Some patients exhibit marked nodulosis due to undiagnosed tophi
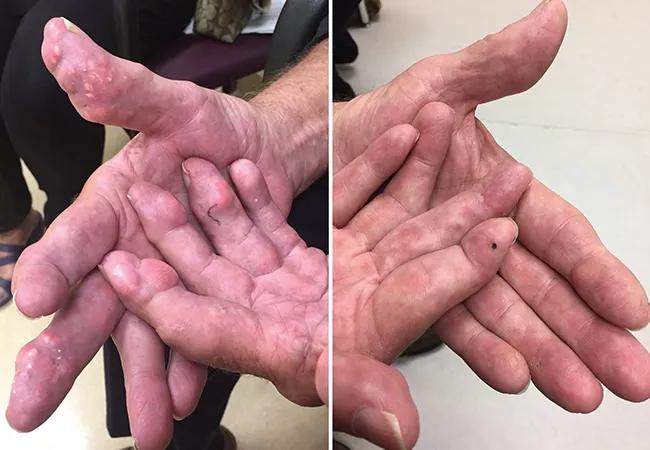
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8b30ddea-1313-408b-8772-2468498209f0/23-RHE-4186164-CQD-650x450-1_jpg)
gout
This article is republished from the Cleveland Clinic Journal of Medicine, June 01, 2023; Volume 90, Issue 6.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Gout is clinically defined by recurrent, dramatic, self-limited flares of inflammatory arthritis, bursitis, or tendonitis. Flares are the cardinal symptom of the gouty disease process, the deposition of uric acid in the soft tissues with a predilection to periarticular structures. The location of initial flares and uric acid deposits (tophi) is frequently in the extremities. This is attributed to the cooler temperatures in the hands and feet facilitating the deposition of uric acid in patients who have biologic hyperuricemia, defined as a serum urate level above its approximate saturation level of 6.8 mg/dL. However, some patients exhibit tophi detected on physical examination or deeper tophi detected by advanced imaging such as ultrasonography or dual-energy computed tomography in the absence of typical clinical flares or pain.
Uric acid deposition can be seen using dual-energy computed tomography or ultrasonography before the occurrence of flares. Deep-tissue periarticular and intra-articular tophi are usually clinically unrecognized until they are associated with a painful flare. Tophi in more superficial areas such as the ears, olecranon bursae, and skin may be noticed as asymptomatic nodules, often in patients who have experienced flares elsewhere. Some patients exhibit marked nodulosis due to undiagnosed tophi in the absence of typical gouty flares and thus may be undiagnosed as having gout and not treated. Two such patients are described below.
Advertisement
A 46-year-old male was referred to Rheumatology for evaluation of hand stiffness. He had no history of acute painful flares. He had chronic kidney disease of unclear etiology, with a serum creatinine level 2.4 mg/dL (reference range 0.74–1.35) and a serum urate 8.6 mg/dL (4.0–8.5). He had been told of osteoarthritis and possible gout but had never sought treatment.
The patient had tophi overlying the proximal interphalangeal (PIP) and distal interphalangeal (DIP) finger joints. While this presentation is often seen in postmenopausal women with osteoarthritic Heberden and Bouchard nodes and with tophi that may become acutely inflamed,1 tophacious deposition around the DIP and PIP joints is not limited to that demographic group and may be mischaracterized as inflammatory osteoarthritis.
On full examination, the patient also had a nodule on the helix of his left ear and small nodules palpable in the olecranon area bilaterally. The physical appearance, firm feel on palpation, and location of these asymptomatic nodules in conjunction with the significant hyperuricemia and chronic kidney disease supported the clinical diagnosis of gout. He did not have significant hyperlipidemia.
Treatment
Due to the periarticular location of the significant tophacious deposits, with resultant hand stiffness and difficulty in fully flexing the fingers, the suggested treatment regimen was aggressive urate-lowering therapy aiming for a very low serum urate level (< 3 mg/dL), which would be expected to accomplish relatively rapid dissolution of the deposits. Depending on the patient’s response to medication, this serum urate level might be attained using a dose-adjusted xanthine oxidase inhibitor with or without probenecid or pegloticase, followed by a xanthine oxidase inhibitor once significant tophi were dissolved and hand function normalized.
Advertisement
The patient was cautioned that rapid and intense lowering of the serum urate was likely to precipitate gout flares until the uric acid deposits had dissolved, and he was advised to have a plan in place to prevent flares and treat them if they should occur. As the patient lived very far from the clinic, treatment was anticipated to be provided closer to his home.
A 70-year-old male presented with dermal and soft-tissue nodules in the hands (above left)2 with no history of gout flares. He had been diagnosed with gout and previously had documented serum urate levels between 7.2 and 8 mg/dL, with a normal serum creatinine.
Experiencing minimal symptoms, he had never received urate-lowering therapy. He was otherwise healthy without any kidney, vascular, or metabolic disease. He described increasing hand stiffness causing difficulties in his avocational use of power tools and in driving industrial machinery. Interestingly, a large, hard mass adjacent to his right lateral malleolus led to him frequently being stopped and examined as he went through airport security screening procedures.
Treatment
He was prescribed aggressive urate-lowering therapy utilizing uricase-replacement therapy with pegloticase, and with serial testing of serum urate levels. After six months of therapy, with serum urate levels maintained below 0.2 mg/dL, there was dramatic resolution of his hand nodules (above right). After an additional six months of treatment, the malleolar tophus also regressed, allowing the patient to travel unimpeded through airport security screening. Pegloticase therapy was followed by treatment with allopurinol to maintain a serum urate of approximately 5.5 mg/dL.
Advertisement
Chronic subcutaneous nodules can be found associated with a number of disorders, including rheumatoid arthritis, dyslipidemia, sarcoidosis, multicentric histiocytosis (periungual nodules), lipoma, systemic lupus erythematosus, dermatofibroma, calcinosis, metastatic carcinoma, and leukemia or lymphoma. However, only gouty tophi are likely to present in the anatomic locations with the appearance shown in these scenarios—especially in the absence of other systemic or laboratory features associated with an alternative underlying disorder.
When the skin is pulled taut, there is a pearlescent yellow-white appearance to these firm, nontender nodules. If there is clinical uncertainty, or if the response to urate-lowering therapy is not as anticipated, needle aspiration of a nodule will reveal the presence of chalky material composed of monosodium urate crystals when viewed under polarized microscopy. Aspiration can be done with a 20- or 18-gauge needle by penetrating the nodule and twisting the needle, then wiping the bevel of the needle on a clean slide. Tophi, particularly if traumatized or repeatedly stretched due to location over a joint, may spontaneously perforate, drain uric acid crystal-containing material, and in rare cases, become infected.
Advertisement
Advertisement
Unraveling the TNFA receptor 2/dendritic cell axis
Nasal bridge inflammation, ear swelling and neck stiffness narrow the differential diagnosis
Genetic testing at Cleveland Clinic provided patient with an updated diagnosis
From dryness to diagnosis
Multiple comorbidities are associated with pediatric psoriasis
Untreated seropositive erosive RA led to peripheral ulcerative keratitis
New clinic meets Hispanic patients where they are
Treatment strategies require understanding of pathomechanisms