CPAP found to have multiple physiologic advantages
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The discovery of surfactant was one of the most significant events to occur in the history of neonatology. Certainly, surfactant saved lives for premature infants who were otherwise considered nonviable. However, the prevention of chronic lung disease (CLD) did not progress, and it became clear that a significant portion of the help surfactant provides to the premature lung is counteracted by mechanical ventilation.1
The incidence of CLD differs significantly among institutions even after adjusting for centers’ distributions of birth weight, race and sex. The wide variability could not be explained by biological factors and, therefore, respiratory management was considered key to creating or preventing CLD. The lowest incidence of CLD in literature has been reported from centers that use bubble CPAP (b-CPAP) as early as possible, preferentially in the delivery room and as the primary mode for respiratory support of all premature infants in respiratory distress.2
I have previously demonstrated the reproducibility of b-CPAP use. In a center that had 33 percent of its very low birth weight (VLBW) infants develop CLD, the implementation of a b-CPAP program was associated with a reduction of CLD to 6 percent. However, the reduction of CLD rates did not occur immediately – it required significant time to develop staff experience and to achieve the full effect of b-CPAP. In a follow-up study, I demonstrated the consistency of outcomes over 12 years with a CLD rate of 5 percent.3
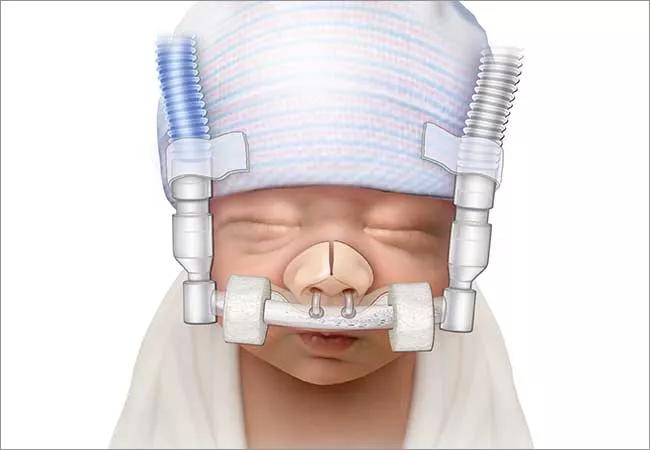
The bubble CPAP apparatus is simple; it is composed of a breathing circuit with an inspiratory limb delivering heated humidified gas mixture to the infant and an expiratory limb immersed under water in a container to create the desired pressure. Gas flow generates bubbles under the water that cause oscillations of the water level and subsequently of the pressure delivered to the patient. Therefore, the patient on b-CPAP receives an oscillating rather than a constant pressure. This oscillation effect may add to the efficacy of b-CPAP in volume recruitment.
Advertisement
CPAP has multiple physiologic advantages. In spontaneously breathing premature infants, it eases respiratory efforts by stenting the airway and the diaphragm. It maintains alveoli inflated, increases the functional residual capacity of the lung, and optimally matches ventilation with perfusion. Compared with mechanical ventilation and tracheal intubation, CPAP minimizes volutrauma and subsequent biotrauma. CPAP induces a favorable strain that stimulates lung growth when administered to animals over a prolonged time.4
Multiple randomized controlled trials were launched to compare the efficacy of early nasal CPAP to mechanical ventilation. These trials did not specify b-CPAP, but rather used any type of CPAP and did not offer details of competency-based training to ensure its efficacious use. Despite these reservations, trials confirmed the feasibility of applying CPAP early in life to premature infants, including those at the extreme premature age of 24-25 weeks, without change in mortality and CLD.
When these trials were considered collectively in a recent meta-analysis, early use of CPAP had a marginal benefit for the composite outcome of survival without CLD when compared to prophylactic surfactant with intubation. These findings do not reconcile with recurring reports on substantial reduction of CLD in neonatal units that used b-CPAP.
There are two factors that could explain the reduced CLD in b-CPAP units. The first is the type of CPAP and the type of nasal prongs. The second is the competency of the caregiver using b-CPAP at the bedside. Therefore, b-CPAP strategy is a complete bundle of care that requires clear practice guidelines and training process. In an effort to help neonatal units reproduce b-CPAP success, we offer a hands-on training program that familiarizes staff with b-CPAP components, indications for use, method of application, check points for maintenance, troubleshooting of problems, weaning methods and criteria for b-CPAP failure.2
Advertisement
No studies have compared CLD in infants supported with b-CPAP versus infants supported with other CPAP devices. Data are scarce on short-term endpoints, including work of breathing and oxygenation that favored b-CPAP. Nonetheless, numerous studies compared short-term outcomes of using CPAP, biphasic nasal CPAP, nasal intermittent positive pressure ventilation, and high-flow nasal cannula while using various types of facial and nasal interfaces.
The American Academy of Pediatrics Committee on Fetus and Newborn recently acknowledged the deficiency of data on efficacy and safety of these modalities. Of note, none of these non-invasive modalities could mimic the success of b-CPAP in reducing CLD. In the absence of data on CLD reduction, the extrapolation that all CPAP and non-invasive techniques are as efficacious as b-CPAP are realistically unfounded.1
References
Advertisement
Dr. Aly is Chair of the Department of Neonatology, Cleveland Clinic Children’s, and Professor of Pediatrics, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University.
Advertisement
Advertisement

One pediatric urologist’s quest to improve the status quo

Overcoming barriers to implementing clinical trials

Interim results of RUBY study also indicate improved physical function and quality of life

Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner

The benefits of this emerging surgical technology

Integrated care model reduces length of stay, improves outpatient pain management

A closer look at the impact on procedures and patient outcomes

Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve