An update with advice for traveling patients
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
After a hiatus of nearly 200 years, chikungunya has returned to the Americas.
In the modern era, chikungunya was first identified in 1952 in Tanzania, where it derived its name from a word in the Makonde language meaning “that which bends up” in reference to the posture often caused by the debilitating pains that attend the infection. In an earlier era (1827-1828), the infection is believed to have swept the Caribbean and is suspected to have been similar to a disease observed on Zanzibar known by the Swahili term kidenga pepo, referring to a cramp-like seizure brought on by evil spirits. Common to all these epidemics is an illness of formidable morbidity caused by a member of the Togaviridae family (also part of the Old World alphavirus group associated with arthritis).
Prior to the current epidemic, these diseases, rare in the West (originating in Australia [Ross River fever], the Pacific, Central Africa [o’nyong-nyong fever] and other locations), were considered curiosities and the subject of questions on board exams. The situation changed dramatically in 2013 when chikungunya was identified on the Caribbean island of Saint Martin and has since swept across the hemisphere.
Chikungunya is a virus maintained in a sylvatic transmission cycle between primates, rodents, bats and other vertebrates that appear to be asymptomatically infected. Chikungunya can be transmitted to humans by mosquitoes of the Aedes genus (aegypti and albopictus species) and then transforms to a human-mosquito-human epidemic.
Advertisement
The infection has been clinically documented in over 1.5 million individuals in the Americas, including a small number of locally-regionally transmitted cases in the U.S. It should be noted that mosquitoes of the Aedes genus are also capable of transmitting several other serious viral infections, including dengue and Zika.
The disease is characterized by viremia, rash, arthralgia, arthritis and myalgia that can be profound and arise rapidly. The fever and rash can resolve over 7 to 10 days, but the particular symptoms can persist in up to 60 percent of patients and may last for several years. The precise spectrum of joint manifestations is still being described, and description is limited by the fact that in most studies from endemic regions, there are few reliable data from microbiologic and pathophysiologic investigations. Regardless, chikungunya can appear as a fulminant disease looking like acute rheumatoid arthritis (see Figure) and should be suspected in any patient returning from an endemic area.
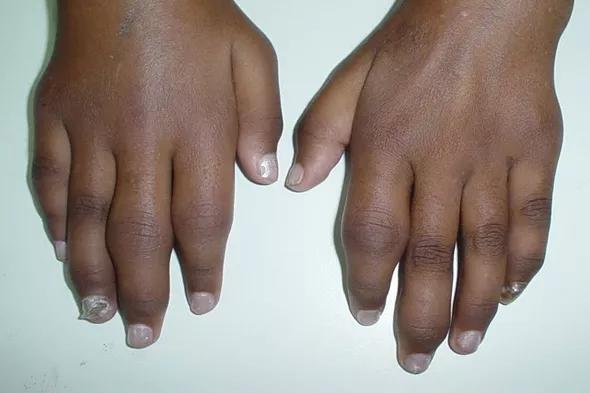
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/838cda1a-7ee1-430b-8d77-0af44abfe96f/15-RHE-2603-Calabrese-Inset-Image-01-590pxl-width_jpg)
Figure. Hands of a patient with chikungunya. Note the resemblance to joints in acute rheumatoid arthritis.
The disease is currently most prevalent in the Caribbean, Central America and Colombia. Until the epidemic subsides, travelers to endemic areas in this region need to be instructed on strict mosquito precautions and advised to be alert to the symptoms of the condition should they become infected.
Recent studies from Washington University (Miner et al, Arthritis Rheumatol. 2015;67:1214-1220) suggest that the underlying mechanisms of joint inflammation are very similar to those operating in rheumatoid disease.
Advertisement
Dr. Calabrese is the R.J. Fasenmyer Chair of Clinical Immunology and Director of the R.J. Fasenmyer Center for Clinical Immunology at Cleveland Clinic.
Advertisement
Advertisement

The case for continued vigilance, counseling and antivirals

High fevers, diffuse rashes pointed to an unexpected diagnosis

No-cost learning and CME credit are part of this webcast series

Summit broadens understanding of new therapies and disease management

Program empowers users with PsA to take charge of their mental well being

Nitric oxide plays a key role in vascular physiology

CAR T-cell therapy may offer reason for optimism that those with SLE can experience improvement in quality of life.

Unraveling the TNFA receptor 2/dendritic cell axis