
Promising preclinical research indicates functional motor recovery is durable
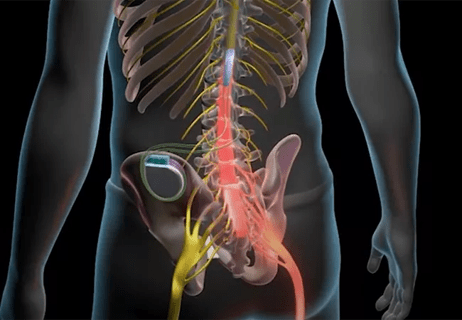
Individual needs should be matched to technological features
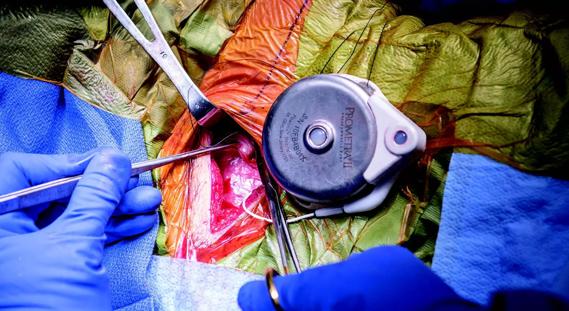
New technologies and tools offer hope for fuller understanding
When artificial tears don’t bring relief
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy

Exploring when and how to consider epilepsy surgery or neuromodulation
Randomized controlled study takes a closer look
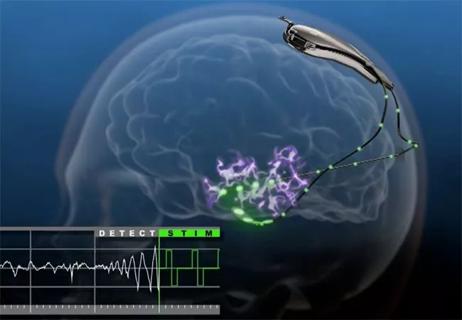
75% median reduction in seizures observed over 9 years of treatment

New neuromodulation therapy prevents over stimulation
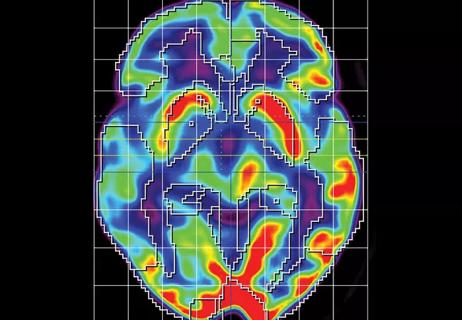
A trial status update and overview of investigational aspects
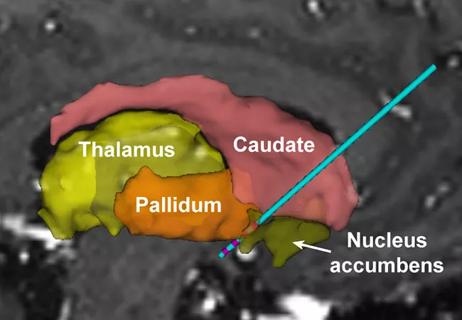
Effects specific to affective pain sphere argue for shift in surgical targeting
Advertisement
Advertisement