A case study in pairing imaging acumen with subspecialty expertise to yield answers and symptom relief
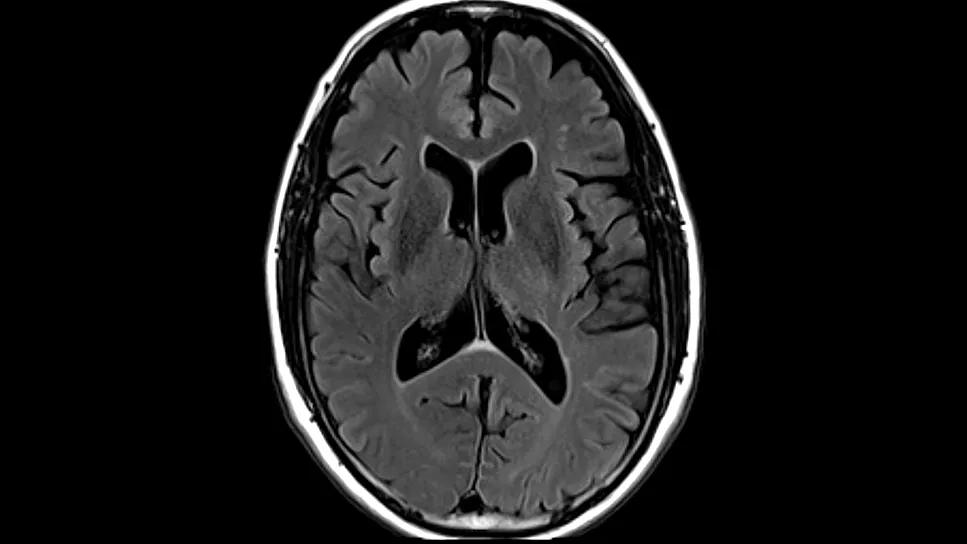
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/863646bc-367e-454b-b11b-10a5372d7fbe/brain-mri-volumetric-hero)
MRI of the brain against black background
In January 2021, a 68-year-old male was referred to Dylan Wint, MD, Medical Director of Cleveland Clinic Lou Ruvo Center for Brain Health in Las Vegas, by his primary care provider. The patient was experiencing fluctuations in thinking, apathy, headaches and dizziness upon standing.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The patient was very accomplished in the computer field, and he was having trouble understanding technical details that used to come to him very easily,” says Dr. Wint, a behavioral neurologist and neuropsychiatrist. “He was also having trouble with his balance and walking.”
During the initial assessment, Dr. Wint administered the Montreal Cognitive Assessment, a 30-point screening tool, to assess for mild cognitive impairment and early dementia. Although the patient scored a 29, Dr. Wint notes that “some people who are very intelligent can perform really well on the test even though they have lost a considerable amount of their abilities.”
A motor exam was also performed. “He had a bit of an action tremor, but we couldn’t really detect problems with his movement or see any clear issues with his gait,” Dr. Wint says. “The patient was sensing issues, but it was hard to get objective evidence.”
Dr. Wint ordered an FDG-PET scan, which measures cerebral glucose metabolism in different brain regions to assess for degenerative disorders; a dopamine transporter (DaT) SPECT scan; and a neuropsychological evaluation. He also requested the images from a previous MRI scan.
The DaT and PET scans were normal. When the outside MRI became available, the report said it was normal, but Dr. Wint wasn’t convinced. “One condition that can cause difficulties with cognition, balance and walking is progressive supranuclear palsy [PSP], which is associated with atrophy of the midbrain,” Dr. Wint explains. “Using measuring tools in our imaging portal, the patient’s midbrain measured 9.0 mm,” below the normal range of >9.5 mm.
Advertisement
Dr. Wint’s neuropsychologist colleagues at the Lou Ruvo Center for Brain Health performed more than a dozen assessments, including the Beck Anxiety Inventory; Boston Naming Test; Delis-Kaplan Executive Function System; Geriatric Depression Scale; Hopkins Verbal Learning Test – Revised; Wechsler Adult Intelligence Scale, 4th edition; and Wide Range Achievement Test, 5th edition. The results were unremarkable.
To evaluate for brain shrinkage and to verify his measurement of the midbrain, Dr. Wint ordered a volumetric MRI scan, which automatically calculates the sizes of different brain regions and compares them with those of other people of the same age. Unfortunately, volumetric analysis was not covered by the patient’s insurance company. The routine MRI scan was uninformative.
Dr. Wint considered normal pressure hydrocephalus, but the lack of the usual imaging findings left this suspicion inconclusive. “With normal pressure hydrocephalus, typically you see enlarged ventricles, but the ventricles did not look unusual on the imaging we had at the time,” he says. “We were not able to detect a cause of what was going on, so we decided to follow the patient.”
At two additional patient visits in 2021, not much changed. In June 2022, Dr. Wint referred the patient to Cleveland Clinic Nevada’s movement disorders service because of his action tremor as well as his continuing dizziness upon standing and orthostatic hypotension. Zoltan Mari, MD, the Ruvo Family Chair and Director of the Parkinson’s Disease and Movement Disorders Program, diagnosed the patient with orthostatic tremor.
Advertisement
“That’s a rare condition that causes rapid muscle contractions in the legs when standing,” Dr. Wint notes. “We are fortunate to have a team of movement disorder subspecialists at the Lou Ruvo Center for Brain Health because I certainly would not have picked up on that.”
By 2023, the patient’s condition had worsened. He fell in January and broke his collarbone and a rib. The patient, who required a catheter to urinate, also began experiencing urinary leakage.
“I once again requested a volumetric MRI to give us a chance at understanding and treating this man’s symptoms,” says Dr. Wint.
In March 2023, in hopes of resolving his quest for a definitive diagnosis, the patient elected to self-pay for a volumetric MRI at the Lou Ruvo Center for Brain Health. The volumetric analysis indicated that he had enlarged cerebral ventricles. Enlarged ventricles can be seen in normal pressure hydrocephalus, along with symptoms of Hakim’s triad — cognitive decline, gait disturbance and urinary incontinence. Normal pressure hydrocephalus, which is caused by cerebrospinal fluid (CSF) buildup in the brain, affects approximately 0.2% of people between 70 and 80 years of age. Since the patient now had its three primary symptoms, a diagnosis of normal pressure hydrocephalus was plausible.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f62f13fa-c6a4-49cc-8651-e93602b43dd0/brain-mri-volumetric-inset-1)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1c77e5e6-bc65-492e-9f81-e3ab14aa1a66/brain-mri-volumetric-inset-2)
Representative images from the patient’s volumetric brain MRI.
The patient underwent a therapeutic lumbar puncture in July 2023, which temporarily alleviated his symptoms, suggesting a shunt could provide long-term relief. In September 2023 he had a ventriculoperitoneal shunt surgically implanted to divert CSF from the lateral ventricles into the peritoneum.
Advertisement
During a February 2025 appointment with Dr. Wint, the patient noted that he had remained symptom-free since the shunt placement 17 months earlier.
“While he has other health issues, including a new diagnosis of Ehlers-Danlos syndrome, he is very grateful that his normal pressure hydrocephalus was discovered and treated,” says Dr. Wint. “The patience and persistence of the patient and our team in trying to find a solution for him were really important.”
Offering advanced diagnostic imaging is a pivotal component to finding solutions for patients. Every individual who comes to the Lou Ruvo Center for Brain Health with memory problems undergoes neuroimaging for two primary reasons, Dr. Wint says. First, degenerative conditions that cause cognitive decline have varying imaging characteristics that can be detected when the center’s subspecialty radiologists review the images. Second, appropriate neuroimaging helps neurologists answer common questions that patients ask.
“The fundamental things patients want to know are, ‘Is what’s going on normal? If it’s not normal, is it fixable? And whether it’s fixable or not, what are we going to do about it?’” says Dr. Wint. “Advanced brain imaging can provide objective measures, supplement our evaluations and give us a lot of those answers.”
Advertisement
Advertisement
Technology helps address gait abnormality in normal pressure hydrocephalus and more
Large analysis of familial cases and genomic studies sheds light on genetic contributions
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Insights from one of the first studies of invasive monitoring in the rare form of focal cortical dysplasia
Guidance from the largest cohort of SEEG-confirmed insular epilepsy patients reported to date
Despite less overall volume loss than in MS and NMOSD, volumetric changes correlate with functional decline
Researchers pair quantitative imaging with AI to improve surgical outcomes in nonlesional epilepsy
Promising preclinical research indicates functional motor recovery is durable