Pediatric rheumatologist discusses rare diagnosis, aggressive treatment regimen and outcomes
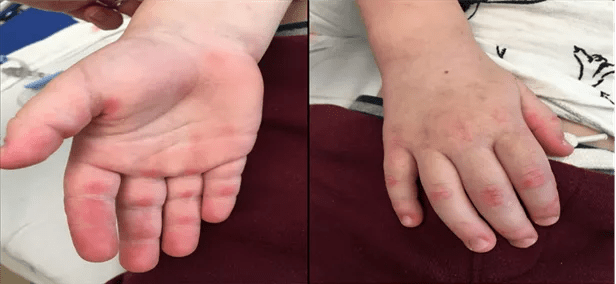
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3ea1a871-196f-4079-a89f-bed18084bd67/image001_png)
image001
In August 2019, a 3-year-old boy presented to the Cleveland Clinic Center for Pediatric Rheumatology and Immunology with a three-month history of multiple erythematous patches on his face, arms, elbows and extensor surfaces of both knees. He also had erythematous papules on the dorsal and palmar aspects of finger joints consistent with Gottron papules. He was active and playful without signs of muscle weakness. He was initially evaluated by a dermatologist who referred him to the center for further evaluation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The characteristic skin findings led to an initial diagnosis of juvenile dermatomyositis (JDM), an uncommon autoimmune disease typically affecting muscles and skin. Children with JDM can have certain autoantibodies that are associated with skin, muscle and lung involvement which vary in severity. JDM may be triggered by a viral infection. “Some patients have a genetic predisposition to JDM just as they do to other autoimmune diseases,” says Sirada Panupattanapong, MD, a rheumatologist at the Center for Pediatric Rheumatology and Immunology.
He also had a history of asthma presenting with non-productive coughing and wheezing. The combination of JDM and respiratory symptoms raised a concern for anti-MDA5 juvenile dermatomyositis, a distinct clinical phenotype of JDM which is more prevalent in East Asia than North America and Europe. Melanoma differentiation-associated gene 5 (MDA5) is a cytosolic protein essential for antiviral host immune responses and a well-described autoantigen target in a subset of patients with dermatomyositis.
As in this patient, anti-MDA5 JDM has a lower incidence of myositis and a higher incidence of lung disease. Because it is rare, anti-MDA5 JDM is often overlooked which can negatively affect patient outcomes.
The initial work-up with muscle enzyme levels included creatinine kinase, aldolase and lactate dehydrogenase which were within normal ranges for the patient’s age. The myositis-specific antibody panel revealed anti-MDA5 positivity. A chest x-ray showed signs of increased interstitial lung markings; interstitial lung disease (ILD) is a serious complication of anti-MDA5 JDM, which can lead to a worse prognosis. The test results confirmed a diagnosis of anti-MDA5 JDM with rapidly progressing (RP)-ILD.
Advertisement
There are no specific treatment guidelines for anti-MDA5 JDM-ILD in children, so the standard initial therapy for JDM was used: a tapering course of prednisolone and IVIG (2 grams/kilogram) every four weeks. Mycophenolate mofetil (MMF) was used instead of methotrexate to avoid the possibility of lung toxicity from methotrexate and because of the family history of alfa-1 antitrypsin deficiency. MMF is commonly used to treat scleroderma-ILD. “If we treat the patient early and aggressively with various immunosuppressants, we can achieve a better outcome,” says Dr. Panupattanapong.
At three months, the patient’s skin rash worsened so hydroxychloroquine was started. After five months of therapy, his skin disease significantly improved but a repeat CT scan showed increased opacity of the left lower lobe. Given the refractory nature of the disease, treatment was escalated by increasing the frequency of IVIG to every three weeks and adding one dose of rituximab (750 milligrams/m2). Rituximab is effective in treating refractory JDM and adult anti-MDA5 dermatomyositis with ILD.
“Rituximab is used for rheumatology conditions that don’t respond to conventional therapy. If we use the right dose based on body surface area, rituximab is safe at any age. Interstitial lung disease is difficult to treat and can cause long-term symptoms, which we wanted to do everything possible to prevent,” says Dr. Panupattanapong.
After six months, a CT scan showed significant improvement in lung opacity. The latest CT scan at 24 months following treatment showed near complete resolution of the airspace opacity. “Today, the patient is doing very well and looks like a healthy child. This case emphasizes the importance of monitoring for early signs and symptoms of lung disease in patients with anti-MDA5 JDM and treating it aggressively from the start. If you don’t treat the inflammation, it can become fibrocystic and irreversible,” says Dr. Panupattanapong.
Advertisement
She advises clinicians that a rash that looks like eczema may be a symptom of JDM. “If the rash doesn’t improve from treatment and the child also complains of muscle weakness and other symptoms, including lung and joint pain, they should suspect JDM and refer the patient to rheumatology,” she says.
Advertisement
Advertisement
How to use? Consider starting during the acute attack and seek patient preferences for chronic use
Similarly, patients with noninfectious uveitis have a higher risk of being diagnosed with an autoimmune disease within five years
Distinct MRI signature includes lesions beyond the corpus callosum, features predictive of vision and hearing loss
Despite less overall volume loss than in MS and NMOSD, volumetric changes correlate with functional decline
Unraveling the TNFA receptor 2/dendritic cell axis
Nasal bridge inflammation, ear swelling and neck stiffness narrow the differential diagnosis
Genetic testing at Cleveland Clinic provided patient with an updated diagnosis
It’s time to get familiar with this emerging demyelinating disorder