A recently published case series highlights the broad range of laryngeal findings that can present among individuals with EDS
Given an increase in reports of laryngeal complaints among patients with Ehlers–Danlos Syndrome (EDS) and limited literature on the topic, a team of experts — led by Michelle Adessa, MS, CCC-SLP, a speech-language pathologist in Cleveland Clinic’s Voice Center — sought additional insights into these patients and their needs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
An inherited connective tissue disorder, Ehlers–Danlos Syndrome involves joint hypermobility, skin extensibility and tissue fragility. While rare, EDS patients can present with laryngological issues such as as hoarseness, dysphonia, dysphagia and vocal fold hemorrhage.
Adessa and colleagues initiated a case series, “Laryngological Symptomatology in Patients with Ehlers–Danlos Syndrome,” which was recently published in The Laryngoscope. They examined the laryngological presentations, comorbidities and related findings of patients referred to Cleveland Clinic’s otolaryngology clinic.
Adessa and colleagues conducted a retrospective chart review of nine EDS patients who presented to Cleveland Clinic with laryngological complaints between 2019 and 2022. Of the identified patients, eight had hypermobile EDS.
The mean age was 33 years old, and eight of the nine patients included in this analysis were female. Additionally, six of the patients were singers, and one other participant reported high voice demands due to their position as a mental health counselor. Eight of the patients underwent videostroboscopy.
Eight patients presented with dysphonia, or hoarseness and straining of the voice. Other common complaints included dysphagia in five patients and laryngospasm in three individuals. EDS can be associated with a number of comorbidities. Conditions observed in this patient cohort included gastroesophageal reflux disease (GERD), postural orthostatic tachycardia syndrome (POTS), fibromyalgia and vagal nerve sensitivity, to name a few.
Advertisement
Among the patients with dysphonia, four had abnormal findings on videostroboscopy — three had bilateral midfold swellings and one had vocal fold edema. According to Adessa, all four were professional voice users.
“The patient with fold edema had a history of bilateral vocal cord nodules that were treated with microsurgical excision of the nodules. However, her hoarseness persisted following surgery,” says Adessa. “A mild improvement in phonation was observed after voice therapy and two rounds of steroid injections.”
Of the five patients with dysphagia, four underwent modified barium swallow studies, which showed normal swallow function. While two received swallowing therapy and function improved, the other two patients had underlying functional GI pathology and were referred to gastroenterology. The fifth patient had dysphagia and episodes of hyoid bone dislocation, according to Adessa and colleagues, who reported that the patient was referred to speech language pathology for further intervention.
Two of the three patients with laryngospasm were diagnosed with vagal nerve sensitivity and chronic cough. They were subsequently treated with superior laryngeal nerve blocks. One patient, who presented with dysphagia, laryngospasm and throat tightness, underwent successful voice and swallowing therapy.
The analysis offers important insights into this patient population, highlighting the broad range of laryngeal findings that can present among individuals with EDS. “While there are rare laryngological complaints that appear to be more common among EDS patients, such as hyoid bone dislocation due to hypermobility, most patients with EDS may have presentations that are similar to others in the laryngology clinic,” according to Adessa.
Advertisement
This research underscores the association between laryngological symptoms and other comorbidities in patients with EDS. “We must view these patients through a holistic lens,” says Adessa, while emphasizing the importance of interdisciplinary assessment and management. “Our research speaks to the need for collaboration across disciplines to ensure the best outcomes and quality of life for our patients.”
Part of that interdisciplinary effort is asking patients the right questions, notes Adessa. “If I have patients presenting with these symptoms, I will ask questions regarding EDS because if the patient doesn’t think it is related to their throat complaints, they may not bring it up,” she explains.
“Here at Cleveland Clinic, this allows us to make sure they are receiving appropriate care,” Adessa says. “We have the resources to help treat these patients and together we can establish a clear pathway of care and support.”
Moving forward, Adessa and colleagues plan to continue their work to better understand patients with Ehlers–Danlos Syndrome and their unique care needs. “Our next steps include defining particular treatment modalities to better support this patient population.”
Advertisement
Advertisement

Recommendations on identifying and managing neurodevelopmental and related challenges

Phenotypic clustering study reveals four distinct disease trajectories

Rare genetic disorder prevents bone mineralization

Oral medication reduces epistaxis and improves quality of life for patients with rare vascular disorder
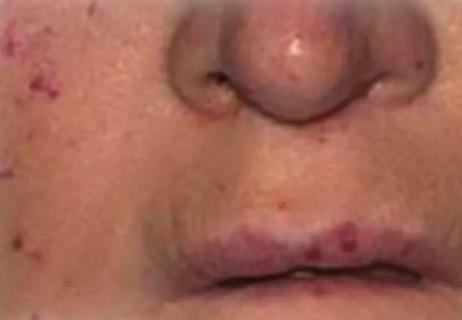
The disorder can greatly impact patients’ quality of life, but sclerotherapy and a multidisciplinary approach to care can be life-changing

Microvascular “supercharging” is a critical newer step to promote favorable outcomes

National database study reveals insights into survival outcomes

New innovations in upper airway care and insights into the Pediatric Voice Center