Infectious disease and kidney transplant specialists share key insights
A new report from infectious disease and kidney transplant specialists at Cleveland Clinic suggests that otherwise healthy kidneys from deceased donors infected with SARS-CoV-2 are suitable for transplant.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The team is the first to report these early successes in kidney transplant from SARS-CoV-2 patients. They describe their experiences in the American Journal of Transplantation. At the time of publication, the team had completed 10 transplants from five donors. To date, that number has grown to over 40 transplants, and the physicians continue to observe good outcomes.
These findings upend conventional thinking that extrapulmonary organs from SARS-CoV-2-infected donors should be ineligible for donation because of the potential risk for virus transmission. In April 2020, a SARS-CoV-2 screening became mandatory for all potential organ donors. Any detectable virus essentially nulled eligibility for organ donation. While airway infection precludes the possibility of a lung transplant, whether or not extrapulmonary organs should be utilized has been more controversial.
The backdrop of this report is a persistent organ shortage. Nearly 4,000 kidney transplant candidates died on the waitlist in 2020 alongside the coronavirus pandemic. With this in mind, the team set out to examine the viability of kidney transplants from SARS-CoV-2 infected donors.
Alvin Wee, MD, MBA, Surgical Director, and Emilio Poggio, MD, Medical Director of the Kidney Transplant Program in Cleveland Clinic’s Glickman Urological & Kidney Institute, coauthors of the report, say the team’s goal was to put forth a strategy to utilize these otherwise healthy kidneys that had been declined by other transplant centers.
Advertisement
“None of the donors had clinical manifestations of COVID-19, either before or at the time of admission. None of their chest imaging revealed infiltrates emblematic of severe COVID infection,” he says. “And if there was any concern, the use of lower airway sampling with negative results provided reassurance.”
All 10 recipients consented to the organ from the SARS-CoV-2 infected donor and were counseled on the potential risk, albeit low, for transmission. There were no surgical complications, and at the time of follow-up (56-112 days), all transplanted kidneys were functioning well with no clinical evidence of virus transmission, either between donor and recipient or among organ procurement teams.
Aside from monitoring for COVID-19 symptoms and allograft function following the procedure, other potential monitoring strategies are not reasonable in a typical clinical setting, unless the patient becomes symptomatic. They do advise obtaining a nasopharynx COVID test and chest X-rays at baseline.
The Organ Procurement Transplant Network Disease Transmission Advisory Committee stresses the importance of balancing the potential risk of viral transmission with waitlist-related mortality.
Christine Koval, MD, Section Chief of Transplant Infectious Diseases at Cleveland Clinic, advised on the COVID-positive donor protocol . She says that there is no evidence linking transmission of SARS-CoV-2 by way of extrapulmonary transplant, but it’s still important to recognize theoretical risk and mitigate potential risk within reason.
Advertisement
“We can’t guarantee zero risks, but given what is currently known about viral transmission, it seems unlikely that a recipient would become infected or experience adverse outcomes via the extrapulmonary transplant.”
One strategy to mitigate risk, Dr. Koval suggests, is pairing extrapulmonary organs with recipients who have some form of immunological protection, like vaccination or prior infection, against the virus.
Though this paper reflects deceased donors whose causes of death were not linked to viral infection, the team has started to utilize well-functioning kidneys in more severe cases of COVID-19. These findings are not yet published. The team says they continue to be conservative in their selection and management process and will evolve their practice as they learn more.
“These are cases of balancing minimal risk with overall benefit,” says Dr. Wee. “This is always part of the process when a patient weighs the risk-benefit ratio of accepting an organ versus remaining on the waitlist. Yes, the pandemic has further complicated this process, but we are heartened that we help find meaning in this senseless death.”
Advertisement
Advertisement

Milestone minimally invasive surgeries reduce pain and recovery time

Enhanced visualization and dexterity enable safer, more precise procedures and lead to better patient outcomes

Insights on bringing Cleveland Clinic even closer to becoming the best transplant enterprise in the world

Minimally invasive approach, peri- and postoperative protocols reduce risk and recovery time for these rare, magnanimous two-time donors

Minimally invasive pancreas-kidney replacement reduces patient’s pain, expedites recovery

First-ever procedure restores patient’s health
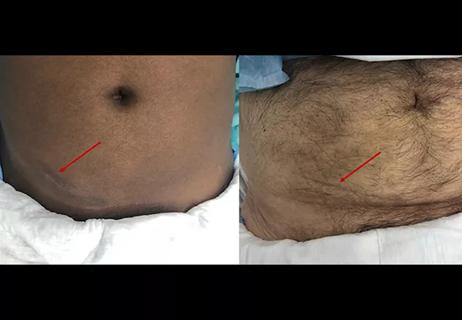
Smaller incision may lead to reduced postoperative pain for some patients
Improving access to lifesaving kidney transplant