Modified Barium Swallow Study and Flexible Endoscopic Evaluation of Swallowing can both be used to diagnose dysphagia, but it’s important to understand their advantages and disadvantages
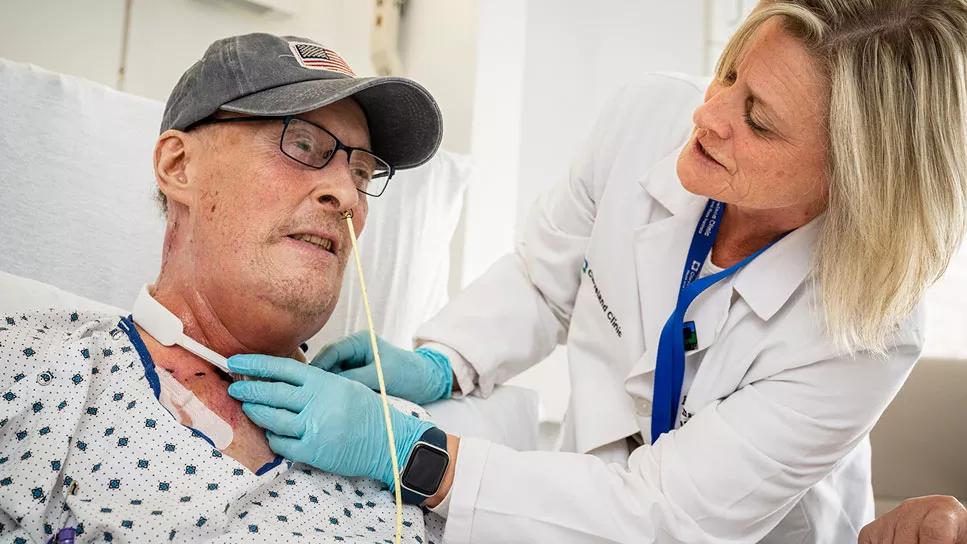
Dysphagia, or difficulty swallowing, is a common clinical challenge that can have significant implications for an individual’s health. Determining the best method to diagnose the cause of this condition has been an ongoing topic of discussion.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are two standard approaches for the evaluation and diagnosis of dysphagia: the Modified Barium Swallow Study (MBSS) and the Flexible Endoscopic Evaluation of Swallowing (FEES). While both evaluations are considered “gold standards,” it’s important to recognize and understand the differences between the two so that each can be applied correctly and appropriately.
“Every provider wants the best care for their patients,” says Martin Brodsky, PhD, ScM, CCC-SLP, Section Head of Speech-Language Pathology, Head & Neck Institute, Cleveland Clinic. “And that begins with finding the exam that meets their unique needs and will benefit them the most.
“MBSS and FEES come with their own advantages and disadvantages, and whereas one isn’t necessarily ‘better’ than the other, there are cases where one may be the preferred approach,” he explains. “Making this decision requires a clear understanding of both techniques and how they fit into clinical care.”
Below, Dr. Brodsky discusses the pros and cons of each option as well as how to not only determine the best approach but also optimize these techniques in clinical practice.
MBSS is one of two reference standards for the diagnosis of dysphagia, according to Dr. Brodsky. “It is a real-time fluoroscopic motion study used to assess swallowing physiology and airway protection,” he explains while noting that in the ideal scenario, it is performed by a speech-language pathologist alongside a radiologist—and assisted by a radiologic technologist—to effectively evaluate anatomy and swallowing physiology. There are also some constraints regarding time due to the radiation exposure for the procedure, which is typically less than 5 minutes of radiation time.
Advertisement
Comparatively, the FEES exam uses a flexible endoscope that is passed transnasally to view the pharynx and larynx during the swallowing process. This procedure allows the SLP to assess the anatomy and physiology of the nasopharynx, pharynx, base of tongue, larynx and opening of the esophagus at rest, while breathing and speaking, and while the patient is eating and drinking. Unlike MBSS, there are no associated time constraints – the duration of a FEES exam is limited only by the time available for the evaluation and the patient’s ability to tolerate the procedure, and most patients do very well.
“Both tests are conducted in real-time, but there are key differences,” says Dr. Brodsky. “FEES uses a full-color camera while MBSS uses x-ray and therefore is done in black and white. Additionally, FEES involves normal liquids and foods whereas MBSS uses barium.”
“With FEES, you are looking exclusively at the nasopharynx, pharynx and larynx. You aren’t looking at the oral cavity or the esophagus,” he adds. “MBSS allows us to examine all of those areas and the esophagus all the way down to and including the stomach.”
MBSS, like other X-ray studies, is not sensitive to soft tissues, according to Dr. Brodsky. “When you compare that to what FEES is capable of, you can see the vocal cords and all of the surrounding tissue. You can see where surgical incisions and sutures are as well as areas that have been scarred by radiation,” he explains. “You can see where nasal, pharyngeal and laryngeal structures have been removed or surgically altered a little bit easier or at least differently than with MBSS.”
Advertisement
Given the increased sensitivity associated with FEES, it may be the preferred approach for patients who have diagnoses dealing with the soft tissues, such as head and neck cancer, vocal cord disorders or airway issues.
Conversely, FEES would not be appropriate for a patient with esophagus concerns because the scope does not reach this area, notes Dr. Brodsky. Another example is glossectomy or resection of part of the tongue. “In these cases, FEES isn’t going to be the best option. It allows you to see what’s happening in the pharynx, but if you want to see the synthesis of how the bolus is prepared, manipulated, and moved out of the mouth and into the pharynx following the glossectomy then MBSS is the better study.
“It is important to emphasize that while these two exams overlap, they are not interchangeable,” explains Dr. Brodsky. “You cannot simply use one if the other is not available. Determining which exam to use depends on the clinical question and which approach is going to answer that clinical question best.”
When it comes to making diagnoses following these tests, Dr. Brodsky notes that FEES is not a standardized procedure in terms of its scoring or the protocols used to complete the exam. “As a result, it can vary from clinician to clinician, even within the same institution, and certainly across facilities,” he says. “However, the basic principles remain the same. We are making observations based on what we see during the evaluation and making clinical decisions based on the information gathered.”
Advertisement
In comparison, there is currently only one standard for the MBSS, according to Dr. Brodsky, which is the Modified Barium Swallow Impairment Profile, or MBSImP. This is a standardized approach for the instruction, assessment, and reporting of physiologic components of swallowing.
Another area where Dr. Brodsky believes FEES is particularly beneficial—and should be used more frequently—is critical care, specifically among patients in the ICU who have been extubated from oral or nasal intubation with mechanical ventilation.
One of the biggest advantages of FEES for this patient population is its portability. “It can be performed in the ICU patient’s room, eliminating delays as well as the need for a potentially difficult patient transport,” says Dr. Brodsky, who has conducted extensive research using this procedure in the ICU.
“This is where FEES shines,” he emphasizes. “Not only do you avoid the risks associated with moving a critically ill patient, but also the increased sensitivity of this test allows for the assessment of voice and laryngeal function after extubation when an injury is expected.”
It is also more convenient and cost-effective since the evaluation can be scheduled directly with the SLP and does not involve multiple departments. Additionally, FEES can be performed more frequently than MBSS — provided it is well-tolerated by the patient. The test is safe to complete, even in infants, and this includes infants who are breastfeeding.
“This is not to say that the patient won’t require a MBSS, depending on the findings but, in the immediate timeframe, there will be more than enough information to make some clinical decisions,” says Dr. Brodsky. “FEES allows you to move forward without delay and addresses the issues of swallowing, airway and voice.”
Advertisement
Although FEES is the newer evaluation of the two, Dr. Brodsky notes that he does not envision a scenario where it replaces MBSS. Rather, he argues, the two diagnostic tools are complementary and each has an important role to play.
“It’s important to remember that there are patient populations that may benefit from one versus the other,” he says while emphasizing the importance of selecting the best approach based on individual patient needs. “Also, just because you opted for one method, doesn’t mean you can’t use the other if clinically relevant questions remain unanswered. While they are most often conducted in isolation, MBSS and FEES are not mutually exclusive.”
Both procedures are currently performed at Cleveland Clinic and, according to Dr. Brodsky, there has been an eight-fold increase in the number of FEES exams conducted during his tenure—a trend he expects to continue. “I can confidently say we offer both procedures—inpatient and outpatient,” he notes while recognizing that this might not be the case at every facility.
“Access can be an issue. Ultimately, the decision to choose one approach over the other depends on availability as well as the clinical questions that need to be answered,” Dr. Brodsky concludes. “Ongoing development and training for these procedures will be beneficial for all involved, ensuring clinicians have the necessary tools at their disposal to provide comprehensive patient care.”
Podcast content: This podcast is available to listen to online.
Listen to podcast online (https://www.buzzsprout.com/2241209/13504208)
Podcast content: This podcast is available to listen to online.
Listen to podcast online (https://www.buzzsprout.com/2241209/13504207)
Advertisement

25-year series of over 1,000 patients reveals good long-term palliation, esophageal preservation

Case highlights the benefits of a minimally invasive approach

3 pediatric gastroenterologists discuss advances in their diagnostic toolkits
Going beyond the Eckardt symptom score to evaluate dyspepsia, eating and symptom “bother”

Microvascular “supercharging” is a critical newer step to promote favorable outcomes

Promoting accessibility for all children

Research could help direct care pathways for patients with unexplained swallowing difficulties

Potential for new, non-invasive screening option