Judicious application yields a 99.7% repair rate and 0.04% mortality
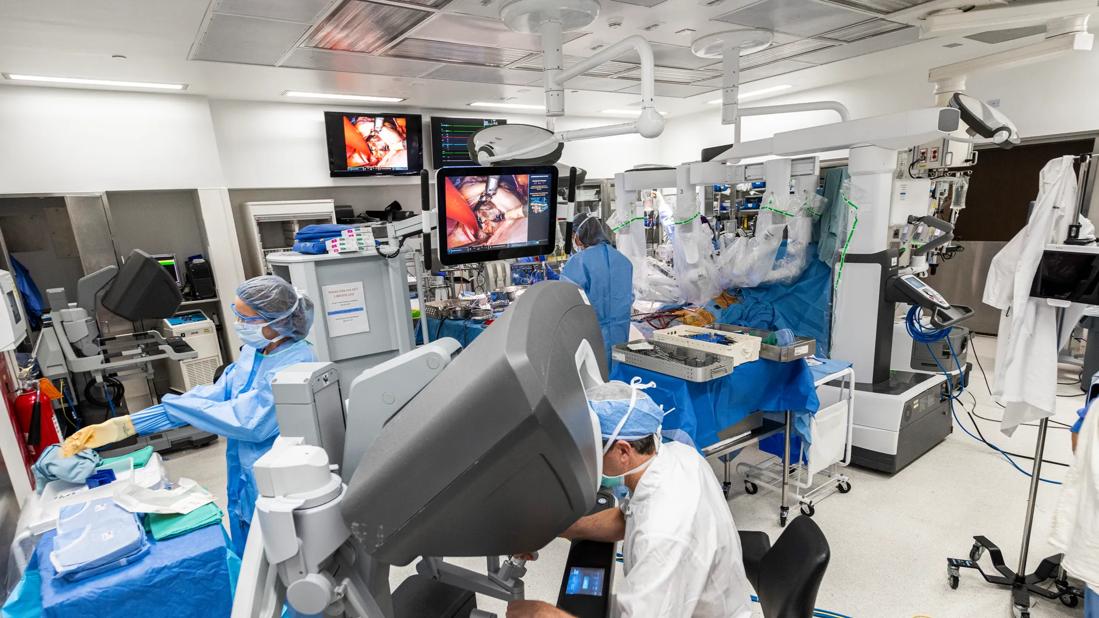
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1e42758e-943c-4202-8678-b374ea18d586/HVI_Valleriano_3312115_Dr-Gillinov-Robotic-Surgery_10-19-22_MLC)
operating room during robotic heart surgery
Robotically assisted mitral valve repair surgery holds clear appeal for patients: Its minimally invasive nature means shorter recovery time and better cosmetic results compared with full or partial sternotomy. For surgeons, it additionally offers unparalleled visualization into the heart.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This appeal has translated to continued embrace of the procedure at Cleveland Clinic, which performed its 2,400th robotically assisted mitral valve repair surgery in May 2024. This series of robotic procedures, which began nearly 20 years ago, was achieved with a 99.7% rate of repair (versus replacement) for isolated degenerative mitral valve disease and a mortality rate of 0.04%.
Additionally, the robotically assisted repairs done in the past decade make up an important share of the 4,600-plus consecutive mitral valve repairs overall that Cleveland Clinic has performed without an operative death through May 2024.
“Many patients with mitral valve disease come to Cleveland Clinic asking specifically for a robotically assisted repair,” says A. Marc Gillinov, MD, Chair of Thoracic and Cardiovascular Surgery. “While many of them are good candidates, some are not. What we can assure patients is that we’ll work with them to judiciously determine which option — whether it involves robotic assistance, another minimally invasive approach, or partial or full sternotomy — will give them the very best chance of a safe and lasting mitral valve repair.”
In lieu of sternotomy, robotically assisted mitral valve repair involves miniscule incisions for each of three arm ports as well as one working incision about 3-4 cm long between the ribs. The cameras housed in the robotic system enable the surgeon, seated at the robot console, to visualize parts of the valve at 10x magnification and 360-degree orientation.
Advertisement
“The motions of the robot arms and the articulation of the instruments are so precise that it mimics exactly the motions we direct from the console,” says Cleveland Clinic cardiothoracic surgeon Tarek Malas, MD, whose specialty interests include robotic and minimally invasive surgery.
Preoperatively, patients considered for robotically assisted repair undergo transthoracic echocardiography (TTE) as well as CT of the chest, abdomen and pelvis. The CT studies are done to ensure safe and effective femoral perfusion.
Postoperatively, patients undergoing robotically assisted repair have shorter length of stay, on average, than their open-surgery counterparts. Overall recovery is shorter as well, although it still takes two to four weeks for most patients. Patients are particularly pleased that they can drive within a week of robotic surgery, vs. four to six weeks of no driving after standard heart surgery.
Beyond acquisition of a robotic surgical system, another key aspect of what’s involved in these procedures is specialized training. “Robotic heart surgery requires the surgeon to learn a new skill set,” Dr. Gillinov says. “It’s not something you learn in medical school or in a regular residency. You need to do specialized training. Our sizeable team of experienced surgeons at Cleveland Clinic allows us to offer this instruction to our trainees.”
Cleveland Clinic’s approach in this realm is guided by a home-grown screening algorithm used to assess patients’ candidacy for a robotic procedure when undergoing repair for isolated degenerative mitral valve disease. The algorithm requires that candidates for robotic mitral valve surgery fulfill the following requirements based on imaging findings.
Advertisement
From TTE:
From CT of the chest, abdomen and pelvis:
A recent study published in the Journal of Thoracic and Cardiovascular Surgery (2022;164[4]:1080-1087) evaluated use of the algorithm across a 1,000-patient sample. It showed that 60% of screened patients qualified for robotic surgery and that these patients’ postoperative outcomes were just as good as those of patients undergoing mitral valve repair with sternotomy. “These findings validate this screening approach,” Dr. Gillinov notes. More recently, 70% of patients with isolated degenerative mitral valve disease have qualified for the robotic approach.
Although the study was not a randomized investigation, it also showed that patients in this large sample who underwent robotic surgery had several benefits compared with sternotomy patients, including statistically significant reductions in new-onset atrial fibrillation, red blood cell transfusions and hospital length of stay.
The Cleveland Clinic mitral valve surgery team describes their screening algorithm for robotic procedures as conservative. “It is our philosophy that minimally invasive surgery is only appropriate when it can be offered without sacrificing safety or quality,” Dr. Malas explains.
Dr. Gillinov notes that the algorithm was developed in response to specific needs during Cleveland Clinic’s initial experience with robotic mitral valve surgery. “This is not meant to be prescriptive for other centers,” he says, “but it has served us well. It has been an important contributor to our institution’s zero mortality for mitral valve repair over many years and our very high repair rate.”
Advertisement
“Robotic mitral valve repair is a great technique in appropriately selected patients, allowing more rapid recovery and cosmetic advantages,” adds Brian Griffin, MD, Medical Director of Cleveland Clinic’s Mitral and Tricuspid Valve Center. “The algorithm developed here has been very effective in providing outstanding outcomes in patients with degenerative mitral regurgitation.”
As the team’s experience has grown, Dr. Gillinov says, they have extended robotic surgery to patients with some degree of left ventricular dysfunction, mild mitral annular calcification and the need for concomitant procedures.
“We continue to explore robotic assistance in other areas of cardiac surgery practice,” he concludes. “For instance, we now offer robotically assisted coronary artery bypass grafting for selected individuals with coronary artery disease.”
Advertisement
Advertisement
NIH-funded comparative trial will complete enrollment soon
Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic
Why and how Cleveland Clinic achieves repair in 99% of patients
Two surgeons share insights on weighing considerations across the lifespan
An overview of growth in robot-assisted surgery, impressive re-repair success rates and more
Cleveland Clinic series supports re-repair as a favored option regardless of failure timing
A call for surgical guidelines to adopt sex-specific thresholds of LV size and function
Cleveland Clinic series shows re-repair is feasible with excellent midterm results