Disease associated with higher risks for maternal and fetal morbidities
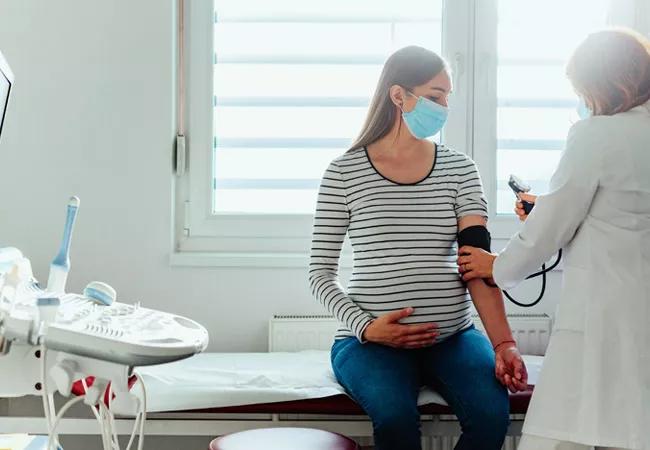
Physicians who care for women of child-bearing age and have systemic lupus erythematosus (SLE) should ask them one crucial question: Do you plan to become pregnant? The answer can make the difference between a smooth perinatal experience and one beset by complications.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
While most pregnancies for patients with lupus have positive outcomes, SLE is associated with significantly higher risks for complications, including preeclampsia, gestational diabetes, and delivering a baby with neonatal lupus. In addition, a recent cross-sectional study using data from the National Inpatient Sample concluded that lupus was an independent risk factor for increased cardiovascular complications at the time of delivery.
These are among reasons Cleveland Clinic specialists say family planning conversations with SLE patients should take place as early as possible. The sooner that patients understand the importance of management efforts, the more empowered they are to set the stage for a successful experience, say Cara Dolin, MD, MPH, maternal-fetal medicine specialist in the Ob/Gyn & Women’s Health Institute, and Emily Littlejohn, DO, MPH, a physician in Cleveland Clinic’s Department of Rheumatologic and Immunologic Disease.
SLE raises risks for a number of serious maternal complications: thromboembolism, high blood pressure, stroke, and acute kidney injury. Preeclampsia is among Dr. Dolin’s top concerns.
“We worry about preeclampsia with all pregnant women, but the risk is much higher with lupus, especially if the patient has underlying hypertension, kidney disease or other underlying comorbidities,” Dr. Dolin says.
The November 2022 study on cardiovascular complications for pregnant women with SLE aimed in part to isolate factors contributing to the recent, steady increase in maternal morbidity rates in the United States. Results from its focus on time-of-delivery complications dovetail with other concerning health trends, says Dr. Dolin.
Advertisement
“It mirrors the increase in maternal morbidity and mortality that we’re seeing across the board,” she says. “Part of that is more people are going into pregnancy less healthy, whether because of obesity, older age, chronic hypertension, diabetes overlaying their lupus — any number of factors. And these conditions increase cardiovascular events.”
By ensuring effective management of pregnancies in patients with lupus, related fetal risks — including neonatal lupus, premature birth, miscarriage and still birth — also can be reduced.
Fetal growth restriction is a condition more common in patients with than without autoimmune disease. The condition can have multiple causes related to maternal health, and it can significantly affect outcomes, says Dr. Dolin. “Underlying vasculopathy due to lupus, or chronic hypertension, can affect the development of the placenta and how efficiently it functions to bring blood, oxygen and nutrients to the baby. A dysfunctional placenta can lead to fetal growth restriction, preeclampsia, and sometimes a need for a preterm birth,” she adds.
Dr. Littlejohn strives to always ask patients within child-bearing age whether they plan to conceive or begin pregnancy planning within the next year.
“It’s really important because there are elements of care that have to align for them to safely conceive,” she says. “The first is that we need to make sure that their medicines are safe for pregnancy, that they’re not having any side effects on these medications, and that their disease is well controlled on them. We have to switch from medicines that are not safe for pregnancy to those that are. And then we want to make sure their disease is controlled for three to six months before they conceive. Studies show patients who have well-controlled lupus going into pregnancy and during pregnancy will have better outcomes.
Advertisement
“Patients who go into the pregnancy with their lupus well controlled on safe medications have the highest odds of safe and healthy pregnancy outcomes,” says Dr. Littlejohn.
Instances in which no planning has taken place can yield some of the most difficult scenarios, says Dr. Littlejohn.
“Certain lupus medication are so teratogenic that patients are required to sign a Risk Evaluation and Mitigation Strategy (REMS) form that ensures patients are going to use two types of birth control while taking them,” she says. “They can cause fetal malformations and other birth defects.”
Patients also need to know when it’s important to keep taking their medication, adds Dr. Dolin.
“We run into trouble if patients haven’t seen us for a preconception consult, then become pregnant and suddenly think they have to stop all medications because of the pregnancy,” she says. “This can lead to disease flares, which can complicate both their health and the health of their developing baby.”
Dr. Littlejohn notes that certain medications should absolutely be continued.
“Hydroxychloroquine, or Plaquenil, for instance, is safe for pregnancy,” she says. “It takes a long time to work, and it’s one of the medicines that we know is associated with better birth outcomes in patients who continue to take it through pregnancy”
Resources provided by HOP-STEP, an education program designed to help providers improve pregnancy management for women with lupus, can help both providers and patients, says Dr. Littlejohn. Materials include a list of medications commonly used for SLE that are compatible with pregnancy; a “stop” list of drugs that may cause birth defects; and identifies two — rituximab and belimumab — for which insufficient information is available.
Advertisement
“The recommendations are relatively straightforward, with some drugs being absolutely suitable for pregnancy and others absolutely not suitable,” says Dr. Littlejohn. “There are some drugs that we can give in different trimesters, but overall, you don’t want to be changing things during the pregnancy. Ideally, the treatment plan is set before the patient even conceives. We do have some options if someone has a flare during pregnancy, but it’s not ideal.”
Pregnant women with lupus should be seen more frequently than those without underlying conditions.
“Part of these frequent visits is the opportunity to check their blood pressure and look for protein in the urine, to screen for preeclampsia,” says Dr. Dolin. “We also perform serial fetal growth assessments throughout the third trimester to make sure that the baby’s growing appropriately. In the last few weeks of pregnancy, we perform twice-a-week antepartum testing, because that’s really the highest risk time for there to be a complication.”
One of the insights offered by the JAMA paper on increased cardiovascular complications is the importance of close postpartum follow-up, she adds. “Many of these cardiovascular events don’t necessarily happen during delivery hospitalization, but in the weeks that follow.’
Peripartum cardiomyopathy, one of the most serious complications, can show up as many as 30 days after delivery. Patients are at elevated stroke risk up to six weeks postpartum. Those who have antiphospholipid antibodies (lupus anticoagulant syndrome) are predisposed to blood clots and strokes. Social drivers of health can exacerbate all risks for this patient population. In Ohio, a 2022 regulation change extended Medicaid benefits for mothers to a full year post-partum. “That is a great help in supporting us to follow the patients during the postpartum period and ensure their transition back to their primary care team and other subspecialists,” Dr. Dolin says.
Advertisement
Even in cases where planning has taken place, pregnant patients can experience SLE flares.
“It’s better to have their disease quiescent at conception,” says Dr. Dolin. “However, if they become pregnant, I am reassuring but also work to make sure that we aggressively manage the flare.”
Flares are typically treated with steroids, which can be used in pregnancy, but can carry risks of causing premature labor. They should be used carefully and for a short period of time. “We will already be watching these women very closely during the pregnancy, and maybe for that patient I would increase my surveillance even more,” says Dr. Dolin. “But overall, the most likely outcome is having a normal pregnancy.”
The compound complexities of pregnancy with SLE make cross-disciplinary collaboration important, the physicians say. The potential lupus has for affecting multiple systems often makes it essential for interdisciplinary care with care teams often including dermatology, ophthalmology, nephrology, cardiology, hematology and maternal-fetal medicine, adds Dr. Littlejohn.
“It’s not just the rheumatologist who is caring for these patients,” she says. “It really does take a village.”
In this video case study, Dr. Littlejohn discusses a case of a pregnant patients with SLE.
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/UqSmrR6fDO4?feature=oembed)
Systemic Lupus Erythematosus (SLE) and Pregnancy Planning
Advertisement

CAR T-cell therapy may offer reason for optimism that those with SLE can experience improvement in quality of life.
Advancements lead to a new trial involving autoimmune disease

A review of expanding options that hold new promise

Prescribing eye drops is complicated by unknown risk of fetotoxicity and lack of clinical evidence

ACOG-informed guidance considers mothers and babies

Psychological care can be a crucial component of medical treatment

Rare pregnancy complication can lead to fetal demise

Research may offer family-planning insights for those with the condition