Surgeons also report benefits of integrated heads-up display
Initially used only on an outpatient basis, optical coherence tomography (OCT) first made its way into the surgical arena via handheld systems. It eventually progressed to microscope-mounted external intraoperative OCT (iOCT), positioning the technology to become widely available. Microscope-integrated iOCT systems received clearance from the U.S. Food and Drug Administration in 2014 and 2015.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The evolution of the technology continues today with 3D digitally-enabled viewing systems that integrate iOCT. According to a study presented at the Association for Research in Vision and Ophthalmology (ARVO) 2022 meeting, a 3D viewing system may provide additional benefits compared to conventional microscope-integrated iOCT.
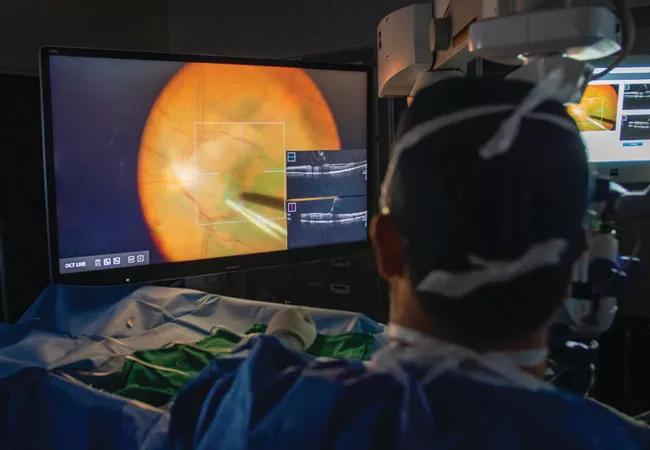
“Intraoperative OCT is useful to see what’s going on in the retina at the time of surgery and to better understand the pathology, but how we integrate it into new surgical visualization technology, including using a three-dimensional heads-up display, is unique,” explains ARVO presenter Katherine Talcott, MD, of Cleveland Clinic Cole Eye Institute.
This study was a post-hoc case-control analysis from the DISCOVER study, a prospective iOCT study led by Dr. Talcott’s mentor Justis P. Ehlers, MD, Director of The Tony and Leona Campane Center for Excellence in Image-Guided Surgery and Advanced Imaging Research at the Cole Eye Institute. It focused on a new commercially available 3D digital visualization system, the Artevo 800 (Zeiss). Dr. Talcott says the Artevo is purported to have benefits over existing systems, such as less lag time, more accurate color and larger intraoperative OCT images.
“There really haven’t been studies comparing an Artevo system to a regular system, and definitely none that have talked about how intraoperative OCT is integrated, so we wanted to see how retina surgeons use this new system and report any potential benefits from using it,” she says. “We looked at patients from that larger [DISCOVER] study who had intraoperative OCT images, but we also used the 3D heads-up display to be able to compare how physicians use it.”
Advertisement
Researchers compared two groups, each consisting of 100 eyes from 100 subjects. In one group surgeons used conventional microscope-integrated iOCT (Rescan 700, Zeiss), and in the second group surgeons used 3D digitally-enabled iOCT (Artevo 800, Zeiss). Researchers optimally matched the subjects for surgeon and preoperative diagnosis. The majority of surgical indications were for epiretinal membrane, retinal detachment and macular holes. Immediately after surgery, standardized questionnaires were collected from the surgeons.
The main objective of the study was to compare the efficiency of both surgical- and nonsurgical-field-based visualization. The conventional iOCT group used ocular heads-up display while the digitally-enabled group used 3D screen-based visualization. Additionally, the researchers compared surgeon perception of iOCT utility and the direct impact of iOCT on surgical decisions.
The study found that 3D digitally-enabled microscope-integrated iOCT enabled significantly higher surgical-field-based visualization of the iOCT datastream (88% 3D vs. 7% conventional).
“The OCT images that are displayed through the 3D digitally-enabled system are amazing — they’re very large and there’s great detail,” says Dr. Talcott. “And you can review those intraoperative OCT pictures just by looking at the screen.”
Surgeon-perceived utility of iOCT was similar — and high — in both groups (60% 3D vs. 53% conventional).
“Similar to what we’ve seen in the larger intraoperative OCT studies, we found that iOCT gives a great deal of information about the eye and can, in some cases, change the surgical management,” says Dr. Talcott.
Advertisement
The direct impact of iOCT on decisions made during surgery was similar in both groups as well (21% 3D vs. 16% conventional).
“Getting that extra information in real time can sometimes allow you to avoid additional surgical maneuvers,” says Dr. Talcott.
Because surgeons didn’t need to look away from the screen with the 3D heads-up modality, Dr. Talcott says this translated into ergonomic benefits, including less back pain and headache. Another benefit of the 3D system is that less light is needed in the eye, “which translates to better safety for the patient,” says Dr. Talcott.
“Anything we can do to make retina surgery safer for patients and more comfortable for retina surgeons is important. This study highlights that new innovations can improve both of those factors,” she adds. “Hopefully our work showing the potential benefits of this technology will help increase its use.”
Advertisement
Advertisement

Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma

Registry data highlight visual gains in patients with legal blindness

Prescribing eye drops is complicated by unknown risk of fetotoxicity and lack of clinical evidence

A look at emerging technology shaping retina surgery

A primer on MIGS methods and devices

7 keys to success for comprehensive ophthalmologists

Study is first to show reduction in autoimmune disease with the common diabetes and obesity drugs

Treatment options range from tetracycline injections to fat repositioning and cheek lift