Training in stretches, emphasis on biomechanics help ease work-related pain, survey finds
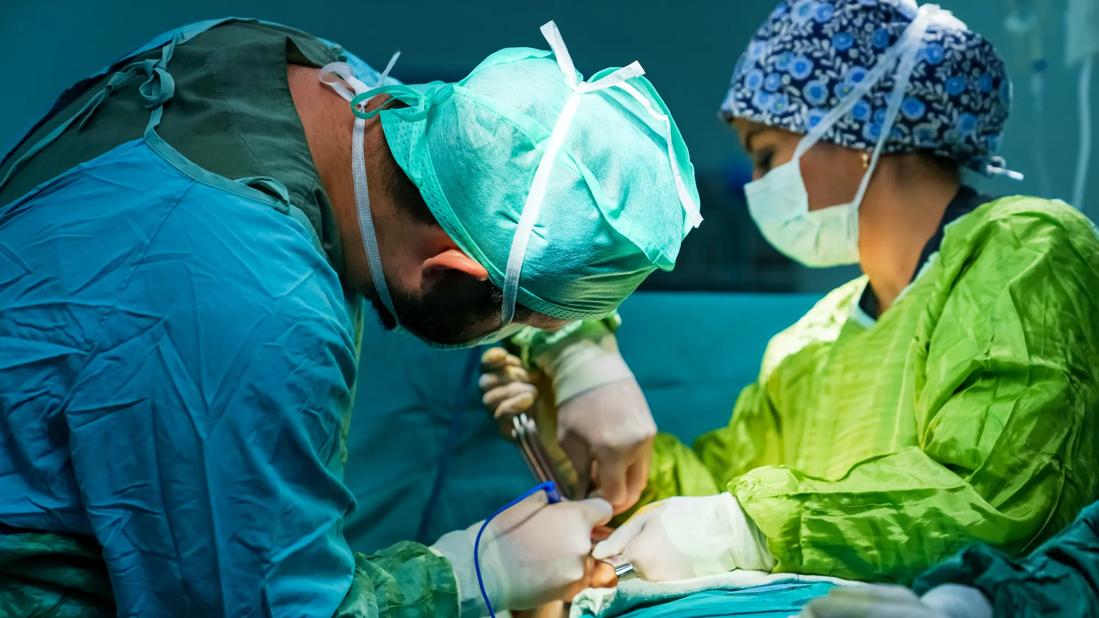
Working in the neuro-spine operating room (OR) at Cleveland Clinic requires long hours standing and the ability to move heavy patients and equipment. The lifting, pushing and pulling can be both physically and emotionally challenging for the nurses, technicians and physicians involved.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
To help the team cope in that demanding environment, the Neuro-Spine OR Safety & Wellness Initiative was created in 2021 as a multipronged approach to:
Now, a survey of nurses who completed the training shows that it is helping to address issues such as musculoskeletal pain and burnout. Before training, 96% of respondents said they had pain in the OR, but that percentage fell to 80% after the education. Prevalence of pain at home also declined, from 85% to 73% on pre-training and post-training surveys, respectively.
“This was not just a single session,” says Pamela Dixon, MOT, OTR/L, Manager of Rehabilitation Services. “As occupational therapists, we incorporated biomechanical safety and wellness education and focused on a team approach to promote best practices for caregivers before they enter the OR, during surgery and after work. For OR caregivers who are moving fast, small changes can make a big difference.”
One of the key focuses of the education was stretching exercises, according to Michael Milicia, OT/L, Clinical Team Leader. “You wouldn’t expect an athlete to run into a sports arena cold, and the same is true for the nurses in a spine OR,” he says. “I call them clinical athletes because these nurses have special knowledge about their area of practice and they are also required to perform in a physically demanding environment.”
Advertisement
In fact, the stretches were widely identified as among the most impactful parts of the training, cited by 80% of nurses surveyed, followed by information on biomechanical/posture training (cited by 73%) and changes in equipment storage (40%).
“We showed the nurses how to do stretches and provided resources on how to reduce or prevent risk factors,” says Dixon. “We also posted signs in the OR reminding them to stretch. Additionally, we have champions in the OR, like Christina Turner, ADN, RN, who have been key in supporting the education, as success requires this to be a team effort.”
According to Milicia, the nurses “need to be prepped for action by stretching before and during long procedures.” The moves in the OR — of patients and surgical instruments — should be rehearsed to maximize effectiveness and minimize risk of injury.
Survey results attest that stretches and biomechanical/posture training are being integrated into caregiver work practice and that dialogue about surgical equipment in the spine OR is ongoing. Dixon noted that besides maneuvering patients who are anesthetized, the nurses routinely deal with surgical kits that can weigh up 20 or 25 pounds. The result, she says, can be chronic shoulder and back pain that impacts nurses’ work and lives outside the OR.
Before the training, 25% of the nurses reported taking time off work for pain, compared with 0% after the training. The percentage who sought treatment for pain also fell, from 60% to 33%.
Average pain levels of respondents at work and at home, however, increased from 5 to 6 and from 4 to 5, respectively, on a scale of 10 on surveys pre- and post-training. The reason, the survey authors suspect, may be chronic or individual factors in those specific cases. Half of the respondents remain concerned about burnout and 40% about chronic pain.
Advertisement
All these ongoing issues, according to Dixon, are key aspects that need to be monitored and addressed. Among the main action points from the survey for Cleveland Clinic’s Neurological Institute are:
“Particularly in the era of COVID-19, there is an awareness that our caregivers need to be taken care of so that they, in turn, can care for patients,” Dixon notes. “One of the huge wins for the nurses from the safety initiative has been collaborating with their physician colleagues. As a result of this collaboration, more-ergonomic equipment options were identified and purchased, such as lower surgical back tables.”
Dixon adds that her team plans to survey neuro-spine OR physicians in the near future to gauge their concerns and needs related to OR safety and wellness.
“The positive trends seen in the wake of this innovative initiative are encouraging,” says Michael Steinmetz, MD, Chair of Cleveland Clinic’s Department of Neurosurgery. “While opportunities exist to further address the physical and emotional stresses unique to practice in the neuro-spine OR, acknowledging these challenges and providing training of this type is fundamental to progress in ensuring wellness among our caregivers in this care setting. We look forward to expanding similar efforts to our surgeons.”
Advertisement
Advertisement

A look at how personal stories sparked an enterprise-wide cultural reset

Interdisciplinary program fosters high-performance teams

CRNA careers offer challenge and reward

1:1 guidance benefits individuals and organization

Embrace coaching and other tips to be a stronger leader

How hospitals can weave ethics into daily nursing practice to strengthen patient-centered care

Strategies for building connections, staying present

Annual event galvanizes leaders and inspires excellence