Patients with minimal disease activity report better physical and mental health as well as less fatigue
By Elaine Husni, MD, MPH and Juliette Yedimenko, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Discrepancy between patient reported outcomes (PROs) and clinical measures of disease activity in patients with psoriatic arthritis (PsA) who are known to be in remission can lead to under- or over-treatment of disease and patient dissatisfaction. This may be, at least in part, due to the limits of clinical disease activity measures in assessing the domains of health that are important to patients.
Patients diagnosed with PsA experience significantly poorer health-related quality of life than both the general population and those with psoriasis alone. Patients with PsA may experience pain, sleep disorders, diminished physical function and productivity, comorbidities such as cardiovascular disease, and cosmetic effects that negatively impact self-image and emotional health. They are also at higher risk for developing depression.
PROs provide valuable insight into patients’ perception of their disease, enhance communication between clinicians and patients, and help guide treatment decisions. Unfortunately, however, general health measures traditionally incorporate only a handful of PROs, and may provide a very limited patient reported assessment.
We recently conducted a cross-sectional study to examine the correlation between minimal disease activity (MDA) status and PROs. In the study, we compared data documented in the Patient Reported Outcomes Measurement Information System (PROMIS) to the physician clinical assessments of MDA status. Results from this work were presented at the 2019 American College of Rheumatology’s Annual Meeting.
Advertisement
Together with the Psoriatic Arthritis Research Consortium, we analyzed the records of 235 patients (51% female, mean age 51 ± 13.9) who met the Classification Criteria for Psoriatic Arthritis (CASPAR); were on treatment with biologic and non-biologic DMARDs, monoclonal antibodies antagonist IL 12/23 or IL17a, PDE4 inhibitor or JAK inhibitor; and were enrolled in the PARC database between 2016 and 2019. Of the patients, 129 were in MDA and 106 were not in MDA.
We assessed the following:
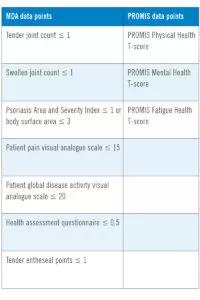
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/45763156-8615-4bb2-ace2-fdd906001025/19-RHE-1358-PROMISmeasures-psoriaticArthritis-table1-800x1200-1-200x300_jpg)
There was a significant positive correlation between MDA scores and PROMIS scores in the Physical and Mental domains, and a more moderate correlation between the MDA and PROMIS Fatigue T-Score. In other words, patients who were in MDA rated their physical and mental health better than those who had not achieved MDA. They also reported less fatigue when compared with non-MDA patients. There were no significant differences in demographics between patients with and without MDA.
We found that achieving MDA was associated with a positive effect on patients’ Physical, Mental and Fatigue PROMIS domains, irrespective of their demographics or PsA comorbidities; however, patients with a greater number of comorbidities were less likely to be in MDA overall.
PROs can provide valuable insight when they complement laboratory studies and physician assessment in PsA. This suggests the need for ongoing assessment of PROs in PsA patients. Additionally, rheumatologists should listen carefully when asking patients about symptoms that harm their quality of life to ensure a complete understanding of their needs and identify the best course of treatment to meet their patients’ goals.
Advertisement
In Cleveland Clinic’s Department of Rheumatologic and Immunologic Diseases, we recognize the value of PROs. In 2016, we deployed MyRheum, a computer-based program to collect PROs that is integrated with the electronic health record (EHR). PROMIS domains are administered using computer adaptive testing, and scores are standardized on a T-scale. Results are displayed within the EHR at the time of the visit, allowing the clinician to evaluate patient-reported health measures at the point of care, engage patients in their care and make better treatment decisions based on patient-centric data.
Dr. Husni (@ElaineHusniMD) is Director of the Arthritis and Musculoskeletal Center in the Department of Rheumatic and Immunologic Diseases and Cleveland Clinic’s Psoriatic Disease Biobank.
Advertisement
Advertisement

The case for continued vigilance, counseling and antivirals

High fevers, diffuse rashes pointed to an unexpected diagnosis

No-cost learning and CME credit are part of this webcast series

Summit broadens understanding of new therapies and disease management

Program empowers users with PsA to take charge of their mental well being

Nitric oxide plays a key role in vascular physiology

CAR T-cell therapy may offer reason for optimism that those with SLE can experience improvement in quality of life.

Unraveling the TNFA receptor 2/dendritic cell axis