Despite wide variations in contours, researchers find AI and physician methods yield equivalent results.
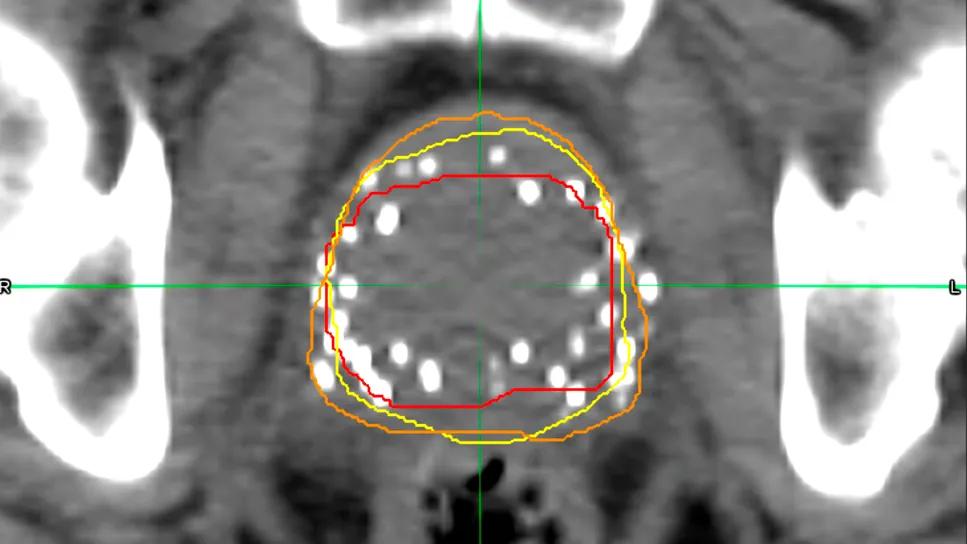
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3636bcab-0399-4fe2-ab59-11ca3e6f2f4a/ai-vs-physician-drawn-contours-after-prostate-brachytherapy)
CT scan after prostate brachytherapy
Although there are sizeable variations between AI- and human-generated contouring of CT scans after prostate brachytherapy, a recent study finds no notable differences in patient outcomes. The study data was presented at the 2025 annual meeting of the American Society for Radiation Oncology (ASTRO).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Auto-contouring software is a relatively new innovation that offers a potential alternative to time-consuming manual contouring of CT scans by physicians for post-implant quality assurance. However, these AI-generated contours don’t always match those drawn by physicians. Now a small study by Cleveland Clinic researchers shows that — despite discrepancies on the screen — patient outcomes between the two approaches are the same.
While it’s too early to rely on auto-contours without physician verification, researchers said the technology could serve as a helpful, time-saving starting point. The researchers found assessments of these tools should focus on patient outcomes, not just the contour lines themselves.
“When the measure of the adequacy of AI contours versus human contours is clinical outcome rather than subjective assessments of the contours (such as whether they look “pretty” or “right”), the best contour may not be what a practitioner may think,” explained senior author Jay Ciezki, MD, a radiation oncologist at Cleveland Clinic.
For the study, researchers compared two different auto-contouring systems against standard physician-drawn contours for 100 patients. In addition to comparing the contour outlines, they looked at patient outcomes, including biochemical failure, clinical failure, toxicities and survival.
Researchers found that there were significant variations between the different contouring methods. In one case, the auto-contouring software generated a median prostate volume of 65 ccs — more than double the volume drawn by physicians.
Advertisement
However, these large discrepancies didn’t seem to matter. Despite the variations in the contours themselves, the study found no significant difference in predicting clinical outcomes.
“When we looked at whether there was either a biochemical failure, meaning a rise in PSA down the line; or a clinical failure, in which there was a distant metastasis or the prostate cancer came back; or survival, there was no difference based on the different contours that were generated,” said first author Anirudh Bommireddy, MD, a radiation oncology resident at Cleveland Clinic.
One possible explanation for the findings is that, even with size variations, the clinically important part of the prostate was adequately covered by all three methods. .
“Ultimately, the larger prostate size on the scan or the way it’s drawn doesn’t necessarily mean we’re treating a different part of the prostate,” he says.
While the findings are encouraging, researchers said more data is needed to confidently support the use of auto-contouring software. They plan to expand the study to 300 patients to validate their initial findings.
“I think it’s still too small of a cohort to make any definitive conclusions, so expanding the sample size is the next step for us,” says Dr. Bommireddy.
Advertisement
Advertisement
Understanding supports for adolescent and young adult patients
Reframing cancer survivorship
New guidelines empower clinicians with practical diagnostic framework
Pivotal Studies Guide Treatment Decisions in Muscle-Invasive Bladder Cancer
Reflections from an oncology provider and communications educator on new ASCO Guidelines on Patient-Clinician Communication
Phase 1 trial outcomes offer encouraging news for developing targeted therapy for solid tumors
Cleveland Clinic to administer first-of-its-kind T-cell therapy
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy