Clinicians must navigate options as more patients qualify for CGM
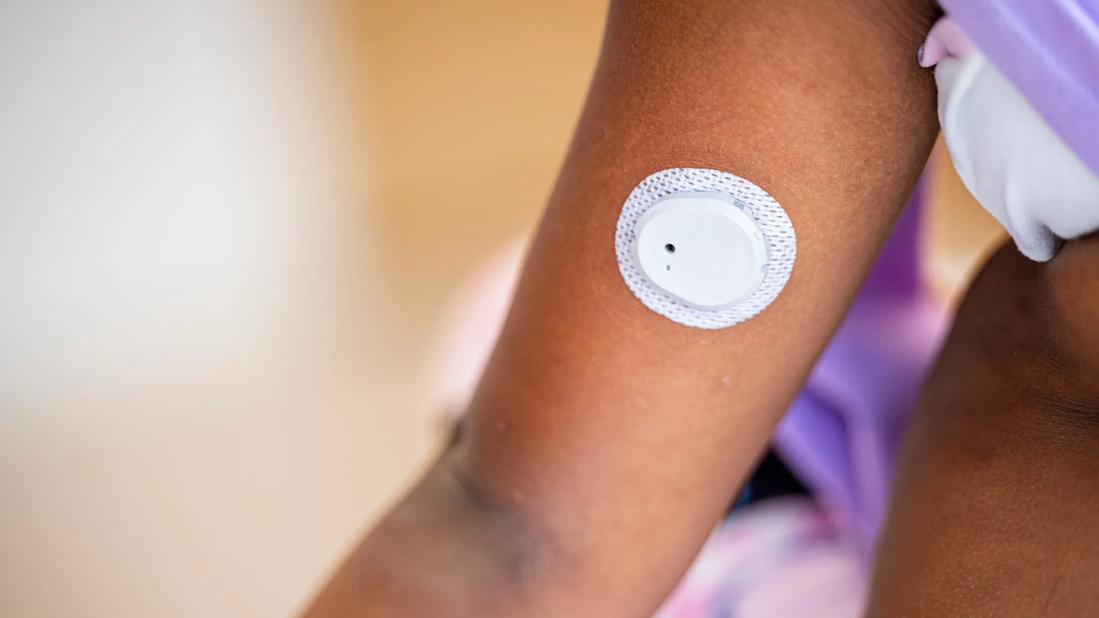
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/06e7c7c4-2212-4af6-ae10-1ce5fc1b5a19/CHP_5223060_09-13-24_057_SCG)
Continuous Glucose Monitoring
A new policy from the Centers for Medicare & Medicaid Services (CMS) vastly expands coverage for continuous glucose monitoring (CGM), putting better type 2 diabetes management within reach for millions more patients. That makes it more important than ever for clinicians to stay current on technology and to find solutions to CGM-related challenges.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As of April 16, 2023, Medicare provides device coverage for anyone who takes insulin, as well as for patients who are not on insulin but have problematic hypoglycemia. Previously, CGM was covered only for those who required mealtime insulin.
The change is good news, says Diana Isaacs, PharmD, a Cleveland Clinic clinical pharmacy specialist. Dr. Isaacs advocates passionately for CGM and other technologies that help patients with diabetes.
“This is really is going to open the floodgates, because there have been so many people who were not on mealtime insulin who now will meet the criteria for coverage,” Dr. Isaacs says. “Commercial insurance often takes the lead from CMS, so hopefully we will see CGM coverage expand with commercial insurance as well.”
Better glycemic control is critical to reducing morbidity and mortality for those with diabetes, says endocrinologist Mary Vouyiouklis Kellis, MD.
“Over 30 million people have diabetes, and 90% of those have type 2 diabetes. Improving hyperglycemia is crucial to helping reduce the risk of microvascular and macrovascular complications,” Dr. Kellis says. “A recent study in JAMA1 showed that patients with type 2 diabetes on basal insulin who were using a CGM had a significant reduction in A1C levels compared to those using standard blood glucose meters.
“Previously, the CGM coverage was for patients on multiple insulin injections daily. Expanding coverage to include those on basal insulin is a great move forward. Not only has CGM been shown to reduce A1C, but it can also reduce hypoglycemia, as many of the newer monitors can notify patients when blood glucose begins to go low, so the patient can take action.”
The policy update is the latest in a series of moves that have made CGM more accessible. In Ohio, Medicaid recently started covering CGM for all people with diabetes, regardless of what medications they take. Manufacturers also have helped with programs that that limit out-of-pocket costs for people with commercial insurance.
According to the Centers for Disease Control and Prevention, diabetes is the most expensive chronic condition in the United States.
Advertisement
“The data now confirm the A1C benefits of CGM for those on basal insulin as well as for people with hypoglycemia,” Dr. Isaacs says. “You’re going to save on emergency department visits and hospitalizations. With the robust data that we have, and the fact that the devices have come down in price, it totally makes sense to cover CGM.”
With that said, increase demand will require flexibility from clinicians, especially those in practices that haven’t had much experience with CGM. The shortage of endocrinologists in the United States makes the challenges more complex.
“Most of diabetes care is delivered by primary care providers,” Dr. Kellis says. “Many providers may not feel comfortable prescribing CGM, because, depending on the patient’s insurance, these prescriptions may need to go through a durable medical equipment provider. In addition, some providers may not have the software in their offices to be able to access patient data.
“Moreover, there is a learning curve with understanding the ambulatory glucose profiles that are downloaded from these CGMs,” Dr. Kellis adds. “These may be obstacles to prescribing CGMs for these patients. Informing and educating providers will be important to help increase accessibility of CGM to patients who have diabetes.”
Data management presents another challenge. CGMs capture lots of data. Medical teams need to learn to access it through a dashboard and ensure that patients have access, too.
“The data usually does not go straight to the electronic medical record. This means logging into separate systems and pasting notes from one platform into another,” Dr. Isaacs says. “So it is extra work.”
Advertisement
If patients are on different systems, then the team must learn different dashboards.
“These are all issues I worry about,” Dr. Isaacs says. “I see all the benefits of CGM, but everyone in healthcare is already operating at their maximum level. How do you add to that?”
With that said, she believes that extending the extra effort is worthwhile.
“We know about the limitations of A1C alone, so CGM is worth pursuing,” Dr. Isaacs says. “But we have to come up with systems to make this easier.”
Three areas of focus can help medical teams in their efforts to transition patients to CGM.
If possible, select a team member to take the lead on managing portal access and ensuring everyone is connected. This could be a pharmacist, nurse or diabetes educator.
A1C numbers have been the standard for a long time, but learning to look at CGM data, specifically for time-in-range information, is key, Dr. Isaacs says. “We’re aiming for patients to spend 70% or more time in the target blood glucose range, and to minimize hypoglycemia. The ambulatory glucose profile report is just one page and includes everything you need for interpretation”
“Selecting the right device is really important,” says Dr. Isaacs. “Some places pick a technology they like and decide that’s what they’re using, take it or leave it. We should be making sure that we take into consideration all the different factors — the patient’s needs and lifestyle, as well as the features of various devices — and make the best match for the patient.”
Advertisement
The most popular CGMs are FreeStyle Libre and Dexcom, and then Medtronic Guardian for those using Medtronic pumps, Isaacs says. Eversense is trying to grow. “It’s great to have options,” Dr. Isaacs says.
She also recommends online tools to help with decision making. DiabetesWisePro offers information and resources for healthcare providers. DiabetesWise aims to help patients understand their device needs. “I always encourage people to go learn about the different systems, to see what they think and what’s important to them,” she says.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/4d8e281b-30f2-45b9-b674-921b6fbe5531/23-EMI-3658673-CQD-Inset-Chart-800x1200-1-683x1024_jpg)
Notes:
1. Martens et al. JAMA. 2021;325 (22):2262-2272.
Advertisement
Advertisement
Patient’s unexplained low blood glucose levels in the absence of diabetes spark quest for answers
Cleveland Clinic endocrinologists work to identify protocols for improving care
New service for patients with diabetes will make annual screening more convenient
Retrospective analysis finds lower mortality rates, fewer hospital visits among patients with Type 1 diabetes using GLP-1 Therapies
The advanced stage of diabetic retinopathy is among the most challenging for retinal surgeons
Meta-analyses signal an opportunity to reshape risk stratification and surgical protocols for these comorbidities
Association revises criteria for the diagnosis and resolution of severe conditions
While results were negative for metformin, lifestyle counseling showed surprising promise