Key findings and proposed clinical interventions for affected areas
Waitlisting kidney transplant candidates before they begin maintenance dialysis raises their chances of transplantation, improving patient outcomes. It also has the potential to lower the cost and burden of dialysis by allowing patients the possibility of receiving a kidney transplant earlier, reducing time on maintenance dialysis. In turn, this decreases patient morbidity and boosts the chances of both graft and patient survival.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Despite these benefits, only around 30% of patients on the kidney transplant waitlist are listed pre-dialysis. According to a new study published in Clinical Transplantation, there are also small area geographic variations, where certain zip code areas in the southwest, southeast, Puerto Rico, Appalachia, and California have particularly poor rates of post-dialysis waitlisting. There also continue to be differences in kidney disease and access to kidney transplants.
In the study, lead author Robert (Blake) Buchalter, PhD, MPH, a postdoctoral fellow at Cleveland Clinic Lerner Research Institute, and his team evaluated ZIP code tabulation area hot spots of post-dialysis waitlisting for deceased donor kidney transplant candidates. Hot spots are defined as geographic areas where deferred placement on kidney transplant waitlists is far more likely than in nearby areas.
“There has been a gap in previous research related to geographic kidney transplant waitlisting differences, specifically as they relate to listing of transplant candidates after beginning dialysis,” says Dr. Buchalter. “Other studies identified larger regional patterns of transplant candidates that were waitlisted after beginning dialysis, but there were no small area granular studies, such as for ZIP code areas.”
Using data from the Scientific Registry of Transplant Recipients, the researchers performed a retrospective cohort study with deceased donor kidney transplant candidates in the United States from 2010 to 2020.
Advertisement
The candidates were categorized as preemptively (pre-dialysis) or non-preemptively (post-dialysis) registered on the transplant waitlist according to their listing and dialysis dates. Candidates were then placed into race categories and aggregated into ZIP code tabulation areas.
The total study population was 421,617 transplant candidates in 24,264 ZIP code tabulation areas. Of the total study population, 281,436 patients (66.8%) were waitlisted after beginning maintenance dialysis and 140,181 (33.2%) were waitlisted preemptively.
The researchers found small area hot spots of post-dialysis waitlisting across a wide variation of regions, including the Southeast, the Southwest, Puerto Rico, Appalachia and California.
The majority of hot spots were seen in the Southeast, including Mississippi, South Carolina, Arkansas, Texas and Georgia, “where certain racial groups are more concentrated,” says Anne Huml, MD, a nephrologist at Cleveland Clinic’s Glickman Urological & Kidney Institute and one of the study’s authors.
“I think the most surprising findings were the strong overlap of the post-dialysis listing hot spots between the various race strata and also that the overlaps were clearest in the Southeast and portions of Texas,” Dr. Buchalter says. “This further indicated to us there may be underlying drivers beyond just basic demographics, such as access to care.”
Dr. Buchalter considers this study a first step in pinpointing small areas where waitlist access could be improved. “Our work shows that even within smaller strata of waitlisting candidates, only certain geographic areas might be appropriate for clinical interventions,” he says.
Advertisement
According to Dr. Buchalter, there are some clinical interventions that can be instituted in geographic areas where variation occurs, and specifically targeted toward the hot spots identified in the study. These include:
Dr. Huml believes the study’s findings can “help us to understand the mechanisms of these differences to design effective interventions and quality improvement projects on a regional basis to help patients and improve outcomes as far as kidney transplant.”
She is currently spearheading a pilot program at Cleveland Clinic to automate early referral processes for kidney transplant waitlisting among patients who have advanced kidney disease but aren’t yet on dialysis.
“I think by shifting the paradigm to early referral for kidney transplantation, we may be able to offer patients preemptive waitlisting, meaning that patients don’t have to start dialysis prior to being evaluated and eligible for transplantation,” says Dr. Huml.
From a clinical standpoint, Dr. Huml notes that even though the study shows these hot spots of patients being waitlisted after they start dialysis, there are multiple reasons this can happen.
“It’s a little bit hard to decipher how patients finally get to the waitlist as there are many variables,” she says. “I think there are missed opportunities to capture data about referral and the evaluation process for waitlisting that may help us better understand delays in access to kidney transplant.”
Advertisement
“We hope this study serves as an impetus for further work using geospatial methods to examine kidney transplant waitlisting variations,” says Dr. Buchalter. Additionally, he notes that this methodology could be used to identify other solid organ transplant differences that have less data than kidney transplant.
“In future studies, we hope to dig further into the post-dialysis waitlisting hot spots we found and identify potential drivers of those,” Dr. Buchalter says.
Advertisement
Advertisement
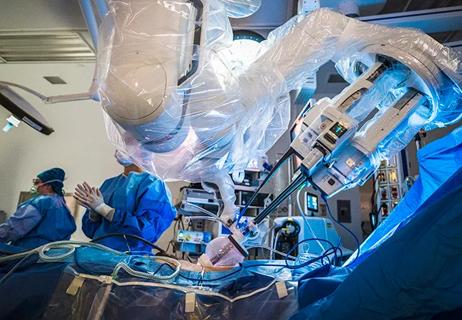
Surgeons choreograph nearly simultaneous procedures, sharing one robot between two patients
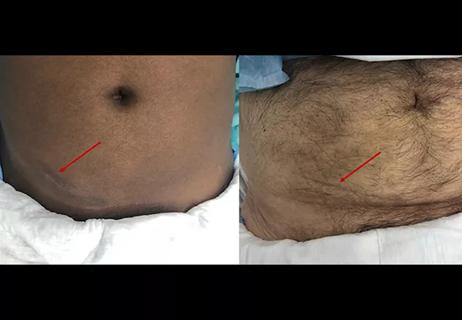
Smaller incision may lead to reduced postoperative pain for some patients
Improving access to lifesaving kidney transplant

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more

Milestone minimally invasive surgeries reduce pain and recovery time

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Enhanced visualization and dexterity enable safer, more precise procedures and lead to better patient outcomes

Insights on bringing Cleveland Clinic even closer to becoming the best transplant enterprise in the world