Cleveland Clinic experience is applicable to other laboratories
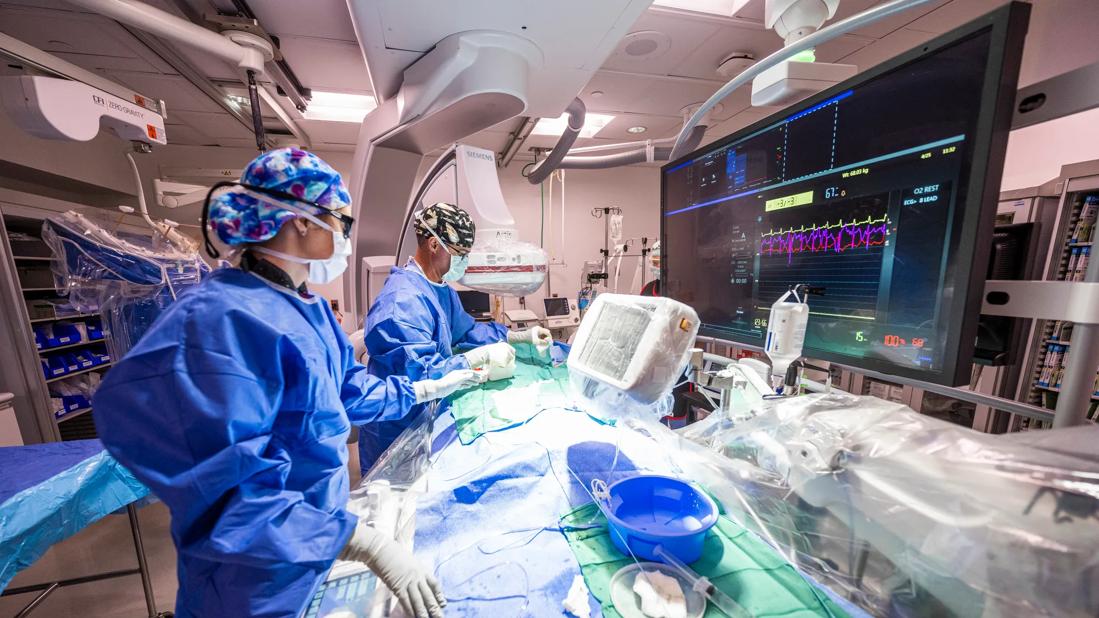
Implementation of radiation dose reduction measures for diagnostic catheterization or percutaneous coronary intervention (PCI) can lead to significant and sustained reduction in radiation exposure for patients and personnel without significantly affecting image quality. So concludes a study comparing air kerma before and after radiation reduction initiatives were adopted by Cleveland Clinic catheterization laboratories. The findings were reported in Catheter and Cardiovascular Interventions (2022;100[4]:575-584).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The measures we took were simple and generalizable to other facilities,” says study co-author Amar Krishnaswamy, MD, Section Head of Invasive and Interventional Cardiology at Cleveland Clinic. “I urge leaders in other cath labs to work with their vendors to adopt similar measures to reduce patient exposure and mitigate a major occupational hazard.”
Personnel radiation exposure has become an increasing problem in cath labs as the number and complexity of interventions have risen dramatically in recent years. While the dangers of ionizing radiation are well known and monitoring devices are mandatory, few advances have been made to actually reduce exposure of cath lab personnel.
“Although current technology offers radiation reduction mechanisms, relatively few users adopt them if they are different from so-called factory settings,” says study co-author Khaled Ziada, MD, Chief Academic Officer for Cardiovascular Interventions at Cleveland Clinic. “The cath lab leadership worked with the vendors to modify baseline acquisition settings and take better advantage of our existing systems.”
The study included adults who underwent diagnostic catheterization or PCI at any of eight cath labs on Cleveland Clinic’s main campus from January 2009 through December 2019. Propensity score matching (based on age, sex, body surface area, total fluoroscopy time and total acquisition time) yielded the following four cohorts:
Advertisement
Radiation dose reduction measures were instituted at the beginning of 2013, some of which required vendors to alter machine settings and default modes. Key measures included the following:
Total air kerma (i.e., a measure of the amount of ionizing radiation to which a patient is exposed) and fluoroscopy‐ and acquisition‐mode air kerma were compared between the periods before and after implementation of the radiation reduction initiatives for both diagnostic catheterization and PCI.
Radiation exposure was significantly reduced following the initiative, as evidenced by the following data from the propensity score-matched groups:
Drs. Krishnaswamy and Ziada emphasize that the measures their team instituted can be widely applied to other cath labs. They highlight the following additional points from the study.
Advertisement
Changing default settings to low doses is key. Laboratory leaders worked with system vendors to change machine settings so that using the low-dose settings took the least thought and effort on the part of operators. “Although the low-dose settings were previously available, they were almost never used,” Dr. Krishnaswamy notes.
Image quality was acceptable after radiation reduction. Multiple setting changes were tried to reduce radiation dose without compromising image quality. During each step of the process, image quality was assessed by blinded observers. In addition, feedback from operators was sought on a regular basis. “With the changes we ultimately agreed on, operators noted that the images were not as crisp, but the differences were modest and not clinically significant,” Dr. Ziada says. “Since the radiation dose reduction was significant, the compromise seems to be a winning one.”
“We instituted these measures with the goal of ALARA [as low as reasonably achievable] for radiation exposure,” Dr. Krishnaswamy adds. “We met this standard, as exposures were significantly reduced and the resulting decline in image quality was not prohibitive.”
Leadership and staff buy-in are critical. Radiation reduction was set as a priority by cath lab directors, and cultural changes were encouraged throughout the staff with training, education and follow-up.
Dr. Ziada adds that exciting new developments are in the pipeline, including the use of artificial intelligence to better obtain and process images.
Advertisement
“In this study we took advantage of easy fixes to imaging with existing technology,” he says, “but coming innovations in optimal image acquisition and post-processing are likely to be the next big steps in reducing radiation exposure. I expect the next-generation systems to allow further reduction in radiation dose with the help of more intensive image processing using more powerful computing and AI algorithms.”
Advertisement
Advertisement

Medical and surgical perspectives on current and emerging uses of ECMO and Impella

Least-invasive open-heart AVR option to date yielded rapid recovery in all cases

Launch of the tool promises to reshape quality assessment across the specialty
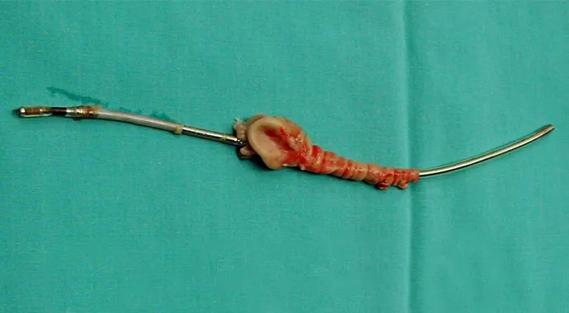
Lead dwell time and manufacturer emerge as independent predictors of success in registry study
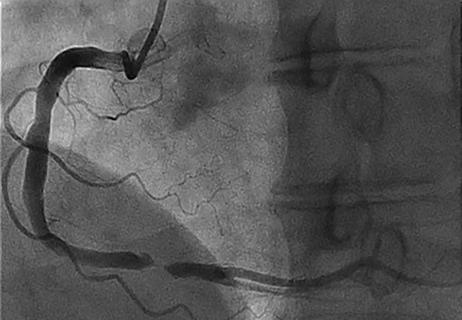
The case for a thoughtful approach to CTO and minimally invasive options for CABG

How the tool could help physicians alter management in real time
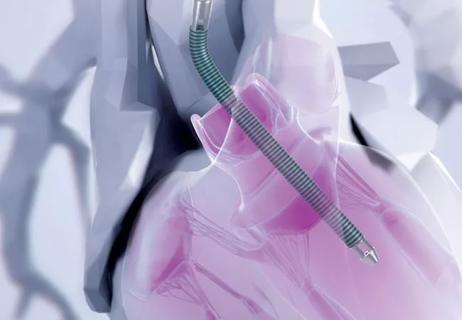
Preoperative Impella 5.5 placement can provide a critical safety net for high-risk patients
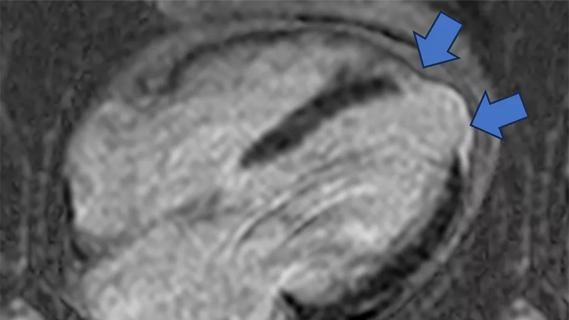
Technique may lay groundwork for personalized decision-making in procedural intervention