Tag debug info: client: {"assets":{},"datasets":{},"live":{},"projects":{},"users":{},"observable":{"assets":{},"datasets":{},"live":{},"projects":{},"users":{}}} Now: 1770671244941 Cache Key: cqdTagPageBySlug:acute-ischemic-stroke fetchCache[cqdTagPageBySlug:acute-ischemic-stroke].expirationTime: falsey fetchCache[cqdTagPageBySlug:acute-ischemic-stroke]. seconds remaining: falsey All fetchCache expiration times: -- Key: cqdNotFoundPage, seconds remaining: 1396 -- Key: cqdTagPageBySlug:oncology, seconds remaining: -13057 -- Key: cqdPostsByTag:cqd-migrated-tag-70,1,10, seconds remaining: -12962 -- Key: cqdTagPageBySlug:patient-access, seconds remaining: -11690 -- Key: cqdPostsByTag:cqd-migrated-tag-1554,1,10, seconds remaining: -11620 -- Key: cqdTagPageBySlug:xiaoxia-li, seconds remaining: -9910 -- Key: cqdPostsByTag:cqd-migrated-tag-3386,1,10, seconds remaining: -9835 -- Key: cqdTagPageBySlug:care-management, seconds remaining: -7660 -- Key: cqdPostsByTag:cqd-migrated-tag-17435,1,10, seconds remaining: -7587 -- Key: cqdTagPageBySlug:generic-medications, seconds remaining: -5358 -- Key: cqdPostsByTag:cqd-migrated-tag-1671,1,10, seconds remaining: -5290 -- Key: cqdTagPageBySlug:mesenchymal-stem-cells, seconds remaining: -3100 -- Key: cqdPostsByTag:cqd-migrated-tag-23898,1,10, seconds remaining: -3028 -- Key: cqdTagPageBySlug:wrist, seconds remaining: 1396 -- Key: cqdPostsByTag:cqd-migrated-tag-3927,1,10, seconds remaining: 1466 -- Key: cqdTagPageBySlug:residents, seconds remaining: 2707 -- Key: cqdPostsByTag:cqd-migrated-tag-24893,1,10, seconds remaining: 2787 -- Key: cqdTagPageBySlug:noninvasive-staging, seconds remaining: 4549 -- Key: cqdPostsByTag:cqd-migrated-tag-24881,1,10, seconds remaining: 4627 conditions: -- false, -- NA, -- NA, -- NA -- false Cache miss for key cqdTagPageBySlug:acute-ischemic-stroke - retrieving from Sanity CCCache.dataFetchCount: 30049 Cache cleanup seconds remaining: 6943
Advertisement
Advertisement
Tag: acute ischemic stroke
Aim is for use with clinician oversight to make screening safer and more efficient
Study links large artery atherosclerosis and delayed presentation to poorer treatment results
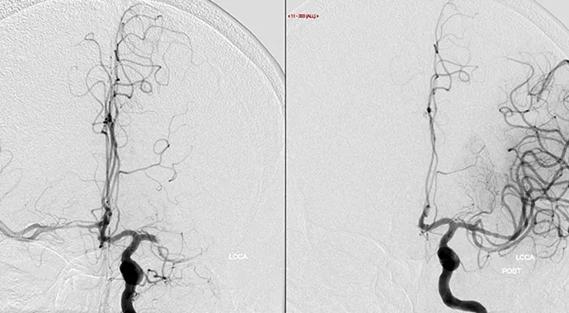
Higher complete reperfusion rate seen with tenecteplase vs. alteplase in single-center study of stroke with LVO
Retrospective looks at a “direct to angio” MSU strategy and mechanical thrombectomy beyond 24 hours
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
New interventions and medications expand options, extend treatment window
Advice on why and how based on Cleveland Clinic’s recent enterprise-wide transition
Retrospective study finds benefits of ultra-early therapy extend to this understudied subgroup
Hospital transfer compromises outcomes, and Target: Stroke proves its value
Study compares financial impacts of clinical and geographic factors
New article reviews time-to-treatment data and looks ahead to emerging outcomes and cost studies
Rendered: Mon Feb 09 2026 21:07:25 GMT+0000 (Coordinated Universal Time)
9500 Euclid Avenue, Cleveland, Ohio 44195 |
800.223.2273 | ©
2026 Cleveland Clinic. All Rights Reserved.