
Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve

Cardiac imaging substudy is the latest paper originating from the VANISH trial

Pre and post-surgical CEEG in infants undergoing congenital heart surgery offers the potential for minimizing long-term neurodevelopmental injury
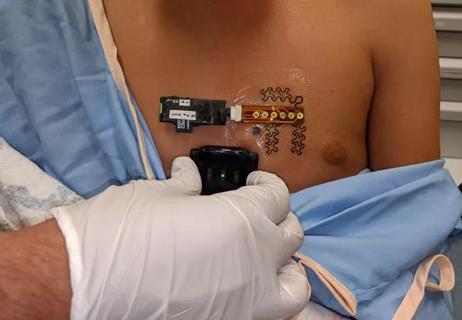
Early projects include predicting cardiac arrest, kidney injury and low cardiac output syndrome after surgery
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
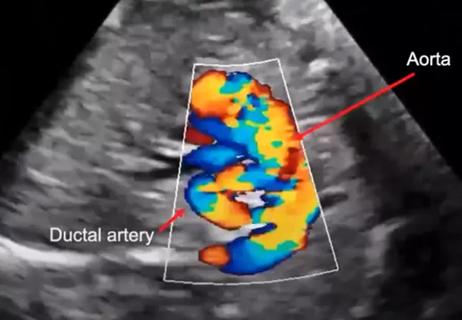
New course highlights role of imaging in the diagnosis and management in TOF

How can we use them to our advantage?

Researchers confirm underlying contributors to success

Coordinated subspecialty care improves survival, functional outcome.

Refinements introduced to Cleveland Clinic-developed approach to a rare defect
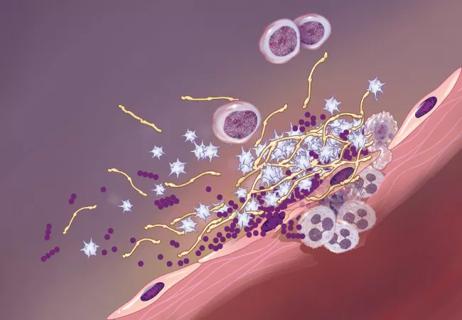
When no source can be found, suspect infective endocarditis
Advertisement
Advertisement