Percutaneous vertebral augmentation proves safe and effective
By Ryan Goodwin, MD; David P. Gurd, MD; Rabi Hanna, MD; and Thomas E. Kuivila, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Osteopenia and osteoporosis are common side effects of both steroid use and chemotherapy in children and adults. Both conditions can potentially lead to vertebral compression fractures. Vertebral compression fractures can be a significant source of debilitating pain, psychosocial decline and physical impairment in patients of all ages.
Vertebroplasty and balloon kyphoplasty are percutaneous vertebral augmentation techniques that have been used extensively with good to excellent results in adults to control pain following vertebral compression fractures. To date, their use in children has been limited, and few studies and no formal indications exist.
We retrospectively reviewed outcomes for three pediatric patients who underwent balloon kyphoplasty at our institution to address their intractable pain from vertebral compression fractures between 2007 and 2013. Our results were published in the Journal of Pediatric Othopaedics.
The underlying diagnoses for these patients (average age 12.3 years, all male) were:
Preoperative pain scores were very severe (8 to 9 on a 10-point scale), impacting the children’s ability to independently ambulate. One patient even required elective intubation due to respiratory distress secondary to pain. Two of the three patients underwent multilevel procedures.
At an average of 3.6 weeks postsurgery, patient pain was improved to an average of 2/10. Two of the three patients were able to sit, stand and walk independently at follow-up. The third patient (with IPEX-like syndrome) was successfully extubated one-week postoperatively. He was capable of normal activity, including playing basketball, at follow-up about two years after balloon kyphoplasty treatment. No complications were encountered in this small case series.
Advertisement
Our follow-up was short in two of the three patients because of their early demise due to underlying oncological disease.
In our series, balloon kyphoplasty dramatically decreased pain and increased function in the immediate postoperative period in each of the patients treated. This small study provides initial information on the usefulness and safety of this procedure in this subset of seriously ill patients.Further research is necessary to establish indications for balloon kyphoplasty in pediatric patients.
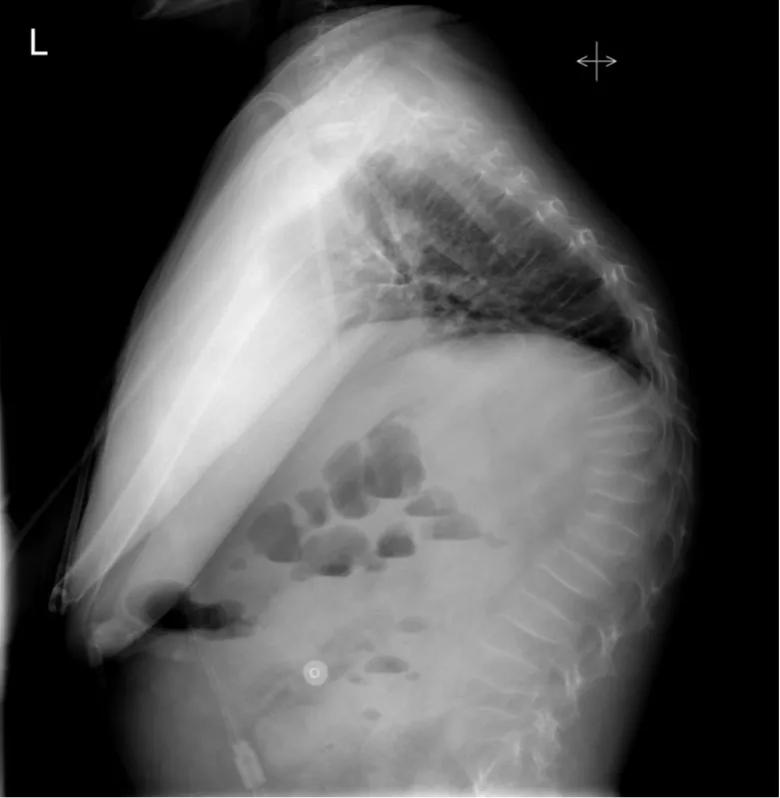
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7a4bd40c-acb6-4317-a254-de22966466ab/17-ORT-1802_inset1_jpg)
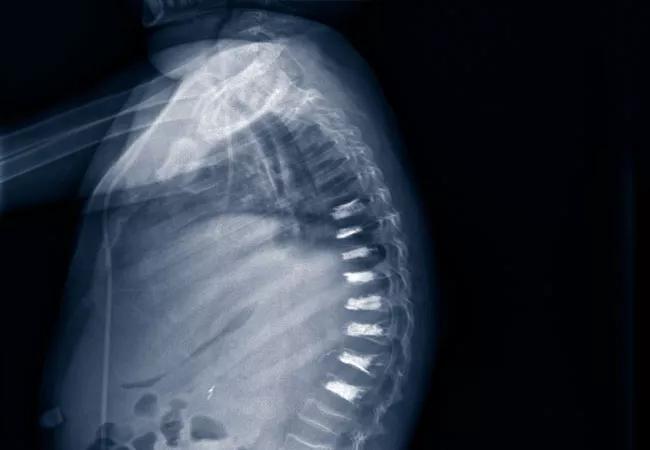
Figure 1A. A 13-year-old male with IPEX-like syndrome presented with severe thoracic and lumbar back pain in the setting of prolonged high-dose steroid use. Numerous vertebral compression fractures in the lower thoracic and upper lumbar regions were identified. The patient was electively intubated due to respiratory distress, thought to be related to his refractory pain.
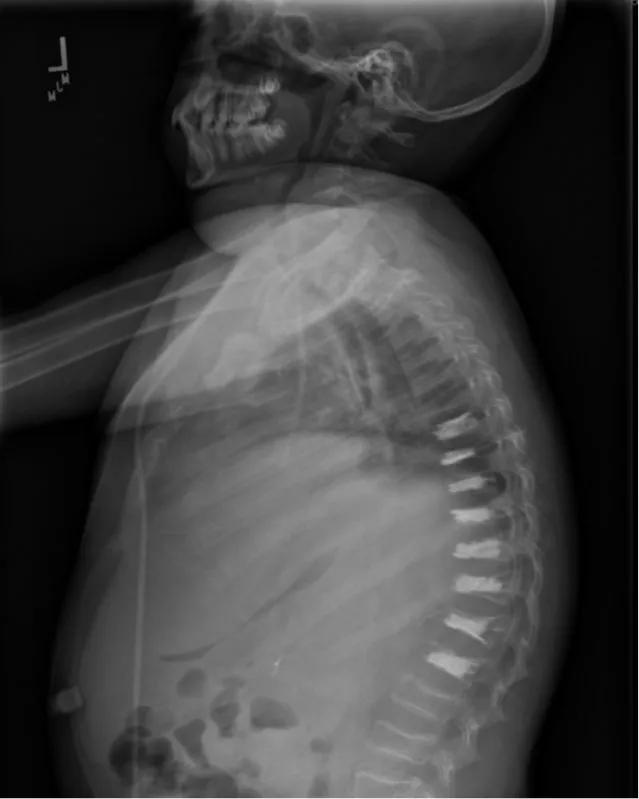
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d0d4f3f1-da5a-451e-9d8e-75a3738337fa/17-ORT-1802-inset2_jpg)
Figure 1B. The patient underwent four-level balloon kyphoplasty in two stages, separated by one week. His kyphotic deformity and pain improved dramatically postoperatively, allowing him to sit without pain within one month and walk independently within two months.
Dr. Goodwin is Director, Center for Pediatric and Adolescent Orthopaedics; Dr. Gurd is Head of Pediatric Spinal Deformity Surgery; Dr. Kuivila is staff physician, Pediatric Orthopaedic Surgery, Vice Chair for Education, Orthopaedic & Rheumatologic Institute, and Residency Program Director, Orthopaedic Surgery; Dr. Hanna is Director, Pediatric Bone Marrow Transplantation, Department of Pediatric Hematology and Oncology, Cleveland Clinic Children’s Hospital.
Advertisement
Advertisement

How it’s similar but different from the direct anterior approach

Collaboration must cross borders and disciplines

Systematic review of MOON cohorts demonstrates a need for sex-specific rehab protocols

Should surgeons forgo posterior and lateral approaches?

How chiropractors can reduce unnecessary imaging, lower costs and ease the burden on primary care clinicians

Why shifting away from delayed repairs in high-risk athletes could prevent long-term instability and improve outcomes

Multidisciplinary care can make arthroplasty a safe option even for patients with low ejection fraction

Percutaneous stabilization can increase mobility without disrupting cancer treatment