Illustrated case series profiles a valuable tool for a rare and complex entity
Patient-specific 3D-printed models are immensely helpful for comprehensive anatomical assessment, presurgical planning, and patient education in the setting of isolated primary tricuspid valve (TV) disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
That’s the conclusion of a new image-rich case series published by a Cleveland Clinic team in JACC: Case Reports (2020;2:2217-2222).
The article features case vignettes of four patients who recently underwent successful surgical repair for primary TV disease at Cleveland Clinic, with each surgery guided by a patient-specific 3D-printed TV replica (Figure). The replicas were generated from 3D transesophageal echocardiography and contrast-enhanced 4D computed tomography. Three of the four patients had severe tricuspid regurgitation, and one had severe tricuspid stenosis. Surgical results were excellent in all patients.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8541d293-019f-4434-b391-662673d1101c/20-HVI-2006254-Image-of-Issue-3D-printing-in-tricuspid-valve-disease-Inset-1_jpg)
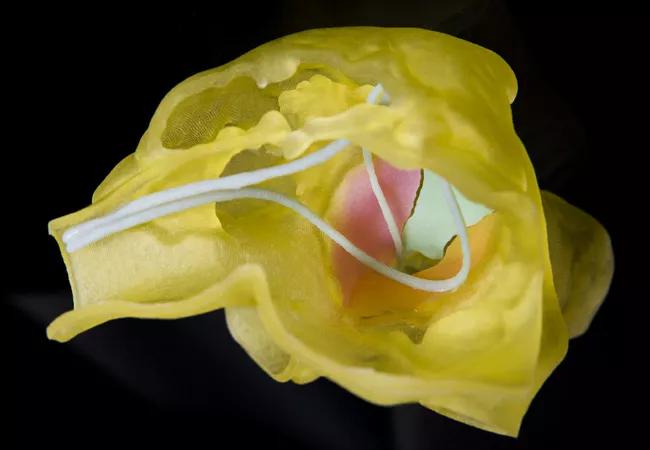
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/00d5f426-bbbd-4743-af0d-9403fbd10ade/20-HVI-2006254-Image-of-Issue-3D-printing-in-tricuspid-valve-disease-Inset-2_jpg)
Figure. 3D-printed anatomic replicas from two patients in the case series. The top panel shows the tricuspid valve (in green) printed in systole in a 66-year-old woman with severe tricuspid regurgitation with prolapse of the topmost valve leaflet. The bottom panel shows the tricuspid valve and pacemaker leads visualized from the right atrium in a woman in her 20s with severe tricuspid stenosis. The patient had a dual-chamber pacemaker for the treatment of congenital complete heart block. The case series features photos of all four cases, along with 3D echo and 4D CT images used to generate the replicas and intraoperative photos of the corresponding anatomy.
“Isolated primary tricuspid valve disease is a rare entity, as it accounts for about 10% of all cases of tricuspid regurgitation,” says the publication’s lead author, Serge Harb, MD, of Cleveland Clinic’s Section of Cardiovascular Imaging. As a result, experience with surgical repair of primary TV disease is limited, which makes imaging-based preoperative planning critical. “However,” adds Dr. Harb, “the complexity of the tricuspid valve anatomy — such as its position in the chest, its thin and variable leaflets, and shadowing from device leads — often makes accurate imaging of the disease a challenge.”
Advertisement
That’s where 3D-printed models — developed with high-spatial-resolution cardiac imaging and advanced image-processing software — prove valuable, as they provide a more-detailed analysis of the TV leaflets and an accurate depiction of the TV annulus and right ventricle morphology.
“Surgery for isolated tricuspid valve disease carries a postoperative mortality rate of up to 8.8% in the Western world,” notes Cleveland Clinic cardiothoracic surgeon Per Wierup, MD, PhD, a co-author of the case series. He adds that the operative complexity and long extracorporeal circulation times heighten risk of vasoplegia and coagulopathy in particular. Underlying right ventricular and liver and/or kidney dysfunction in cases with late presentation also raise the risk of postoperative multiorgan failure.
“The enhanced visualization and anatomic understanding to be derived from 3D-printed models help us optimize our presurgical plan, customize the operation to the patient’s unique anatomy, anticipate potential complications, and reduce operative and extracorporeal circulation times,” adds. Dr. Wierup. “This substantially reduces the risks for our patients.”
In all four cases, the cardiologist and surgeon shared the 3D-printed model with the patient preoperatively to explain their valve disease and to illustrate the expected repair. “All the patients expressed a greatly improved understanding of their disease and the planned operation,” notes Dr. Harb. “Beyond helping us plan the operation, 3D-printed models can greatly enhance patient education and potentially ease patient anxiety about their procedure.”
Advertisement
To view the illustrated case series, click here.
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more