Using donor organs efficiently to help the most patients
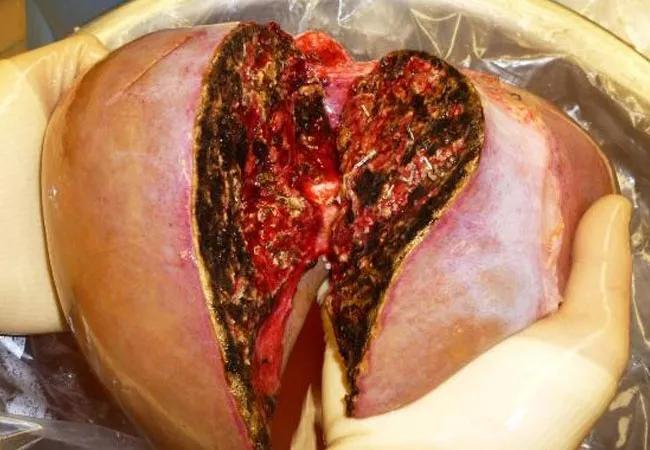
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/72913233-f591-4374-8759-52274de580f5/Split-Liver_jpg)
Split-Liver
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As one of the solutions for severe donor shortage in liver transplantation, Cleveland Clinic performed two liver transplants simultaneously from one deceased donor by splitting a liver graft into two hemiliver grafts.
This highly complex procedure requires an experienced surgical team with expertise in both transplant surgery and hepatobiliary surgery. Because splitting a whole liver graft creates two smaller partial grafts, the risk of liver transplant failure is generally considered to be higher than liver transplantation using a whole liver graft. As a result, this procedure remains underutilized.
The patients are a 65-year-old female with primary biliary cirrhosis and a 54-year-old male with hepatitis C-related cirrhosis and hepatocellular carcinoma. Both were listed for liver transplantation at Cleveland Clinic. A brain-dead donor became available and the decision was made to proceed with split-liver transplantation. Our donor team split the whole liver in situ before the liver was procured from the donor. The split liver grafts were brought back to Cleveland Clinic’s main campus to be simultaneously transplanted into the two recipients. Despite complex vascular and biliary anastomoses, both recipients did very well with excellent liver graft function. The patients were discharged from hospital in six and nine days, respectively.
Advertisement
Advertisement
Advertisement
Research demonstrates cirrhosis regression in one-third of patients, with higher rates using alternative assessment
Elevated risk persists for more than a year after surgery, plus more insights from the first study to quantify risk specifically for CRC surgery
Large, retrospective study indicates improved outcomes after one and five years of treatment
Multidisciplinary collaboration is fueling breakthroughs in endoscopic and surgical technology
A surge in transplants, advanced surgical techniques and multidisciplinary collaboration has helped shape and expand the Liver Transplant Program
Retrospective analysis finds lower mortality rates, fewer hospital visits among patients with Type 1 diabetes using GLP-1 Therapies
Benefits of neoadjuvant immunotherapy reflect emerging standard of care
Multidisciplinary framework ensures safe weight loss, prevents sarcopenia and enhances adherence