Study uses molecular and clinical stratification to help guide patient selection
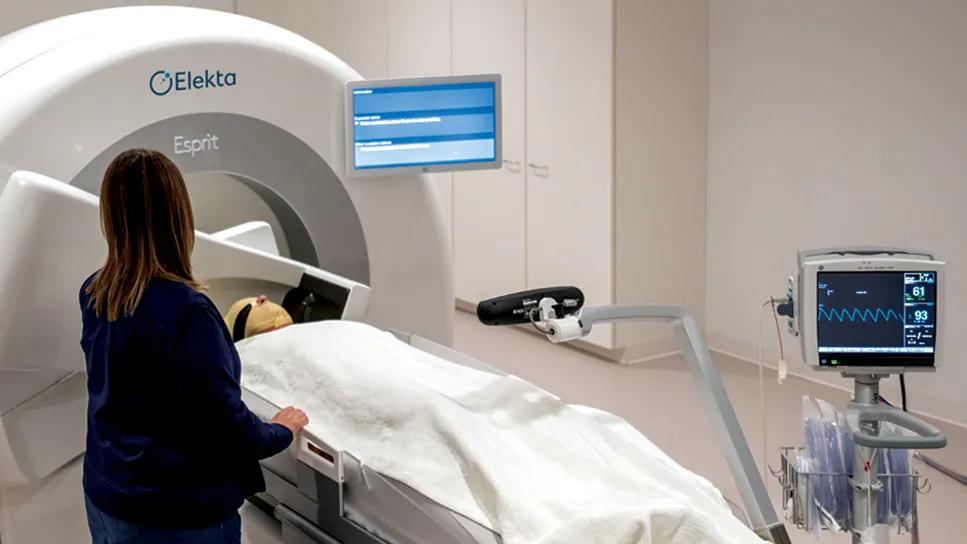
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8769b19b-3e45-4053-98e2-73f3020ca51c/gamma-knife-predicting-outcomes-in-gbm)
person going into a Gamma Knife machine for radiotherapy
For clinicians managing the nearly universal recurrence of glioblastoma, identifying effective salvage therapies remains an uphill battle. While stereotactic radiosurgery (SRS) offers a high-dose, targeted approach to focal recurrences, its utility has long been debated due to the diffuse nature of the disease and a historical lack of prospective evidence.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Now, a new retrospective study from Cleveland Clinic (J Neurooncol. 2025;176[2]:132) provides a roadmap for optimizing patient selection for this modality in recurrent glioblastoma. The study suggests that SRS is most effective when applied to a specific subset of patients characterized by smaller tumor volumes, longer intervals between initial diagnosis and recurrence, and specific molecular signatures, including retention of heterozygosity at the 19q13 chromosomal locus.
Notably, patients possessing at least two of these favorable markers experienced a twofold increase in overall survival compared with those who did not, reaching a median of 15.1 months after SRS.
The controversy surrounding SRS in glioblastoma management stems largely from a 2004 randomized controlled trial that found adding SRS to up-front standard-of-care therapy did not improve survival. Consequently, many institutions moved away from the technology for this indication. However, that landmark trial left critical questions unanswered: Does SRS provide value as a salvage therapy at the time of recurrence, and are there subsets of glioblastoma patients who are more likely to benefit based on specific characteristics?
With the proliferation of molecular and genetic testing in neuro-oncology practice, Cleveland Clinic researchers sought to determine whether routinely collected biomarkers could predict which patients would truly benefit from SRS as a secondary or tertiary line of defense.
“Glioblastoma has a poor prognosis, and many systemic treatments cause serious side effects,” notes the study’s senior and corresponding author, Lilyana Angelov, MD, Director of Cleveland Clinic’s Gamma Knife Center. “If a recurrence is small and in one area, and we can offer a high-dose treatment that might extend survival without affecting quality of life, we owe it to patients to explore that option.”
Advertisement
The investigators conducted a retrospective review of 49 adult patients (comprising 83 distinct lesions) treated with Gamma Knife® SRS for recurrent, IDH1-wildtype glioblastoma between 2010 and 2024. They analyzed the genetic and molecular features of each case at the time of initial diagnosis as well as serial radiography findings from initial diagnosis onward. “We want this therapeutic approach to be considered more widely, so we focused our analysis on data collected with diagnostic tools accessible to any modern hospital that treats glioblastoma,” Dr. Angelov explains.
Median patient age at the time of SRS was 61 years, and median tumor volume was 2.02 cm³. Most patients (83%) received single-fraction treatment, with a median prescription dose of 24 Gy. The researchers used multivariate Cox models to isolate clinical and molecular factors independently associated with progression-free survival and overall survival.
The study identified several critical variables that significantly influenced outcomes following salvage SRS:
Advertisement
The researchers note that while their study is limited by its retrospective nature and a relatively small sample size, it underscores the necessity of molecularly stratified prospective trials. They point out several actionable management insights for recurrent glioblastoma that emerge from their findings:
Advertisement
“Our findings suggest that the use of SRS may be an especially promising treatment modality for recurrent glioblastoma patients with certain favorable prognostic features,” the authors conclude. By identifying patients who may achieve a 15-month survival post-recurrence — a duration that rivals the historical survival of many patients from their initial diagnosis — clinicians can optimize patient selection for SRS in this setting.
“These findings are encouraging because they demonstrate that this essentially noninvasive outpatient therapy, when used in appropriately selected patients, confers a meaningful increase in post-recurrence survival,” Dr. Angelov observes. “A good portion of this extended survival comes with maintenance of neurological function — that is, without disease progression that can lead to weakness, speech difficulties and related challenges. What’s more, these benefits come with limited to no associated toxicity compared with alternatives such as chemotherapy. For these patients, it’s a win in terms of both quantity and quality of life.”
Advertisement
Advertisement
Phase 2 trials investigate sitagliptin and methimazole as adjuvant therapies
Advances in genomics, spinal fluid analysis, wearable-based patient monitoring and more
Researchers use AI tools to compare clinical events with continuous patient monitoring
Combining dual inhibition with anti-PD1 therapy yielded >60% rate of complete tumor regression
Cleveland Clinic researchers pursue answers on basic science and clinical fronts
New research from Cleveland Clinic helps explain why these tumors are so refractory to treatment, and suggests new therapeutic avenues
Presurgical planning and careful consideration of pathology are key to achieving benefits
Study demonstrates its role in tumor lethality, raises prospect of therapeutic targets