AVANT GUARD trial extends first-line role for ablation beyond paroxysmal atrial fibrillation
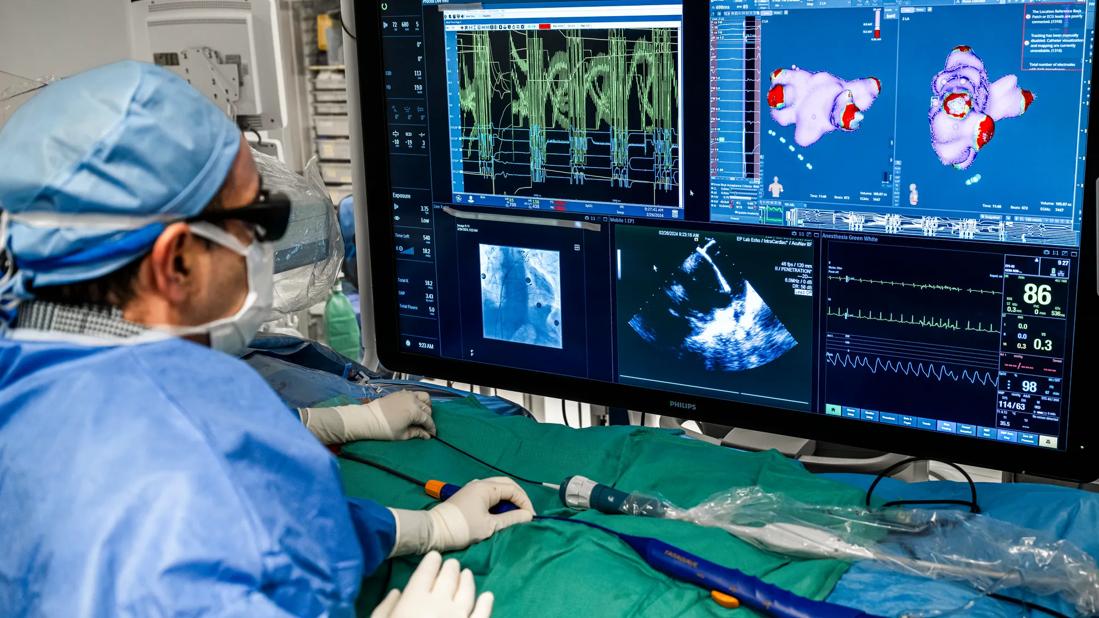
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/9be7fda4-321c-4848-8679-b904327262b8/CCC_4654080_02-26-24_121_MLC-jpg)
doctor looking at images on monitor during a heart procedure
First-line treatment of persistent atrial fibrillation (AF) with pulsed field ablation (PFA) significantly reduces atrial arrhythmia recurrence and burden relative to antiarrhythmic drug therapy, with a similar rate of serious adverse events, according to results of the international AVANT GUARD trial.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The findings, reported in a late-breaking clinical trial presentation at the Heart Rhythm Society’s Heart Rhythm 2026 conference and simultaneously published in the New England Journal of Medicine, promise to reshape initial management of persistent AF.
“We found that ablation is much better than medical therapy as first-line treatment for persistent atrial fibrillation, with 56% of patients achieving acute and chronic treatment success through 12 months after ablation, compared with 30% after starting antiarrhythmic drug therapy,” says global principal investigator Oussama Wazni, MD, MBA, who designed the trial and presented its results.
The findings build on another trial led by Dr. Wazni, STOP AF First (N Engl J Med. 2021;384:316-324), which established cryoballoon ablation as superior to drug treatment as initial therapy to prevent recurrence in patients with paroxysmal AF. “AVANT GUARD involves patients with persistent AF, whereas STOP AF First focused on paroxysmal AF,” notes Dr. Wazni, Head of Cardiac Electrophysiology and Pacing at Cleveland Clinic. “So we are applying first-line ablation further along in the disease process, as persistent AF is more difficult to treat and generally involves sicker patients.”
He adds that AVANT GUARD is also the first major study of PFA as first-line therapy for AF, noting that other trials used cryoballoon ablation.
Persistent AF — defined as continuous AF lasting more than seven days — affects up to 50% of people with AF. Compared with paroxysmal AF, it is associated with worse outcomes, including higher risks of death, thromboembolism and heart failure as well as increased healthcare utilization.
Advertisement
Current guidelines recommend trying antiarrhythmic drugs before catheter ablation for persistent AF, but data on PFA as a first-line treatment are lacking. PFA is a newer ablation technology that may offer advantages over thermal ablation methods, particularly in patients with persistent AF, who often have significant atrial remodeling.
AVANT GUARD was designed as a multicenter, prospective, randomized controlled trial. From December 2023 to February 2025, 310 treatment-naive patients with symptomatic persistent AF were randomized on a 2:1 basis to PFA (n = 207) or antiarrhythmic drug therapy (n = 103). An additional 78 patients were assigned to PFA and monitored solely for safety endpoints.
Patients assigned to PFA underwent pulmonary vein isolation and posterior wall ablation using the pentaspline FARAWAVE catheter. Patients assigned to drug therapy were prescribed daily antiarrhythmic medications consistent with guideline-directed therapy for persistent AF, with amiodarone explicitly excluded. Drugs were titrated as needed during the study’s first 90 days (i.e., blanking period).
All patients received insertable cardiac monitors for continuous rhythm monitoring throughout the study period.
The primary effectiveness end point combined acute and chronic treatment success through 12-month follow-up. Acute success was defined as procedural success in the PFA group and as absence of ablation during the study’s blanking period in the drug group. Chronic success was defined as freedom from amiodarone through 12 months and freedom from all of the following after the blanking period:
Advertisement
“This is the first study to include one hour of asymptomatic atrial arrhythmia as an end point component in addition to the standard component of 30 seconds of symptomatic atrial arrhythmia,” Dr. Wazni notes. “That’s an important addition because the latter has not been associated with clinically meaningful outcomes or pathophysiological processes.”
The primary safety end point (assessed in the 78 PFA patients assigned to the safety analysis plus the randomized patients) was the rate of device- or procedure-related serious adverse events.
Baseline characteristics were well balanced between patient groups, with an average age of around 67 years and a mean CHA₂DS₂-VASc score of approximately 2.5.
Acute isolation of pulmonary veins was confirmed in all patients undergoing PFA. Mean procedure time was 85 ± 32 minutes, which included a prespecified 20-minute waiting period. The drug therapy group received a mean of 1.2 unique antiarrhythmic drugs during the blanking period, with flecainide and sotalol being the most common agents. Cardioversion was required in 64% of drug-treated patients during the blanking period.
At 12 months, the primary effectiveness end point was met by 56.0% of patients in the PFA group versus 30.1% in the drug therapy group (hazard ratio = 0.46; 95% CI, 0.33-0.65; P < .001). As detailed in the table below, recurrence of symptomatic atrial arrhythmias was low in both groups, but asymptomatic atrial arrhythmia lasting one hour or more was significantly lower in the PFA group. Median atrial arrhythmia burden was also lower with PFA. Quality-of-life improvements were observed in both groups, with a slightly higher mean change in Atrial Fibrillation Effect on Quality of Life (AFEQT) score in the PFA group.
Advertisement
| Endpoint | Antiarrhythmic Drugs (n = 103) | Pulsed Field Ablation (n = 207) |
|---|---|---|
| Primary treatment success (12 months) | 30.1% | 56.0% |
| Symptomatic atrial arrhythmia recurrence ≥30 seconds | 2.9% | 1.9% |
| Asymptomatic atrial arrhythmia recurrence ≥1 hour | 45.6% | 30.4% |
| Median post-blanking arrhythmia burden | 0.3% | 0.0% |
| Quality of life (mean AFEQT score change) | 19.8 | 23.3 |
| Endpoint | ||
| Primary treatment success (12 months) | ||
| Antiarrhythmic Drugs (n = 103) | ||
| 30.1% | ||
| Pulsed Field Ablation (n = 207) | ||
| 56.0% | ||
| Symptomatic atrial arrhythmia recurrence ≥30 seconds | ||
| Antiarrhythmic Drugs (n = 103) | ||
| 2.9% | ||
| Pulsed Field Ablation (n = 207) | ||
| 1.9% | ||
| Asymptomatic atrial arrhythmia recurrence ≥1 hour | ||
| Antiarrhythmic Drugs (n = 103) | ||
| 45.6% | ||
| Pulsed Field Ablation (n = 207) | ||
| 30.4% | ||
| Median post-blanking arrhythmia burden | ||
| Antiarrhythmic Drugs (n = 103) | ||
| 0.3% | ||
| Pulsed Field Ablation (n = 207) | ||
| 0.0% | ||
| Quality of life (mean AFEQT score change) | ||
| Antiarrhythmic Drugs (n = 103) | ||
| 19.8 | ||
| Pulsed Field Ablation (n = 207) | ||
| 23.3 |
The primary safety end point of device- or procedure-related serious adverse events occurred in 5.1% of PFA-treated patients, meeting the study’s prespecified safety goal. Serious adverse events overall occurred in 25.1% of the PFA group and 21.1% of the drug therapy group. No deaths were attributed to the PFA procedure or device.
Six neurological events related to stroke occurred among the first 183 patients assigned to PFA, with one event attributed to air embolism; all six patients showed clinical improvement or full recovery on follow-up. After a temporary study pause and protocol modifications to improve safety, no strokes or transient ischemic attacks were observed among the subsequent 74 patients assigned to PFA.
The protocol changes involved excluding patients with a CHA₂DS₂-VASc score ≥4, screening for left atrial thrombus within 24 hours of PFA using transesophageal echocardiography or CT scan, providing at least four weeks of uninterrupted anticoagulation before the procedure and ensuring a minimum activated clotting time prior to ablation.
“Using continuous rhythm monitoring, we have shown that ablation with the pentaspline PFA catheter resulted in a lower burden of detected atrial arrhythmia recurrence through one year compared with antiarrhythmic drug therapy in treatment-naïve patients with persistent AF,” Dr. Wazni observes. “These findings support PFA as an effective initial rhythm control strategy in persistent AF.”
“AVANT GUARD adds to the wealth of evidence showing that first-line catheter ablation is superior to medical therapy, expanding this approach to patients with persistent atrial fibrillation using PFA technology,” observes Walid Saliba, MD, Medical Co-Director of Cleveland Clinic’s Atrial Fibrillation Center, who was not directly involved in the study.
Advertisement
Dr. Wazni notes that the study’s design calls for continuous rhythm monitoring through three years of follow-up, which should provide more comprehensive insights on the comparative treatment strategies.
In their study report, the authors point out that AVANT GUARD’s population was older and had more comorbidities than participants in previous trials of persistent AF, which they say reflects real-world practice and may help explain the trial’s lower absolute success rates and higher event rates relative to prior studies.
They also note that the absence of neurological events after the study’s procedural protocol for PFA was modified is reassuring. “This underscores the importance of careful pre- and periprocedural management to minimize the risk of adverse events with early ablation in this setting,” Dr. Wazni concludes.
AVANT GUARD was funded by Boston Scientific Inc., the manufacturer of the PFA system used in the study. Dr. Wazni reports that he is a paid speaker and consultant for Boston Scientific.
Advertisement
LAA closure may be compelling option in atrial fibrillation ablation patients at high risk of both stroke and bleeding
UK experts compare and contrast the latest recommendations
While results were negative for metformin, lifestyle counseling showed surprising promise
Investigational pulsed-field ablation system also yielded procedural efficiencies
Concomitant AF ablation and LAA occlusion strongly endorsed during elective heart surgery
ACC/AHA panel also upgrades catheter ablation recommendations
For the first time, risk is shown after accounting for underlying contributions of pulmonary disease
Retrospective analysis finds “hypoxic and sleepy” subtype to confer greatest risk