Study identifies factors that improve preoperative detection and procedures
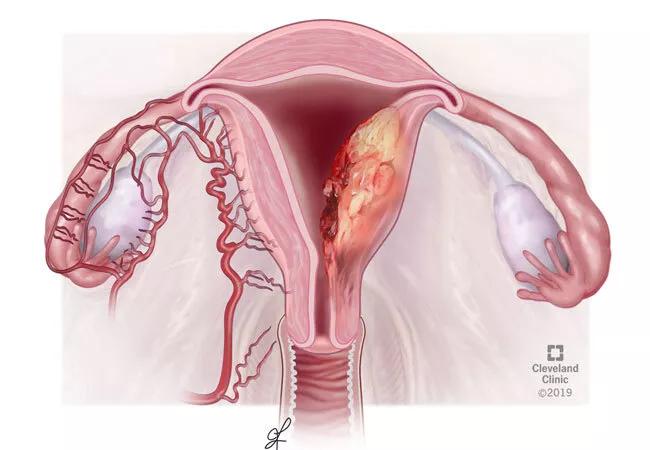
A recent study of the effectiveness of endometrial sampling in detecting leiomyosarcoma (LMS), an aggressive uterine cancer with a poor prognosis, indicates that when sampling is done in conjunction with hysteroscopy before hysterectomy, there is a threefold increase in pre-operative diagnosis.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Rosanne M. Kho, MD, of Cleveland Clinic’s Women’s Health Institute, was lead author on the research published in the Journal of Minimally Invasive Gynecology.
Symptoms of leiomyosarcoma often mimic uterine leiomyomas, which can include abnormal bleeding, pelvic pain and infertility. While LMS is rare, occurring in only 13 out of 10,000 surgeries for presumed leiomyomas, the prognosis for LMS patients is poor. The five-year survival rate for disease diagnosed at stage I is 55.4%; at stage IV it is 13.1%.
Pre-surgical diagnosis is notably difficult. Postmenopausal and Black women are at higher risk, as are those with a history of pelvic radiation, extended use of tamoxifen, and those who present with a single, rapidly increasing tumor with atypical features. No diagnostic test exists to reliably differentiate LMS tumors from a benign fibroid.
“We are continually trying to find ways to catch these patients before we go in with surgery,” Dr. Kho says. “First of all, in many situations of leiomyosarcoma, surgery should not be the first approach. Secondly, if surgery is to be performed, you need to be ready with the right team. It has to be in the hands of the oncologists.”
The researchers examined linked data from the New York Statewide Planning and Research Cooperative System and the New York State Cancer Registry from 2003 to 2015. The study subjects were women with uterine leiomyosarcoma who had undergone endometrial sampling within 90 days before a hysterectomy. Among 79 cases that met the sampling criteria, 46 received a preoperative diagnosis of LMS and 33 had been diagnosed post-operatively.
Advertisement
Leiomyosarcoma was picked up by endometrial sampling about 58% of the time.
“Historically, it was thought that these cancers were contained only within the myometrium, and that therefore an endometrial sampling would be not very helpful, because you’re not actually sampling the tumor itself,” says Dr. Kho. “To find that 58% of the time the result is positive suggests that it’s worthwhile.”
In addition, the study found that the detection rate tripled for cases in which hysteroscopy was used during sampling procedures — pipelle biopsy or dilation and curettage.
“The assumption is that when you use hysteroscopy, you can better direct where to sample,” Dr. Kho says. “Hysteroscopy at the time of sampling should be the gold standard. It has been declared as a gold standard for over 10 years, yet it still is not routinely done. There’s a role for preoperative sampling, and if preoperative sampling is to be done, consider using hysteroscopy and not perform a blind sampling alone.”
The researchers also found that in some women whose diagnosis of LMS was not detected before surgery, the chosen procedure was supracervical hysterectomy. “We know that you don’t do that in cancer surgery,” Dr. Kho says.
In general, she adds, the advantages of supracervical hysterectomy have been shown to be minimal.
“There is strong evidence from the Cochrane Review that it really does not confer any advantage other than the fact that you do not subject the patient to a vaginal cuff dehiscence,” says Dr. Kho. “There are no benefits in terms of bladder, bowel or sexual function in leaving the cervix behind. It used to be thought that if you leave the cervix behind, there’s better sexual function or there is less risk of a prolapse or fewer complications, but that did not bear out as true.”
Advertisement
The endometrial sampling study did not find that the prognosis or the survival rate was worse in women whose diagnosis were missed. Dr. Kho attributes that to possibly the limited sample size in the retrospective research. A prospective study that gathers data from medical centers across the country will be needed, she says.
Advertisement
Advertisement

Uterine transposition cleared the field for radiation therapy

ACOG-informed guidance considers mothers and babies

Prolapse surgery need not automatically mean hysterectomy

Artesunate ointment shows promise as a non-surgical alternative

New guidelines update recommendations

Two blood tests improve risk in assessment after ovarian ultrasound

Recent research underscores association between BV and sexual activity

Psychological care can be a crucial component of medical treatment