Improvements in patient care, research and education set the stage for a promising future
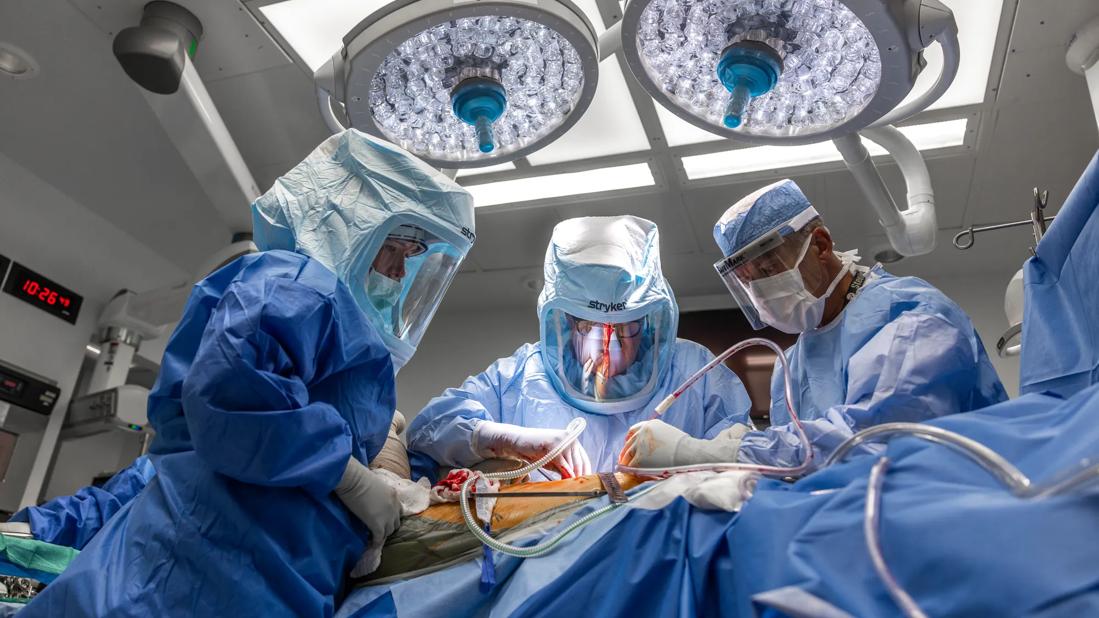
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/49e645c3-0223-48f6-8085-09c97d1223e3/CCC_5367218_06-05-24_1036_AMO)
Ortho surgery
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cleveland Clinic’s rich, patient-centered history began 100 years ago. Even then, innovation was the cornerstone of our academic healthcare mission. It has enabled us to create a culture that drives improvements in patient care, leads breakthrough research and provides exemplary training.
In orthopaedic surgery, specifically, this culture of innovation gave rise to several notable accomplishments in the last century — from early work in carpal tunnel diagnostics and the advent of sports medicine to surgical innovations that became the gold standard, and more.
Some of our most meaningful accomplishments include:
Advertisement
In this same spirit of innovation, last year we increased utilization of virtual visits, created a self-scheduling platform and expanded our centers of excellence and robotic-assisted surgeries. We are exceedingly proud of our history and are heartened by the future possibilities in delivering care.
Dr. Patterson is Chair of the Department of Orthopaedic Surgery in Cleveland Clinic’s Orthopaedic & Rheumatologic Institute. His specialty areas include limb salvage, complex fractures, adult reconstruction, hip and knee replacements.
Advertisement
Advertisement
Protein expression in synovial fluid indicates patients’ immune factors may be involved
Cleveland Clinic’s Global Peak Performance Center and PGA TOUR partnership pair advanced assessment with longitudinal follow-up to enhance clinical decision-making
Study highlights the need for objective functional measures as value-based care expands
Reduces likelihood of achieving CMS-defined substantial clinical benefit at one year
Step counts suggest recovery is more variable and individualized than commonly believed
Innovations and practical insights for safe return to sport after lower-limb injury
Physical therapy before surgery is intended to optimize outcomes after surgery
Recognition could help guide health policy, workforce development and resource allocation worldwide