By Toby Cosgrove
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
President and CEO, Cleveland Clinic
For each of us, our face is our calling card to the world. It helps define our personal identity and allows us to communicate, both verbally and non-verbally, whether through a smile, a scowl or a quizzical furrowed brow.
But the face is also much more than that. It supports multiple functions and senses – seeing, breathing, smelling, tasting, and speaking. These are things we all take for granted, but for those who have suffered traumatic injury or disease, facial disfigurement can be debilitating. Plastic surgery and reconstruction can help in some cases, but it’s often not enough to improve their function or allow them to feel welcome in public.
For some of these people, a face transplant may be the only option.
In December 2008, Cleveland Clinic became the first U.S. hospital to perform a face transplant. At the time, it was considered the largest and most complex face transplant in the world.
In late September, we performed our second face transplant, which was even larger and more complex than the first. Nine surgeons operated for 24.5 hours to replace about 90 percent of the facial tissue on a middle-aged man who suffered severe facial trauma and other complications from a car accident.
The surgery is a marvel of modern medicine. Unlike an organ transplant, which is transplanting just one type of tissue, a face transplant integrates skin, muscle, bony structures, arteries, veins and nerves. In the most recent case – which is supported by the U.S. Department of Defense’s Armed Forces Institute of Regenerative Medicine (AFIRM) program – surgeons transplanted about two-thirds of the patient’s scalp, his forehead, upper and lower eyelids, eye sockets, nose, upper cheeks, upper jaw, upper teeth, facial nerves, salivary glands, facial muscles, and skin.
Advertisement
A face transplant is still considered an experimental procedure. After all, fewer than three dozen face transplants have been performed worldwide.
Successfully completing such a feat requires an institution that supports innovation and encourages its physicians and scientists to push the boundaries in order to serve patients’ needs. It requires years of research and cadaveric practice. It requires skilled surgeons and staff.
Mostly, though, it requires a brave patient and a selfless family that’s willing to donate a loved one’s facial tissue.
Without a doubt, these are difficult decisions. On the patient’s part, they have to ask themselves whether the surgery is worth the risk. On the donor family’s part, they have to wrestle with the notion of donating the most identifiable aspect of their loved one.
It’s important that people understand that the donation of facial tissue is radically different from organ donation. With organ donation, people can decide for themselves whether they want to be a donor, then express their wishes on their driver’s license. Facial tissue is different; donating facial tissue requires a special request of the deceased’s family. (For both of our face transplant surgeries, Lifebanc, Northeast Ohio’s nonprofit organ and tissue recovery organization, discreetly approached the donor families.)
It’s also important that people understand that a face transplant is not just an aesthetic procedure. The significance of the face cannot be under-estimated. In addition to reflecting our personality, vitality, and distinctiveness, the face sustains us, giving us eyes to see, a nose to smell and breathe, a mouth to eat, speak and breathe, and a canvas that conveys richness and complexity of our every emotion.
Advertisement
In those with severe facial disfigurement, the restoration of such complex functions is beyond the bounds of plastic surgery and reconstruction; both of our patients endured dozens of attempts at facial reconstruction, without any measurable improvement in their functioning or quality of life.
After her surgery in 2008, Connie Culp could once again eat solid food, drink from a cup, breathe without a tracheostomy, and kiss her grandson. Our most recent patient is recovering well. He is now breathing without a tracheostomy and will begin eating orally shortly. In the coming months and years, the improvements should only continue to proliferate, until he can once again enjoy the elements of life that the rest of us often take for granted.
Advertisement
Advertisement

Milestone minimally invasive surgeries reduce pain and recovery time

Enhanced visualization and dexterity enable safer, more precise procedures and lead to better patient outcomes

Insights on bringing Cleveland Clinic even closer to becoming the best transplant enterprise in the world

Minimally invasive approach, peri- and postoperative protocols reduce risk and recovery time for these rare, magnanimous two-time donors

Minimally invasive pancreas-kidney replacement reduces patient’s pain, expedites recovery

First-ever procedure restores patient’s health
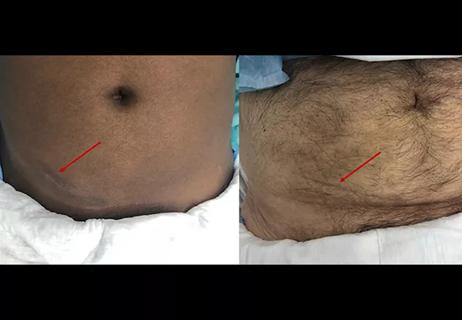
Smaller incision may lead to reduced postoperative pain for some patients
Improving access to lifesaving kidney transplant