Head and neck surgeons discuss the perplexing case
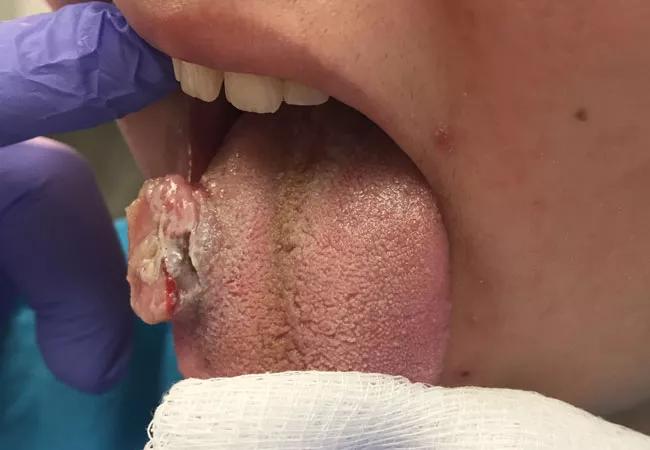
When a 19-year-old woman presented with an exophytic tongue mass, treating physicians, staff surgeon Robert Lorenz, MD, MBA, and Joseph Meleca, MD, a fourth-year resident, both in Cleveland Clinic’s Head & Neck Institute, were puzzled.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The presentation was clinically concerning, particularly given the patient’s young age and lack of obvious risk factors,” says Dr. Meleca.
The neoplasm developed one year prior to presentation and never completely healed. On examination, there was an ulcerated 3 x 2 cm mass, causing the patient severe pain, otalgia and dysphagia. Three weeks prior to the clinical encounter, the mass increased in size and was visibly engorged. The patient did not have a history of alcohol or tobacco abuse.
The biopsy of the mass demonstrated pseudoepitheliomatous hyperplasia and abundant acute and chronic inflammation with eosinophils. It also revealed traumatic ulcerative granuloma with stromal eosinophilia.
Dr. Meleca notes that the pathologist raised concern about the possibility of sampling bias given the overlying ulceration that cushioned the mass. “This added to the urgency of the situation,” he says. “Given the sampling concern, and concern for malignant potential, we resected the mass en bloc with clean margins.”
The physicians could not rule out human papillomavirus-related squamous cell carcinoma at first, although those tumors are less likely to occur in the anterior oral cavity. They also considered non-HPV-related squamous cell carcinoma of the oral cavity, though the patient did not have any known risk factors for this etiology.
Plexiform neurofibroma and granular cell tumors were both considered, as they share the same proteins as the patient’s mass, testing positive for SOX-10 and S-100. Upon closer review, plexiform neurofibromas are characterized by spindle cells, like the mass in question, but the presentation was more heterogeneous. Granular cells are more robust and dimensional than those of the tumor.
Advertisement
Histology revealed spindled cells positive for S-100 and SOX-10 proteins and overlying inflammation consistent with schwannoma with surrounding traumatic ulcerative granuloma with stromal eosinophilia-like (TUGSE) reaction.
“Schwannoma is a nerve sheath tumor that can occur anywhere in the body, but commonly develops in the head and neck region,” says Dr. Lorenz. Repetitive trauma, caused by the patient biting the mass, created a robust inflammatory reaction — the mass that raised clinical concerns about a more nefarious type of tumor.
Two years after this presentation, the patient has not experienced recurrence. While final pathologic reports indicated that the tumor was, indeed, schwannoma with TUGSE, the initial biopsy did not fully represent the mass, only capturing the ulcer, inflammation and squamous epithelium – not the submucosa.
The case illustrates an interesting dichotomy of a benign neoplasm that developed a grossly inflamed and clinically concerning appearance due to the repetitive trauma incurred over time.
“The two very important takeaways here are acting quickly given the clinical presentation, which warranted resection, but also taking a moment of pause to adequately sample the lesion and keep from performing a much larger resection had it been malignancy. Both were key in this scenario,” says Dr. Lorenz.
This case study was published in JAMA Otolaryngology–Head & Neck Surgery in May 2019.
Advertisement
Advertisement

Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor

Case study illustrates the potential of a dual-subspecialist approach

Evidence-based recommendations for balancing cancer control with quality of life

Study shows no negative impact for individuals with better contralateral ear performance

HNS device offers new solution for those struggling with CPAP

Patient with cerebral palsy undergoes life-saving tumor resection

Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition

Detailed surgical process uncovers extensive middle ear damage causing severe pain and pressure.