Paves way for phase 3 testing of novel treatment approach
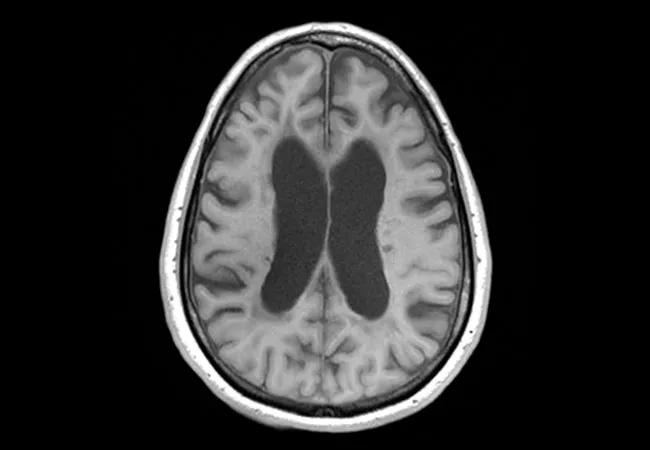
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0090314d-4d31-476a-8ebb-1098ed675b3c/17-NEU-4354-Fox-SPRINT-Study-650x450_jpg)
17-NEU-4354-Fox-SPRINT-Study-650×450
An investigational therapy for progressive forms of multiple sclerosis (MS) with a novel mechanism of action slowed progression of brain atrophy by nearly half relative to placebo over two years of follow-up. So reported investigators with SPRINT-MS, a multicenter phase 2 study presented as a late-breaking trial at the 7th Joint ECTRIMS-ACTRIMS Meeting in Paris Oct. 28, 2017. [Editor’s note: The study was published in full in the Aug. 30, 2018, issue of the New England Journal of Medicine.]
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The 48 percent reduction in brain atrophy with the oral therapy, ibudilast, compares favorably with the 18 percent reduction in brain atrophy reported with ocrelizumab, which earlier this year became the first therapy approved by the FDA for treatment of progressive MS.
“The results of SPRINT-MS are very encouraging,” says Robert Fox, MD, Vice Chairman for Research in Cleveland Clinic’s Neurological Institute and the study’s principal investigator. “Our hope is that ibudilast’s benefit in slowing brain volume loss will translate to slowed progression of physical disabilities as well. That would address a significant unmet need for people with progressive forms of MS.”
These findings will likely pave the way for larger phase 3 studies of ibudilast in progressive MS, which are needed before the drug can be considered for marketing approval for this use.
Ibudilast is a small-molecule compound that acts on three pathways that may be involved in progressive MS: macrophage migration inhibitory factor (MIF), phosphodiesterase-4 (PDE-4) and PDE-10, and toll-like receptor 4 (TLR4).
The agent has been approved in Japan since 1989 for use in asthma and cerebrovascular disorders and is also currently being studied in the U.S. for potential treatment of amyotrophic lateral sclerosis and drug addiction. Animal models suggest that it may be neuroprotective.
SPRINT-MS was conducted at 28 U.S. sites, with Cleveland Clinic’s Mellen Center for Multiple Sclerosis as lead center. The study randomized 255 patients (mean age, 56 years) with primary or secondary progressive MS to 96 weeks of ibudilast (up to 100 mg/day orally) or placebo. Patients were permitted to continue existing therapy with glatiramer acetate or interferon beta-1 agents. All had evidence of disability progression during the prior two years.
Advertisement
One primary end point was change in brain atrophy — which is associated with physical and cognitive disability in MS — as measured by the MRI analysis technique known as brain parenchymal fraction. The other primary end point was safety and tolerability.
Secondary outcomes included changes in magnetization transfer ratio (MTR) and diffusion tensor imaging (DTI), two measures of brain tissue integrity. Optical coherence tomography (OCT) studies, cortical atrophy evaluations and clinical assessments were also conducted but have not yet been analyzed.
The intention-to-treat analysis included 244 patients, and the trial had an 86 percent retention rate.
On the primary efficacy end point, ibudilast showed a 48 percent relative reduction in brain atrophy rate versus placebo (P = .04). On the secondary end point of MTR, ibudilast was associated with a 77 to 82 percent reduction in rate of decline versus placebo, with superior outcomes for normal-appearing overall brain tissue as well as gray matter. In contrast, there was no significant difference from placebo in DTI findings.
In safety analyses, ibudilast was associated with higher rates of gastrointestinal side effects, rash, depression and fatigue relative to placebo. But there were no differences from placebo in overall tolerability, discontinuation rates or rates of serious adverse events. “The drug appears to be quite safe,” Dr. Fox observes.
He notes that although SPRINT-MS was not powered to detect differences in clinical effects, measures of disability and quality of life will be forthcoming in future full-length publications of study results. “We hope this substantial 48 percent slowing in brain atrophy progression will translate to a slowing in disability progression too,” he says.
Advertisement
But phase 3 testing in larger numbers of patients is needed to determine ibudilast’s effects on clinical disability and confirm its safety profile. Dr. Fox says those results are likely about five years off.
“In the meantime, these results are promising,” he says, adding that SPRINT-MS is also helping shape the design of future phase 2 trials in progressive MS. “By evaluating for the first time the longitudinal change in multiple imaging measures and their correlation with disability, we hope to refine our understanding of the best biomarkers for future progressive MS trials.” Publication of the full study will include the OTC and cortical atrophy findings as well as effects on clinical progression, he notes.
“It looks like with this study, not only have we caught a good fish, but we’ve also learned how to fish better,” Dr. Fox says. “This should help us develop more therapies for progressive MS, and do so more quickly and efficiently.”
The study is principally funded by the NeuroNEXT Network, a clinical trials initiative of the National Institutes of Health.
Advertisement
Advertisement
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits
Newer protocols address testing, language and communication
Collaboration with AI startup promises to reshape neurocritical care monitoring at scale
Study looked at mobility measures and safety
Types and presentation may differ from adults, but early recognition and intervention are just as key
Study tests potential for a more accurate treatment predictor
Study uses molecular and clinical stratification to help guide patient selection