Addressing unmet needs in acute injury, neuropathy, nerve tumors and more
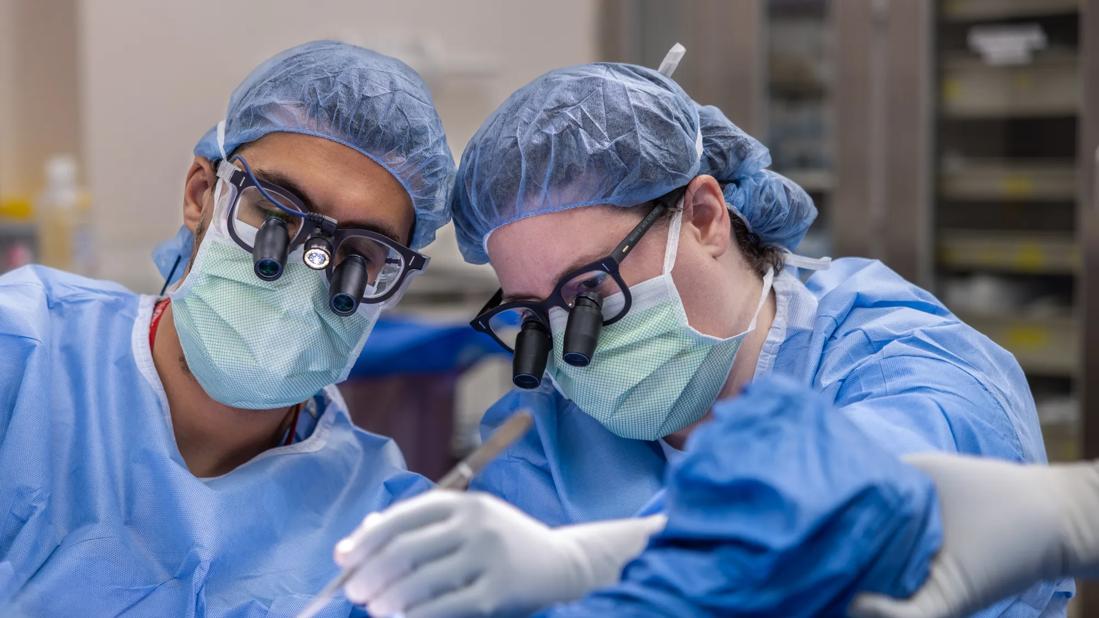
Peripheral nerve neurosurgeons are relatively few and far between, but they offer singular capabilities for improving function and minimizing pain and disability for individuals with acute nerve injuries, entrapment neuropathies, benign nerve tumors and other nerve disorders.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Megan Jack, MD, PhD, is a peripheral nerve neurosurgeon who recently joined Cleveland Clinic’s Neurological Institute. She sat down with Consult QD to explain some specifics of how her little-understood subspecialty can help patients with nerve injury and their referring providers.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3e5a2b04-e3e9-43ff-8993-170569c9b503/21-NEU-2344333-peripheral-nerve-neurosurgery-650x450-1-jpg)
A: Patients with issues in any of the three functional domains of nerves — motor, sensory or pain — can be good candidates for referral. We often see patients who have profound weakness, frequently due to nerve injury, and those with severe sensory changes or pain, often due to tumors or compressive neuropathies.
A: Nerves take a long time to regrow — typically at a rate of about a millimeter a day or an inch per month. So for a nerve that extends through an entire extremity, that represents a years-long process. The challenge is that as a nerve is regrowing, the muscle that is no longer innervated by the injured nerve goes through a dying process. The aim is to reinnervate the muscle before too much muscle loss takes place.
For this reason, referral to a peripheral nerve neurosurgeon is best done early, within three months of the nerve injury. We like to follow our patients with serial imaging and serial diagnostics to determine whether there is some level of recovery of muscle function and the nerve regeneration process.
A: When a patient is referred, I do a thorough neurological examination so I can follow their progression to determine whether they are recovering on their own. If they show no signs of either functional recovery or electrodiagnostic recovery on electromyography or nerve conduction studies by about six months after injury, we will discuss surgical options to try to restore some function. Those include primary repair of a nerve, grafting, or nerve transfer to achieve reinnervation of the muscle to improve functional outcome.
Advertisement
A: Some nerves do better with repair than others, for reasons we don’t yet fully understand. For instance, obtaining recovery from injury to the ulnar nerve can be very challenging, whether it be natural recovery or achieving results from surgical repair. In the lower extremity, the peroneal nerve is more sensitive to injury, which also tends to be harder to recover from. For the most part, however, any nerve in the body can at least be evaluated for surgical repair, and there usually is an option for repair of most nerves.
A: About 75% of my surgeries are outpatient procedures. These operations range from straightforward procedures that take an hour or less to complex brachial plexus reconstructions, which can last eight hours and may require a three-day postoperative hospital stay if a free muscle flap is required. So there is a wide range of complexity.
A: The degree of functional recovery depends on many factors, including patient age, how soon surgery is done and how extensive the nerve injury was. So there is definitely variation. But if intervention is timely, patients usually gain better functional outcomes than what they would achieve on their own. Some achieve a near-full recovery of their pre-injury muscle strength and function along with good range-of-motion restoration.
A: Our subspecialty has focused mostly on motor function, but we’re increasingly learning that sensation is important to patients too, and progress is being made on that front. For instance, patients who need brachial plexus reconstructions also have impaired sensation, and we are able to connect more sensory nerves to allow improved function from that perspective as well. So sensory function has been an overlooked area, but more is starting to be done, particularly in spinal cord injury, which often prevents sensation in ways that can lead to complications such as pressure ulcers.
Advertisement
A: The benign tumors I see most often are schwannomas and neurofibromas, which sometimes accompany cutaneous syndromes such as neurofibromatosis type 1. These tumors can develop on any nerve in the body, from small sensory cutaneous nerves to a complex and important nerve like the ulnar nerve that controls a lot of hand function. So the surgeries to remove them can range from 30 minutes to two or three hours.
I also have particular interest in perineural tumor spread, in which tumor can travel along the small nerves that innervate a cancer-affected organ, such as the prostate, and spread to larger nerves, such as the sciatic nerve. In these cases, which are pretty rare, I can help recognize the phenomenon and do a biopsy to determine the type of cancer affecting the nerve. Similarly, there are lymphoma cases in which tumor can be found in a peripheral nerve and the only presenting symptom is pain or weakness; in these cases I can do a fascicular nerve biopsy and confirm the lymphoma diagnosis.
A: Peripheral nerve neurosurgeons see a wide spectrum of nerve disorders, and we are finding new and innovative ways to treat patients every day. One of the interesting and very rare surgeries we offer is for patients with cervical dystonia, or torticollis. We can do denervation procedures to improve these patients’ head alignment and allow them to keep their head straight.
While this might not seem like a particularly important surgery, it can dramatically improve patients’ quality of life. Torticollis can be a devastating disease, in terms of both pain and social ramifications. Allowing these patients to keep their head up allows them to see the world differently — and allows the world see them differently. That can make a tremendous difference, so it’s very gratifying.
Advertisement
Advertisement

Aim is for use with clinician oversight to make screening safer and more efficient

Rapid innovation is shaping the deep brain stimulation landscape

Study shows short-term behavioral training can yield objective and subjective gains

How we’re efficiently educating patients and care partners about treatment goals, logistics, risks and benefits

An expert’s take on evolving challenges, treatments and responsibilities through early adulthood

Comorbidities and medical complexity underlie far more deaths than SUDEP does

Novel Cleveland Clinic project is fueled by a $1 million NIH grant

Tool helps patients understand when to ask for help