An historical view of the disease
Editor’s note: This is an abridged version of an article originally published in the Cleveland Clinic Journal of Medicine. The article in its entirety, including a complete list of references, can be found here.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The physical examination findings of infectious endocarditis are known by heart by every medical student who can rattle off Osler nodes, Janeway lesions and splinter hemorrhages without a smart phone in sight. These findings, though famous, are rare, and the more common findings like splenomegaly and subconjunctival petechiae are less readily listed.
To better appreciate the famous and not-so-famous physical examination findings of infectious endocarditis, it’s important to look back at the evolution of the disease.
The understanding of endocarditis evolved rapidly after the disease was put into the forefront of medicine by Sir William Osler in 1885. Dr. Osler placed endocarditis on the medical map with his Gulstonian lecture series on the subject. Before these lectures, infective endocarditis was a known entity, usually diagnosed at autopsy, but no comprehensive information existed on its presentation and natural course. Dr. Osler was the first to synthesize the known data and case reports at that time, presenting it in a cohesive way to better understand the condition. He recognized important aspects of the disease, noting the wide range of clinical presentations, the progression from an acute febrile illness leading to rapid deterioration and death. He also noted that the illness could present over months to years before death, in what would later be called subacute bacterial endocarditis.
Osler also recognized that valvular abnormalities predisposed patients to endocarditis, and that a history of rheumatic fever was common.
Advertisement
In 1899, Edward Janeway, MD, described painless lesions on the palms and soles in patients suffering from endocarditis. His objective in describing these lesions was a viable way for clinicians to differentiate endocarditis from another “malignant process” presenting with fever and weight loss. He described the lesions as “small hemorrhages with slight nodular character in the palms of the hand and soles of the feet.”
In contrast to the painless palmar Janeway lesions, Osler nodes are painful and in the pulp of the fingers and toes, and the two lesions have forever confused medical students and clinicians alike.
Splinter hemorrhages are another physical finding of infectious endocarditis on the fingers. These small, dark, straight lines often at the tips of the fingernails are a notoriously nonspecific finding, seen in clinical scenarios from trauma to sepsis but made famous because their initial description was in patients with endocarditis in the 1920s.
George Blumer, MD, was the first to use the term splinter hemorrhages in 1926 after initially finding them on two patients with endocarditis. He later evaluated 48 patients with endocarditis and discovered the lesions only twice, so it was quickly recognized that they were not a very sensitive marker for endocarditis as they were found in a variety of other conditions. Although famous, the findings on hand and foot examination in endocarditis are rare, found in fewer than 15% of cases.
Emanual Libman, MD, was a key figure in elucidating the more common signs and symptoms of endocarditis, as well as introducing blood culture as a diagnostic tool in the United States. With blood cultures, physicians had a new tool to help recognize endocarditis earlier, and the opportunity to recognize more clinical symptoms associated with endocarditis at an earlier stage.
Advertisement
Dr. Libman wrote extensively on the signs and symptoms of endocarditis, recognizing the characteristic murmur, fever, splenomegaly, anemia and transient petechiae (commonly subconjunctival). Perhaps Dr. Libman is best known for his description of noninfectious vegetations in patients with lupus erythematosus, alongside Benjamin Sacks, MD.
A cynic might question the importance of diagnosing endocarditis earlier in the era where antibiotics were still decades away. But it’s important to note that even as progress was being made in microbiology and the recognition of endocarditis was becoming more widespread, it was still a universally fatal condition.
While the early 20th century brought about increased recognition and understanding of infective endocarditis, it was not until the early 1940s with the implementation of penicillin that there was an effective treatment. In 1944, the first published report of the use of penicillin demonstrated a near 75% resolution of disease. For the first time, endocarditis was a potentially treatable disease. Clinicians could use their diagnostic acumen to diagnose a fatal condition, implement a therapeutic agent and potentially save the patient.
The development of penicillin quickly changed how the disease was viewed, and the decades of work detailing the diagnostic clues paid off, as patients could be appropriately diagnosed and effectively treated.
Advertisement
Advertisement

Emerging evidence suggests a patient-specific approach

Not if they meet at least one criterion for presumptive evidence of immunity

Essential prescribing tips for patients with sulfonamide allergies

Confounding symptoms and a complex medical history prove diagnostically challenging

An updated review of risk factors, management and treatment considerations
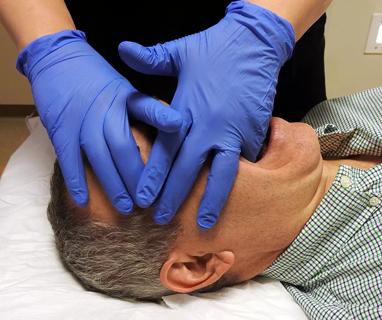
OMT may be right for some with Graves’ eye disease

Perserverance may depend on several specifics, including medication type, insurance coverage and medium-term weight loss

Abstinence from combustibles, dependence on vaping