Two studies from Cleveland Clinic may help advance the technology toward broader clinical use
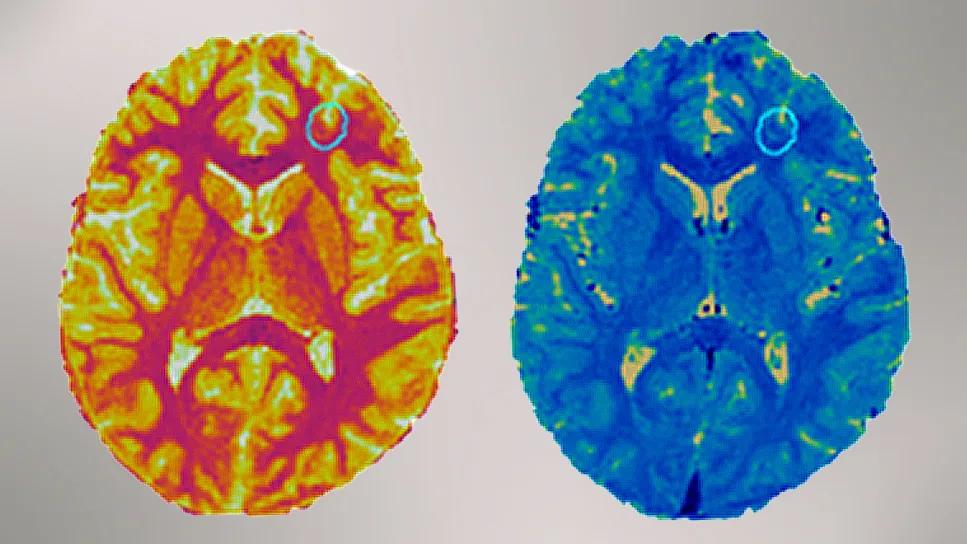
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/a24b00dd-4de5-482e-8107-5614465249f7/two-brain-scans-dr-wang-epilepsy)
two brightly colored brain scans side by side
For clinicians managing medically refractory focal epilepsy, a leading challenge frequently lies in what have been termed “nonlesional” brain MRI scans. Subtle focal cortical dysplasia (FCD) often eludes visual assessment on standard MRI, resulting in forgone or deferred epilepsy surgeries or unsuccessful surgical outcomes.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Two recent Cleveland Clinic studies demonstrate that magnetic resonance fingerprinting (MRF) — a rapid, quantitative imaging technique — can significantly improve the ability to detect the elusive lesions of FCD and determine which ones are actively driving a patient’s seizures.
The studies collectively signal progress in defining optimal clinical applicability of MRF when traditional MRI comes up short in epilepsy imaging. “We have shown that, by integrating MRF with machine learning and surface-based analysis, clinicians can now achieve high detection sensitivities for subtle FCD while simultaneously reducing the noise of false positives,” says the studies’ senior author, Irene Wang, PhD, Research Director, Cleveland Clinic Epilepsy Center. “We also found that in complex cases involving multiple malformations, MRF offers a noninvasive method for prioritizing which lesions require invasive electroencephalography (SEEG) exploration.”
The first study (Epilepsia. 2025 Epub 9 Oct), led by Dr. Wang and Ting-Yu Su, PhD, a postdoctoral fellow in her lab, focused on developing a robust framework for whole-brain FCD detection by combining MRF with machine learning and surface-based morphometry, a widely adopted MRI postprocessing technique.
“Manual identification of FCD is highly variable and depends on specialized clinical expertise,” Dr. Su explains. “Subtle imaging features are easily missed. We sought to create an automated pipeline that leverages the high-resolution, quantitative data of MRF to improve upon existing surface-based detection methods.”
Advertisement
The team retrospectively analyzed 44 patients with confirmed FCD who underwent an MRF research scan at Cleveland Clinic. They also recruited 70 age- and gender-matched healthy individuals to undergo MRF scanning to serve as a control group.
All MRF imaging was performed using a high-resolution 3T MRF sequence (approximately 10 minutes scan time) to generate T1 and T2 maps. These maps were integrated with structural T1-weighted and 3D FLAIR images collected clinically. Quantitative features were generated based on all these data.
For FCD detection the researchers employed a two-stage machine learning approach using the following:
Key findings included the following:
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d6259df8-1610-474f-b0bb-c789d6b2d346/brain-scan-images-dr-wang-inset-1)
Figure 1. Example images from patients in whom the MRF machine learning models identified clusters (yellow) that had excellent overlap with the manual lesion labels (red) in cases where the clinical MRI was positive (left) and negative (right). LEFT: Patient with FCD IIb in the right mesial occipital lobe. RIGHT: Patient with mild malformation of cortical development (mMCD) in the left basal temporal region.
“This research is the first to integrate surface-based morphometry with MRF-generated quantitative tissue property maps,” Dr. Wang notes. “It establishes that MRF-driven machine learning frameworks can match or exceed expert human performance in lesion detection. For clinicians, the framework’s prediction probabilities may potentially serve as a confidence index in distinguishing true lesions from anatomical variants or imaging artifacts.”
The second study (J Neurol Sci. 2025;477:12351) addressed a different clinical dilemma: In a patient with multiple cortical malformations, which one is the source of the seizures?
Multiple FCD-like abnormalities or widespread polymicrogyria (PMG) are present in a single patient, but these lesions are not always equally epileptogenic. Determining which lesion(s) to target often requires invasive stereoelectroencephalography (SEEG). This pilot study investigated whether MRF could noninvasively indicate the active seizure onset zone in this setting.
Dr. Wang and colleagues retrospectively analyzed 69 individuals who underwent a 3D whole-brain MRF research scan at Cleveland Clinic. This included 21 patients with refractory focal epilepsy and 48 healthy controls included for comparative analysis. Of the patients, four had complex cortical malformations (FCD or PMG) for which they underwent SEEG and/or surgery and 17 had histopathologically verified FCD II.
Among the four complex cases, the researchers compared MRF signatures within the same patient (comparing active vs. silent lesions) and across patients (comparing lesions with those in the 17 patients with FCD II).
Advertisement
Key results included the following:

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f1f7e0f6-09fb-4a38-8bba-bbf90cac9600/brain-scan-images-dr-wang-inset-2)
Figure 2. Example patients in whom the MRF T1 shows significant differences in the seizure-causing lesion compared with the electrically “silent” lesion. Knowing this information before surgery could help design better implantation/surgical plans. Reprinted from Kochi et al., J Neurol Sci. 2025;477:12351, ©2025 The Authors, under the CC BY-NC license.
Dr. Wang and co-authors conclude that quantitative gray matter T1 as measured by MRF could serve as a sensitive marker for epileptogenicity. “MRF shows promise as a noninvasive imaging probe for in vivo epileptogenicity,” Dr. Wang says. “What we need to understand more is which quantitative metrics consistently and strongly correlate with epileptogenic tissue. If our pilot findings are confirmed in larger studies, MRF will have a role in guiding SEEG implantation and surgical planning in complex cases, including those with multiple cortical malformations.”
According to the Cleveland Clinic Epilepsy Center researchers, these two studies collectively offer several insights for the management of intractable epilepsy:
Advertisement
“As MRF moves toward broader multicenter validation, the fact that it can now be acquired in just a few minutes makes it increasingly practical for routine use,” Dr. Wang concludes. “It has the potential to become an important part of presurgical evaluation and surgical planning for patients with refractory focal epilepsy.”
Advertisement
Researchers pair quantitative imaging with AI to improve surgical outcomes in nonlesional epilepsy
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Early identification of temporal encephaloceles can improve surgical decision-making
Insights from one of the first studies of invasive monitoring in the rare form of focal cortical dysplasia
Overcoming barriers to implementing clinical trials
Comorbidities and medical complexity underlie far more deaths than SUDEP does
Novel Cleveland Clinic project is fueled by a $1 million NIH grant
Paired blood and brain tissue methylation findings raise prospect of noninvasive precision diagnosis