
Study is first to show reduction in autoimmune disease with the common diabetes and obesity drugs

Therapies include steroid implants, immunomodulation and biologics
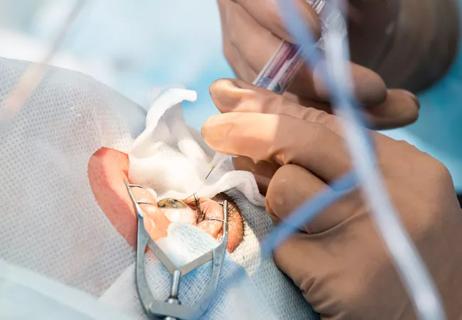
How to screen for and manage treatment-triggered uveitis
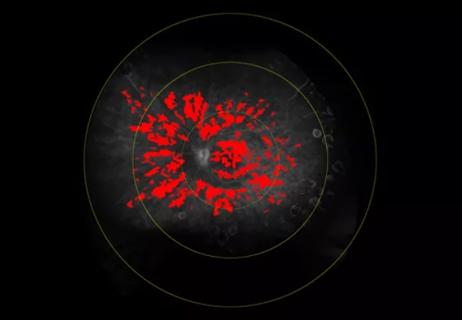
Automated diagnosis, risk stratification and treatment assessment are feasible
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy

Herpetic retinal infection has high rate of recurrence
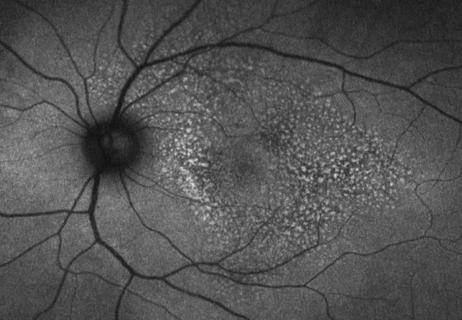
Treatment differs from other types of uveitis
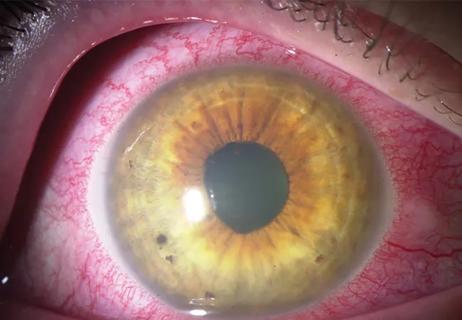
Study assesses utility of patient-reported outcomes measures in uveitis and scleritis
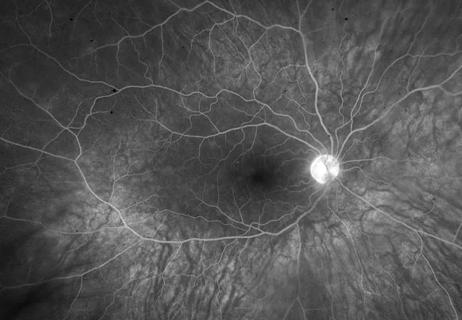
Teen with uveitis, glaucoma, cataract illustrates value
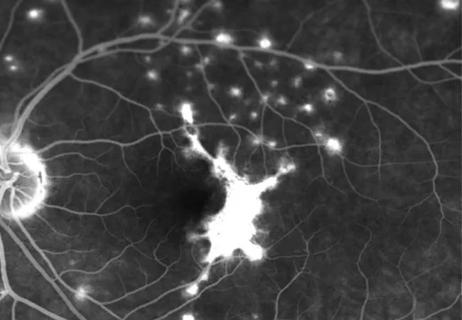
If you can’t see it, you can’t treat it
Advertisement
Advertisement