Increases may be related to opiate crisis and access to reproductive healthcare
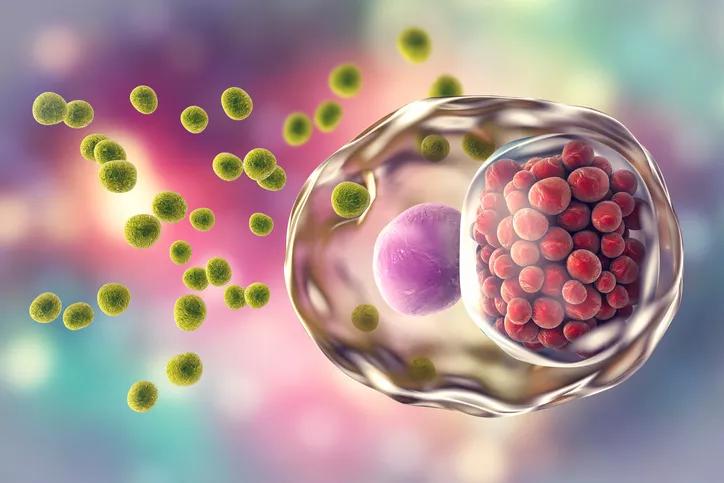
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/53e79397-6ba9-4622-b3f0-0f594c528a74/GettyImages-892829938-jpg)
STD
A recent report from the Centers for Disease Control and Prevention found significant increases in the rates of syphilis, gonorrhea and chlamydia from 2017 to 2018. Nationally, this is the fifth consecutive year that STD infection rates increased. Perhaps most tragic is the increase in congenital syphilis rates, which were up 40% to 1,300 reported cases in 2018. Alarmingly, newborn deaths related to syphilis increased 22%, from 77 deaths in 2017 to 94 deaths in 2018.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The opiate crises may be playing a role in the increasing rates of sexually transmitted infections (STIs), as past studies have indicated links between illicit drug use and risky sexual behaviors, ” states Oluwatosin Goje, MD, an Ob/Gyn and a fellowship-trained Reproductive Infectious Diseases Specialist in Cleveland Clinic’s Ob/Gyn & Women’s Health Institute. “Additionally, increasingly limited access to STI testing and treatment – with the closure of reproductive healthcare clinics across the country – may be a factor.”
Congenital syphilis
Ohio was among 17 states to see an increase in congenital syphilis rates. Congenital syphilis is a rare, disabling condition spread through the placenta from an infected mother to her infant. A diagnosis of syphilis in pregnancy is always treated as soon as possible. With successful maternal treatment, infants tend to have positive outcomes.
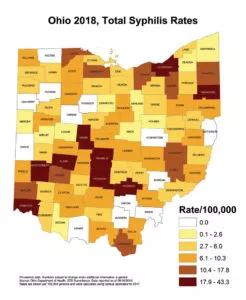
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/69de7948-4085-430f-a7d6-aaa937acf381/19-OBG-1459_CQD-inset-Syphillis-246x300_jpg)
If undetected, congenital syphilis can be a life-threatening infection in infants. Many babies with congenital syphilis are stillborn. Others may be asymptomatic at birth and develop symptoms over time, such as an enlarged liver, failure to thrive, irritation of skin around mouth, genitals and anus, rash on palms and soles, skeletal abnormalities and watery discharge from nose. Untreated infants can develop blindness, deafness, facial deformities and nervous system problems.
“Recently, we had a case in which a woman was infected during her pregnancy. The patient had an initial negative screen with the rapid plasma reagin (RPR) test for syphilis at 16 week’s gestation,” Dr. Goje notes. “The baby developed a persistent rash, and was diagnosed with congenital syphilis at age 3 months. Radiology confirmed evidence of the congenital infection.”
Advertisement
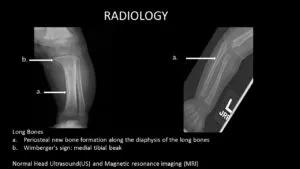
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/e4aa0122-f5cb-4881-be68-be8cacaca598/congenital-syphilis-300x169_jpg)
“Following an intravenous course of penicillin, the infant was stable,” Dr. Goje continues. “As an institution, we revisited our screening practices following this unusual case in which a patient contracted congenital syphilis despite receiving high-quality, standard-of-care prenatal services. Due to the upward trend in STIs in our area, including among pregnant women, we have instituted a second syphilis screen between 28-30 weeks gestation.”
Chlamydia and Gonorrhea
The increasing rates of chlamydial and gonococcal infections are also concerning to Dr. Goje, as these infections are often minimally symptomatic, but can lead to serious complications for newborns and women, including pelvic inflammatory disease, chronic pelvic pain, tubal infertility and ectopic pregnancy. Gonorrhea and or chlamydial infections could increase the risk of HIV acquisition.
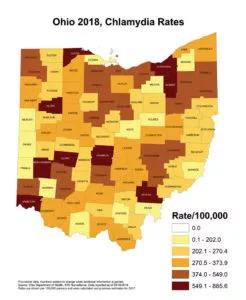
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8720a22c-7b87-428b-bc80-6d8a7ac74fec/19-OBG-1459_CQD-inset-Chlamydia-246x300_jpg)
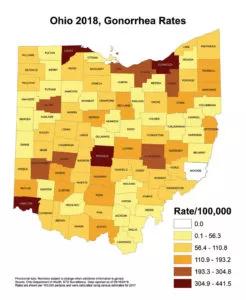
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3ce92e97-1317-487d-aa9e-2d56ff970bdf/19-OBG-1459_CQD-inset-Gonorrhea-246x300_jpg)
Although the infections themselves are treatable, the complications may have long-term impacts on a woman’s health. When detected, these infections are treatable with antibiotic therapy. All sex partner(s) should be treated to prevent re-infection.
“In addition to expanding our prenatal STI screenings, we plan to survey our providers on expedited partner therapy (EPT) for STIs. We hope to provide some education and guidance on how to treat partners to prevent re-infection of our patients,” Dr. Goje says.
Advertisement
Advertisement
Data point to potential for targeted preconception planning
Reproductive psychiatry helps patients balance medication-related risks
Molecular Profiles Help Guide Referral and Care Planning
Hyperthermic intraperitoneal chemotherapy can improve patient outcomes
Leaning into therapies with the strongest evidence
A Q&A with Cleveland Clinic’s board-certified pediatric and adolescent gynecologist
Increasing uptake remains a challenge
Multidisciplinary teams work together in in-situ scenarios