
Researchers pair quantitative imaging with AI to improve surgical outcomes in nonlesional epilepsy

Insights on how stereoelectroencephalography is continuing to improve seizure localization

Progress in stereoelectroencephalography for epilepsy surgery evaluation since Cleveland Clinic performed the first U.S. case in 2009
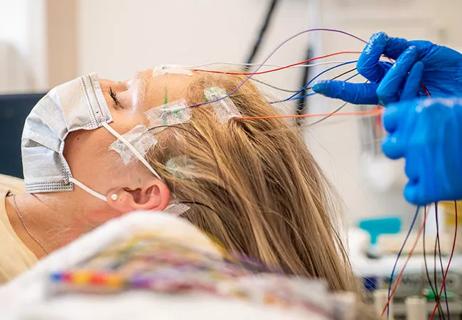
Model relies on analysis of peri-ictal scalp EEG data, promising wide applicability
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy

Data-driven methods may improve seizure localization and refine surgical decision-making
Multivariable models help estimate risk of postoperative declines in cognition and mood

ILAE advises emphasizing options for patients with drug-resistant epilepsy
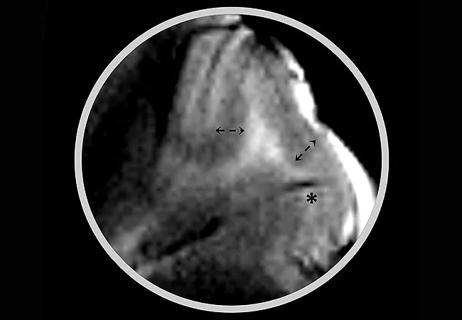
Mounting support for the newly described microstructure from a 7T MRI and electroclinicopathologic study

Surgery can be a game changer when medications fail to control seizures

Machine learning models shown to accurately separate lesions from normal brain, distinguish lesion subtypes
Advertisement
Advertisement