Similarly impressive outcomes argue for offering the valve-sparing option more often
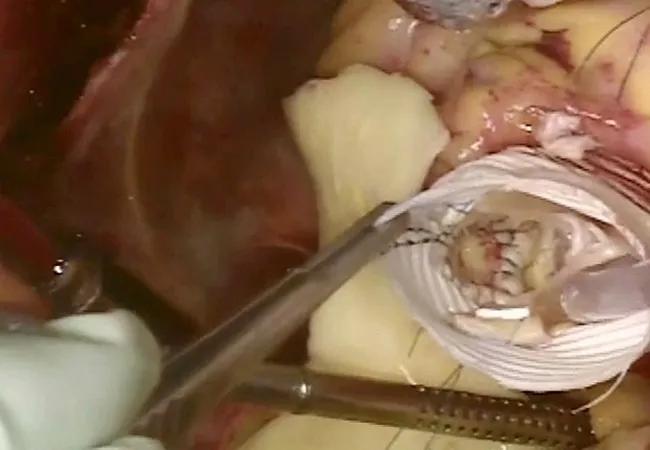
Both reimplantation and root replacement with a Bentall-type procedure for aortic root aneurysm are associated with excellent early and long-term outcomes in patients with or without aortic regurgitation, making reimplantation the better choice for most patients. So concludes a research team that analyzed a large cohort of patients who underwent either procedure at Cleveland Clinic over a recent 17-year period. The retrospective study was published in Aorta (2022;10[2]:57-68).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“In our experience, greater than 95% freedom from reoperation and severe regurgitation can be achieved at 10 years in patients with tricuspid aortic valves who undergo reimplantation,” says the study’s lead author, Lars G. Svensson, MD, PhD, Chair of Cleveland Clinic’s Heart, Vascular & Thoracic Institute. “For this reason, we usually perform reimplantation over the Bentall root procedure, thereby avoiding the problems inherent to bioprosthetic or mechanical valves.”
Aortic root aneurysm accompanied by aortic regurgitation is typically managed electively with either a Bentall procedure (using a bioprosthesis or mechanical prosthesis incorporated in a polyester graft) or reimplantation of the native aortic valve within the graft using a modified David procedure; the modifications used at Cleveland Clinic have been previously described by Dr. Svensson.
Although the Bentall procedure is well established and has low associated mortality and morbidity, bioprostheses deteriorate over time and mechanical valves require lifelong anticoagulation, disadvantages that are especially significant for younger patients.
Multiple studies have demonstrated excellent outcomes with valve-sparing reimplantation for up to 5 years, but longer-term data are scant. The current study was designed to address the dearth of knowledge of long-term outcomes and to examine how timing of surgery affects success.
The study assessed outcomes among 643 adults up to age 70 with tricuspid aortic valves who underwent elective aortic root replacement at Cleveland Clinic from 2000 to 2017. The cohort included patients with all degrees of aortic regurgitation, from none to severe. Patients with aortic valve reoperation, aortic valve stenosis, infective endocarditis, aortic dissection or emergency surgery were excluded.
Advertisement
Outcomes were compared between 448 patients who underwent aortic root replacement with aortic valve reimplantation and 195 who underwent a Bentall operation with either a bioprosthesis (n = 147; 75%) or a mechanical prosthesis (n = 48; 25%). Mean age at operation was 48 ± 13 years in the reimplantation group and 58 ± 10 years in the Bentall group.
To account for differences in patient characteristics between the two groups, propensity matching was conducted, yielding 100 well-matched pairs for selected outcome comparisons.
Patient characteristics associated with a higher likelihood of undergoing reimplantation versus a Bentall procedure were younger age, fewer symptoms, milder aortic regurgitation (or absence of regurgitation), higher left ventricular ejection fraction and smaller cross-sectional aortic area/height ratio.
Results included the following safety outcomes:
Among the 448 patients who underwent reimplantation:
Within the propensity-matched cohort, rates of survival and freedom from reintervention were similar between the two groups at 10 years. However, the reimplantation group (which, due to propensity matching, consisted of patients with Bentall-like preoperative characteristics) had a significantly higher rate of severe postoperative aortic regurgitation than the Bentall group (7.2% vs. 0% at 8 years; P = 0.02).
Advertisement
Patients with more-advanced disease who underwent reimplantation were more likely to develop severe late aortic regurgitation than similar patients in the Bentall group. The study authors write that this suggests “potential benefits of early intervention with valve reimplantation before a large root develops with potential tearing of cusps, more severe aortic regurgitation, or symptoms.”
“Excellent results from tricuspid aortic valve reimplantation lead us to more often recommend it over the Bentall procedure, even for patients with severe aortic regurgitation and significantly enlarged aortic roots,” Dr. Svensson says. “However, success depends on a systematic approach to the procedure that addresses all the factors that contribute to aortic valve competence.”
He and his co-authors outline these factors in their study report, which presents them within the “CLASS” schema previously described by Dr. Svensson. The schema advocates careful attention to the following:
Cleveland Clinic surgeons employ modifications of the David reimplantation method — specifically, use of pledgeted sutures in the left ventricular outflow tract, use of a Hegar dilator to allow reduced anulus size, and use of figure-of-8 sutures to repair cusp prolapse during reimplantation.
“We believe these modifications to the David reimplantation result in a reproducible, reliable procedure with very good late valve function, as evidenced by these 10-year data,” Dr. Svensson concludes.
Advertisement
Advertisement

30-year study of Cleveland Clinic experience shows clear improvement from year 2000 onward

Launch of the tool promises to reshape quality assessment across the specialty

Cleveland Clinic series finds favorable long-term results with this high-risk operation
Surgeons credit good outcomes to experience with complex cases and team approach
Study indicates lower in-hospital mortality and better long-term survival

20 years of Cleveland Clinic experience in ~500 patients with proximal aortic aneurysm or dilation

Why and how we’re using robotic assistance for qualifying CABG candidates

Multicenter pivotal study may lead to first endovascular treatment for the ascending aorta