to 17.2 +/- 5.2 (p=0.01). SHIM was unchanged in 25 percent of patients, mildly improved in 12.5 percent but not sufficiently for intercourse, and significantly improved with erection sufficient for intercourse in 62.5 percent of patients.
Unlike other on-demand ED therapies, improvement with LiSWT appears durable to at least one year.
In Europe, LiSWT is also commonly used for chronic prostatitis/chronic pelvic pain syndrome (CPPS) or nonbacterial prostatitis. Typically, the protocol involves once weekly treatments for four weeks. Efficacy was reported at 12 weeks in the first sham-controlled study.7 However, long-term success is variable with one study showing loss of effect at 24 weeks8 and another showing persistence of benefit to one year.9
Understanding patient selection and mechanism of action of LiSWT for CPPS is more problematic. CPPS is a highly heterogeneous syndrome and none of the LiSWT studies to date attempted to clinically phenotype patients. While discussions have included improving prostate blood flow or reducing prostate inflammation, neither is likely an important pain driver for most CPPS patients. We hypothesize that the primary benefit of LiSWT in CPPS is treating pelvic floor spasm and trigger points, both very common in CPPS.10
Advertisement
We conducted a pilot study in our clinic of 10 men with CPPS, all of whom had pelvic floor spasm with or without trigger points. Four once-per-week sessions involved treating the perineum with 2,000 shocks per session. Total Chronic Prostatitis Symptom Index improved from 27.7 +/- 6.2 to 18.5 +/- 8.2 (p=0.0015). Seven patients had a greater than six-point drop, the accepted threshold for significant symptom improvement. By Global Response Assessment, six patients reported significant improvement, one was somewhat improved and three were unchanged. There were no side effects.
LiSWT is a new technology that has reasonable preliminary data and plausible mechanisms of action in erectile dysfunction and chronic pelvic pain syndrome. Ideal patient selection and treatment course is yet to be determined.
Advertisement
Advertisement
Innovative single-port technique results in no visible scarring
The new application that could augment cancer detection, improve efficiency
Pediatric urologists lead quality improvement initiative, author systemwide guideline
Fixed-dose single-pill combinations and future therapies
Reproductive urologists publish a contemporary review to guide practice
Two recent cases show favorable pain and cosmesis outcomes
Meta-analysis assesses outcomes in adolescent age vs. mid-adulthood
Proteinuria reduction remains the most important treatment target.