Tag debug info: client: {"assets":{},"datasets":{},"live":{},"projects":{},"users":{},"observable":{"assets":{},"datasets":{},"live":{},"projects":{},"users":{}}} Now: 1770470471388 Cache Key: cqdTagPageBySlug:bicuspid-aortic-valve-bav fetchCache[cqdTagPageBySlug:bicuspid-aortic-valve-bav].expirationTime: falsey fetchCache[cqdTagPageBySlug:bicuspid-aortic-valve-bav]. seconds remaining: falsey All fetchCache expiration times: -- Key: cqdNotFoundPage, seconds remaining: 4447 -- Key: cqdTagPageBySlug:ischemic-cardiomyopathy-icm, seconds remaining: -6375 -- Key: cqdPostsByTag:cqd-migrated-tag-15563,1,10, seconds remaining: -6310 -- Key: cqdTagPageBySlug:rheumatoid-arthritis, seconds remaining: -2407 -- Key: cqdPostsByTag:cqd-migrated-tag-17949,1,10, seconds remaining: -2334 -- Key: cqdTagPageBySlug:photoreceptors, seconds remaining: 902 -- Key: cqdPostsByTag:cqd-migrated-tag-24943,1,10, seconds remaining: 969 -- Key: cqdTagPageBySlug:velopharyngeal-port, seconds remaining: 4447 -- Key: cqdPostsByTag:cqd-migrated-tag-21709,1,10, seconds remaining: 4510 -- Key: cqdTagPageBySlug:mladen-golubic, seconds remaining: 7640 -- Key: cqdPostsByTag:cqd-migrated-tag-1550,1,10, seconds remaining: 7716 -- Key: cqdTagPageBySlug:fall-prevention-initiatives, seconds remaining: 9457 -- Key: cqdPostsByTag:cqd-migrated-tag-4761,1,10, seconds remaining: 9528 -- Key: cqdTagPageBySlug:arteriovenous-malformation-avm, seconds remaining: 9702 -- Key: cqdPostsByTag:cqd-migrated-tag-23124,1,10, seconds remaining: 9774 conditions: -- false, -- NA, -- NA, -- NA -- false Cache miss for key cqdTagPageBySlug:bicuspid-aortic-valve-bav - retrieving from Sanity CCCache.dataFetchCount: 3771 Cache cleanup seconds remaining: 20902
Advertisement
Advertisement
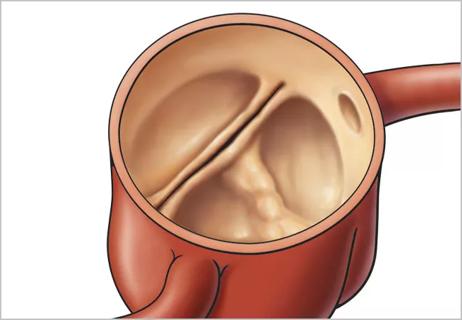
Tag: bicuspid aortic valve (BAV)
Indication, timing and options for surgical intervention
Multidisciplinary teams can deliver good short- and long-term outcomes, Cleveland Clinic experience shows
Large retrospective study supports its addition to BAV repair toolbox at expert centers
Retrospective study shows good durability of well-functioning bicuspid valves
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Series finds short-term outcomes excellent, but BAV may be less durable
Rendered: Sat Feb 07 2026 13:21:11 GMT+0000 (Coordinated Universal Time)
9500 Euclid Avenue, Cleveland, Ohio 44195 |
800.223.2273 | ©
2026 Cleveland Clinic. All Rights Reserved.