A better outlook
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Primary angiitis of the central nervous system (PACNS) remains one of the most complex forms of vascular inflammatory disease. Multiple factors contribute to our relatively limited understanding of the disease including its rarity, the lack of an efficient noninvasive test, a paucity of pathological material to study and the absence of animal models simulating the disease.
Cleveland Clinic has been a leader in care and research in the field of central nervous system (CNS) vasculitis for more than 25 years, developing criteria for its diagnosis that are widely employed today. We have recently begun to report on long-term outcomes of these patients to better understand this rare disease.
Historically, patients with PACNS vasculitis were diagnosed postmortem. The first report by Cupps et al. describing sustained clinical remission in four patients in 1983 brought more enthusiasm to the possibility of treating this disease. Since then, clinicians have elucidated much of the clinical manifestations of and diagnostic approach toward this disease, but little is known about the overall outcomes of these patients. Recent cohort studies have described a generally favorable disease course.
Although most of what we know about this very rare disease is from these large cohorts, there remains no consistency in the studies’ diagnostic approaches, where less than half of the patients had brain biopsies. Therefore, the outcomes depicted may not be generalized.
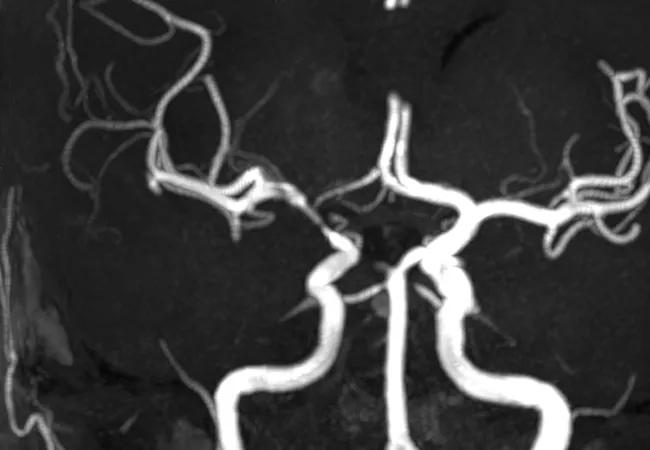
In addition, more recent advances have discerned the importance of ruling out reversible cerebral vasoconstriction syndrome (RCVS), a major angiographic mimic of PACNS. The definition of RCVS as an entity in 2007 is considered a major breakthrough in understanding and eliminating the mimics of PACNS. Prior to 2007, RCVS was not well characterized, which may have added to the contamination of some of the PACNS cohort.
Advertisement
We have recently elucidated functional capabilities, quality of life and frequency of depression for our strong cohort of patients with PACNS. We have only included in this cohort patients whose diagnosis was established by brain biopsy (74.1 percent) or by the presence of both abnormal cerebral angiography and cerebrospinal fluid findings (25.9 percent).
We mailed four questionnaires to patients to assess their disability scores (Barthel Index), quality of life (EQ-5D), and depression (PHQ-9). Modified Rankin Scale, a disability assessment, was obtained during the last visit.
Of 78 patients, 27 responded to the questionnaires (34.6 percent). Mean follow-up was 5.5 years (± 4.7). Seventy percent had mild disability, and 5 percent had severe disability. Around half of the patients had no mobility problem and no problems with usual activities, and two-thirds had no problems with self-care. Physician assessment with the Modified Rankin Scale showed that the majority of PACNS patients had mild long-term disability with a median disability score of one. Approximately 70 percent of patients had minimal or no depression. Mortality was 11 percent.
This is the longest reported follow-up of patients with PACNS in the literature to date and the first evaluation of the quality of life and incidence of depression in these patients. Most of the patients had mild long-term disability and no difficulty with walking, usual activities and self-care, which may be reflective of improved management of this disease or earlier diagnosis and recognition. Rates of depression and mortality represent opportunities for improved diagnosis and treatment of patients with PACNS.
Advertisement
Dr. Hajj-Ali is Associate Director of the Center for Vasculitis Care and Research.
Advertisement
Advertisement

The case for continued vigilance, counseling and antivirals

High fevers, diffuse rashes pointed to an unexpected diagnosis

No-cost learning and CME credit are part of this webcast series

Summit broadens understanding of new therapies and disease management

Program empowers users with PsA to take charge of their mental well being

Nitric oxide plays a key role in vascular physiology

CAR T-cell therapy may offer reason for optimism that those with SLE can experience improvement in quality of life.

Unraveling the TNFA receptor 2/dendritic cell axis