Subtle but important distinctions for ophthalmologists
A 65-year-old woman presented at Cleveland Clinic Cole Eye Institute with symptoms of ocular migraine. She reported a pixelated area in the visual field of her left eye. The phenomenon was transitory, but was increasing in frequency, lasting from seconds to minutes. Most recently, she had experienced a total loss of vision in her left eye, lasting for approximately 30 minutes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Patients with ocular migraine have described the visual aura in various ways, including “seeing sparkles,” shimmering and “like a kaleidoscope.” Some patients report having blind spots. Symptoms typically last less than an hour. Sometimes the visual aura can be followed by a headache. Patients may have a history of migraine.
“Ocular migraine symptoms, such as scintillating scotoma, are usually bilateral,” says ophthalmologist Nicole Bajic, MD, of the Cole Eye Institute. “Even if patients initially report symptoms in only one eye, upon further investigation they often will identify symptoms in the second eye. That didn’t happen with the patient in this case, however. She had checked each eye and insisted that her symptoms were unilateral.”
A dilated fundus exam often can reveal ischemia, which sometimes causes symptoms similar to an ocular migraine. Ocular migraine is a diagnosis of exclusion after an unremarkable exam.
“If there’s an ischemic issue, on a dilation exam you’ll often see spots of blood in the midperiphery of the retina,” says Dr. Bajic. “There also may be other signs of insufficient blood flow to the eye, such as neovascularization in the anterior segment.”
While the patient in this case had no remarkable findings on fundus exam, the unilateral symptoms and temporary loss of vision caused Dr. Bajic to suspect a vascular diagnosis rather than ocular migraine.
“My suspicion was based totally on the symptoms she had described to me,” says Dr. Bajic. “The patient was preparing for a trip out of town, but I urged her to go to the ED right away and then placed orders for blood tests, a CT/CTA and a possible echocardiogram.”
Advertisement
In the emergency department, the patient had a CT/CTA scan of the head and neck that revealed severe atherosclerosis of the carotid arteries — 85% blockage on the left side and 45% blockage on the right. Vascular surgeon Javier Alvarez-Tostado, MD, diagnosed the patient with symptomatic carotid stenosis and left amaurosis fugax (temporary vision loss) due to restricted blood flow to the retina. The patient was admitted to the hospital and scheduled for a carotid endarterectomy.
Amaurosis fugax may or may not be due to a vascular condition. In this case, stenosis of the left carotid artery had caused transient ischemia of the central retinal artery, a branch of the carotid.
“Some plaque or a blood clot can block circulation to the retina, causing loss of vision,” says Dr. Alvarez-Tostado. “It can be transitory, as in this case, or it can cause complete occlusion and damage to the retina.”
Narrowing of the carotid artery likely had been progressing throughout the patient’s life, he says. While visual complaints are not common in vascular stenosis, amaurosis fugax has been known to be a classic symptom of occlusive carotid disease.
“Losing vision for 30 minutes is much longer than we typically see in amaurosis fugax due to underlying carotid disease, which is typically seconds to minutes of vision loss,” says Dr. Bajic. “This patient’s symptom duration actually was more typical of an ocular migraine. However, the increasing frequency and severity of symptoms only in the left eye are what prompted me to send her to the ED. The total blackout of vision in the most recent episode was the most concerning.”
Advertisement
Within days of diagnosis, Dr. Alvarez-Tostado performed the endarterectomy. An incision in the neck exposed the carotid artery. After clamping the artery above and below the occlusion, he removed the plaque and repaired the artery with a patch.
One month later, at her follow-up visit with Dr. Alvarez-Tostado, the patient reported no further episodes of amaurosis. She was symptom-free, and ultrasound showed that her left carotid artery was patent. At her follow-up visit with Dr. Bajic, the patient had no damage to the retina.
“This patient’s condition was severe and symptomatic,” says Dr. Alvarez-Tostado. “Carotid blockage that is symptomatic increases risk for a major stroke. In this case involving ocular symptoms, the patient was also at risk for retinal damage.”
Typically, patients with symptomatic blockage are referred for vascular surgery, as are asymptomatic patients with a blockage of 80% or greater.
This case illustrates the value of eye exams in detecting life-threatening health conditions.
“It’s important to conduct a dilation exam when patients have suspected ocular migraine, to help rule out ischemic causes for the symptoms,” says Dr. Bajic. “While in this case the results of that exam didn’t indicate ischemia, I was not convinced. Worsening severity and frequency of symptoms leading to a total blackout of vision is not normal and should prompt further workup or evaluation.”
Indications that visual symptoms may be due to ischemia rather than ocular migraine include:
Advertisement
“This was an unusual presentation,” says Dr. Bajic. “The patient’s exam findings did not support severe arterial stenosis, but listening to the patient and considering the overall clinical picture helped us provide the correct care and ensure a favorable outcome.”
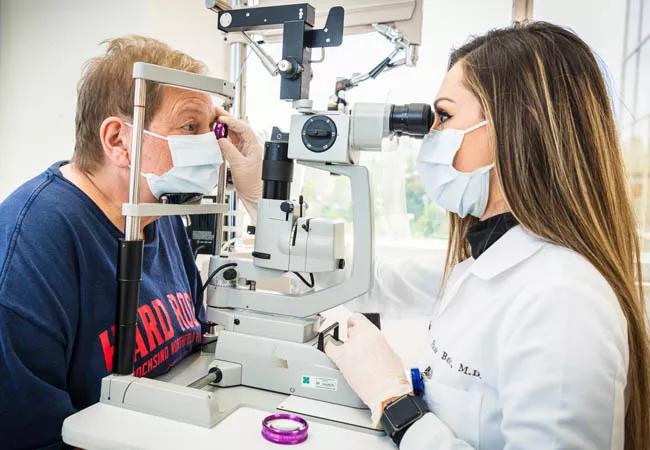
Pictured above: Nicole Bajic, MD, an ophthalmologist at Cleveland Clinic Cole Eye Institute, examines a patient one month after endarterectomy. An 85% blockage in the patient’s left carotid artery had caused visual aura originally thought to be ocular migraine.
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more