Why setting patients’ expectations and an enhanced pathway might be the key

Same-day discharge (SDD) protocols following minimally invasive sacrocolpopexy are associated with safety, feasibility and high satisfaction among patients, according to the findings of one new Cleveland Clinic-led study. The team published their findings in Female Pelvic Medicine & Reconstructive Surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Once considered a procedure that required a one- to two-night hospital stay, patients undergoing pelvic floor reconstructive surgery at Cleveland Clinic can typically expect to be discharged within the same day.
A 2018 study, published in the Canadian Journal of Urology, established its safety and feasibility as an outpatient procedure — something that Howard B. Goldman, MD, urologist and a co-author on both papers, says he has noticed anecdotally for several years.
In the 2018 study, researchers compared the results of 10 patients who were discharged the same day with 30 patients who remained in the hospital overnight. They found that patients who were discharged the same day they underwent surgery were no more likely to require an unscheduled emergency room or office visit during this period. Satisfaction rates among both cohorts were comparable.
Building on this, researchers set out to test the utility of the same-day protocol used to guide SDD. To date, no such study has prospectively evaluated SDD following a minimally invasive sacrocolpopexy. Dr. Goldman, who is also Vice Chair at Cleveland Clinic’s Glickman Urological & Kidney Institute, says the goal was to compare safety, postoperative healthcare utilization and satisfaction in patients following the SDD protocol versus that of those receiving routine care.
The team of female pelvic medicine and reconstructive surgery specialists prospectively examined 47 women undergoing minimally invasive sacrocolpopexy for pelvic organ prolapse from November 2018 to July 2019. In addition to routine preoperative counseling, patients watched a video to help facilitate the SDD protocol. Care teams followed the enhanced recovery after surgery pathway to help facilitate SDD (Table 1).
Advertisement
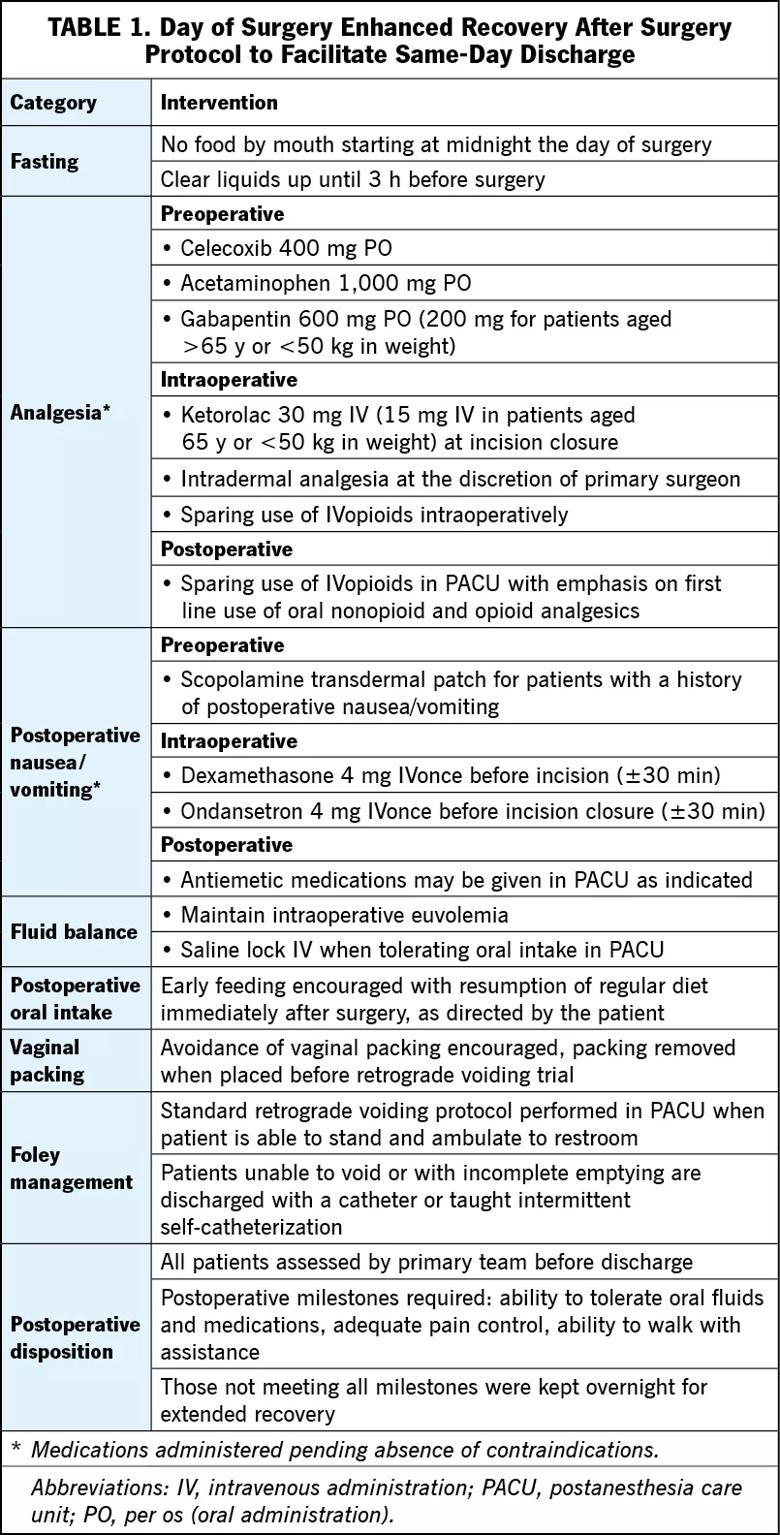
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/9ac96ace-e4d2-42c1-841e-d1d9180c7185/805x-Inset-Goldman-Same-Day-Discharge_jpg)
Hickman LC, Paraiso MFR, Goldman HB, et al. Same-Day Discharge After Minimally Invasive Sacrocolpopexy Is Feasible, Safe, and Associated With High Patient Satisfaction. Female Pelvic Med Reconstr Surg. 2021 Jan 4;Epub ahead of print. Reprinted with permission from Female Pelvic Medicine & Reconstructive Surgery.
Within this cohort, nearly 80% of patients went home on the same day as planned. There was no difference in healthcare utilization or the occurrence of adverse events between these two groups. Importantly, the patient satisfaction rate was high with 95.7% of study participants reporting overall satisfaction.
Dr. Goldman says studies like this are important to affirm sacrocolpopexy as an outpatient procedure, particularly because sending patients home on the same day remains somewhat of a paradigm shift in the field for this procedure.
“With the right support measures in place, most patients do recover better at home. Extended stays aren’t necessarily beneficial to patient care and may, in fact, incur unnecessary healthcare costs.”
“Personally,” says Dr. Goldman, “I think one of the most important things we can do to help facilitate same-day discharge is managing patient expectations. If we communicate early on that it’s our goal for them, most patients are motivated by it.”
Of course, there is always the potential for complications. He notes that following these patients longitudinally is likely to better characterize the long-term outcomes. The team has been looking at data to assess whether longer lengths of stay would have helped mitigate a poor outcome. So far, length of stay does not appear to be associated with a change in complication rates. They presented these findings at the Society of Urodynamics, Female Pelvic Medicine and Urogenital Reconstruction national meeting held February 25 – 27, 2021.
Advertisement
He continues, “The more we can demonstrate the safety and acceptability of same-day discharge for these patients in the literature, the more we can normalize this as a best practice.”
Advertisement
Advertisement

Uterine transposition cleared the field for radiation therapy

ACOG-informed guidance considers mothers and babies

Prolapse surgery need not automatically mean hysterectomy

Artesunate ointment shows promise as a non-surgical alternative

New guidelines update recommendations

Two blood tests improve risk in assessment after ovarian ultrasound

Recent research underscores association between BV and sexual activity

Psychological care can be a crucial component of medical treatment